Problems mount with coronavirus testing, limiting access and sowing confusion
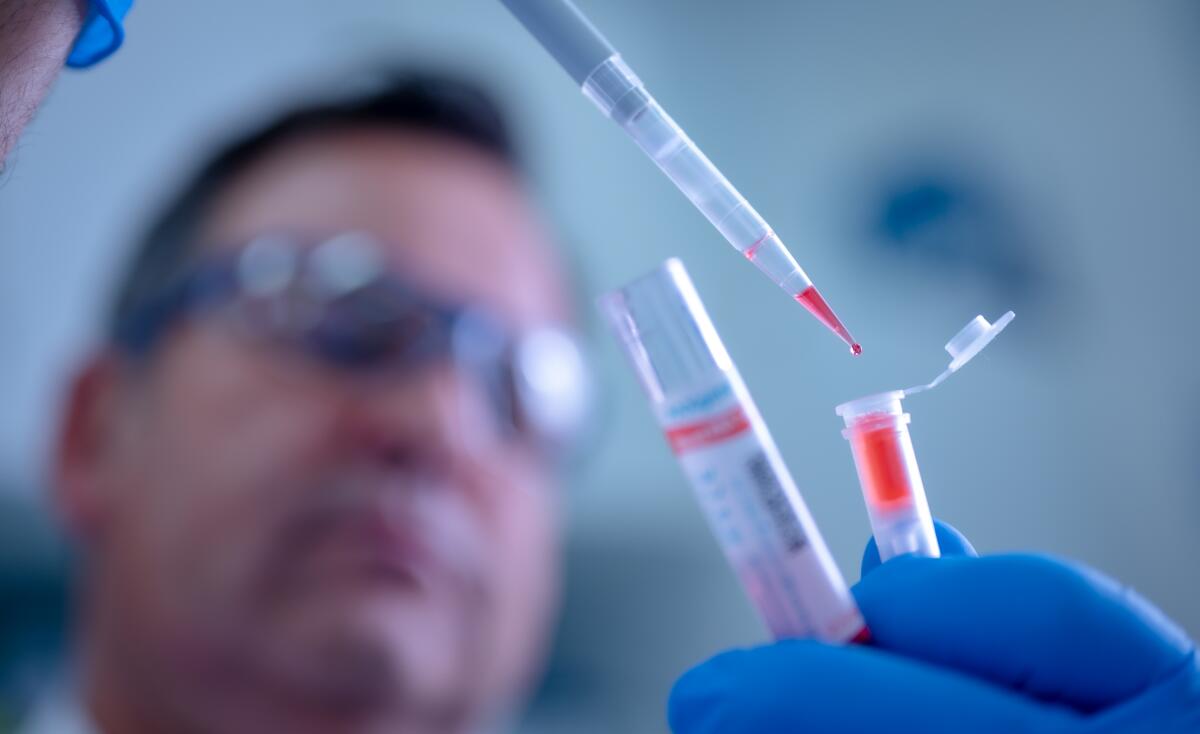
Testing for the novel coronavirus continues to face severe limitations, as California health officials lack key components to conduct laboratory analysis, marking another barrier in the state’s efforts to identify infectious patients.
The shortfall compounds a month of sluggish progress in deploying diagnostic tests developed by the federal Centers for Disease Control and Prevention and, if not quickly remedied, will continue to substantially undercount infected patients and could hinder efforts to contain the outbreak.
“This is imperative that the federal government and labs across the United States, not the state of California, get the benefit of all the ingredients that are components of the test,” Gov. Gavin Newsom said Thursday. “I am surprised this is not more of the national conversation. We need to focus in on these tests.”
The chemicals needed, known as reagents, are used to extract genetic material from a nasal swab sample, among the first steps in the testing process. Demand for reagents has left a key supplier struggling to keep pace with orders from countries around the world.
The new information provides a clearer picture of why testing shortages continue, even as state and federal officials last week insisted there were sufficient kits. Newsom said that without the needed supplies, the “test kits are like printers, but without ink.”
News about the novel coronavirus is moving quickly.
In California, only 1,138 people had been tested for the virus in public health labs as of Wednesday, despite several thousand who have likely been exposed to infected patients. Newsom said the reagent shortage had contributed to a state backlog in testing and that the administration had “been very aggressive with the CDC” in demanding more reagents.
“We have 7,675 tests available, but not every one of those tests can be accessed, because all the ingredients are not available at all of the labs,” he said. Up to 200 samples could be backlogged, he said.
A spokesman for Qiagen, a top supplier of the reagents, said the pandemic was “challenging our capacity to supply certain products” and that it would increase production in facilities in Germany, Spain and Maryland. The company will also hire additional employees and adjust staffing to cover three shifts, working seven days per week.
“This is a period of extraordinary demand,” said Thomas Theuringer, a spokesman for the company.
Wet markets are more vital now than ever. But wildlife regulation is an issue.
The absent reagents are only the latest problem to befall the nation’s bungled rollout of COVID-19 test kits. States have grappled with delays in receiving kits from the CDC while also struggling to rapidly increase staffing and equipment in labs to keep up with the growing number of people falling ill.
“The testing issue continues to haunt us in many ways,” L.A. County Public Health Department Director Barbara Ferrer said in a press briefing Wednesday. “We are very dependent on getting reagents from the CDC. I know both the president and the vice president were assuring us and the general public that those reagents are coming and coming quickly.”
“If we don’t get reagents soon, that will become a problem for us,” she added.
Nationally, a sharp drop in tests reported to the CDC may reflect the ongoing problems with component shortages. Daily testing over the five-day period ending Tuesday fell from 1,246 to only eight, according to the CDC. The figures include tests from the CDC as well as public health labs.
The statistics stand in stark contrast to other figures from the Trump administration. The CDC on Monday announced that 78 public health labs across the country had the capacity to test 75,000 people. Alex Azar, secretary of the Department of Health and Human Services, told Congress on Tuesday that national lab capacity could increase to 10,000 to 20,000 tests per day by the end of this week.
The CDC did not respond to requests for comment seeking clarification of the statistics.
The component shortages could also limit the testing capacity of commercial and academic labs, even as the availability of test kits increases, say experts.
“Increased demand for testing has the potential to exhaust supplies needed to perform the testing itself,” including reagents, plastic pipette tips, and other products, the American Society for Microbiology said in a statement.
The testing situation “gets worse every minute,” said Marc Lipsitch, a professor of epidemiology at the Harvard T.H. Chan School of Public Health.
Newsom called the Trump administration’s claims surrounding test availability a “communication challenge.” They’re “claiming they have tests, but then you talk to local officials, who say, ‘Well, we don’t.’ ” He added that it “would be very helpful” if the White House’s coronavirus task force communicated that technicality “with more clarity, so that we, at the local level, can do the same for people trying to access those tests.”
California officials are working with private commercial lab partners like Quest to deal with testing backlogs.
COVID-19 response issues have trickled to L.A. County, where health officials on Wednesday confirmed the first coronavirus-related death and six new cases, bringing the county’s total to 28.
County officials are currently limiting testing much more than the CDC recommends, due to a lack of available tests. The CDC says any doctor can order testing for a symptomatic patient. But in an advisory sent to doctors Wednesday night, L.A. County officials said they were “recommending that lab testing be restricted to individuals with severe disease.”
“When widespread community transmission becomes apparent, then testing strategies will be reassessed and possibly revised,” the advisory reads.
The county’s lab had tested 100 people so far and the CDC had tested another 27 L.A. County residents, Ferrer said. One hundred and twenty people have been tested by the two commercial labs in the county, she said.
The county lab, which houses only one testing machine, has the capacity to test 30 people per day. Two additional machines have been ordered, she said. However, the lab is already running up to 18 hours per day, and workers are stretched thin.
A 32-year-old New Jersey man was hospitalized with COVID-19. His Twitter video, viewed half a million times, caused concern among younger people.
“We’ll also face an issue of getting more employees to run more tests,” Ferrer said.
Ferrer said Quest and LabCorp, in addition to the local public health lab, are running tests. The county Department of Health Services, which manages public hospitals, is working to get a lab up and running that would be able to collect specimens and also process the test.
“I do think it’s important to be able to increase our capacity when clinically appropriate to be able to test [symptomatic] people,” she said. “We need to have more testing capacity. I’m glad we’re trying to build that capacity.”
In Sacramento County, the shortage has complicated efforts to test patients at a nursing home facility in the suburb of Elk Grove, where an elderly patient died this week. Peter Beilenson, the county’s health director, said Tuesday that the county has access to only 20 tests per day and is having to ration those between possible cases in the community and medical professionals who may have been exposed.
Commercial labs can test milder patients, according to county officials, but many hospitals are still using only the official county lab, restricting who can be tested for the virus.

The WHO has officially declared the coronavirus a pandemic. This is the first pandemic caused by a coronavirus. Infectious disease physician Timothy Brewer of UCLA compares the novel coronavirus to other pandemics, like H1N1, MERS, SARS and influenza.
At hospitals, physicians say they are increasingly requesting COVID-19 testing due to community transmission in California. Calls for testing are sent up a chain of command and often denied, they say, or are dragged out for up to a week, as patients return to their communities.
“The bottom line is that there’s community transmission. You can’t really use a travel screen to screen patients,” said an internal medicine physician who works at an L.A. hospital and was not authorized by her institution to speak. “We need to be testing more people ... as this grows, what’s going to happen?
“It’s just tough. I think this is kind of an unprecedented situation here,” she said.
Staff writers Tony Barboza, Anita Chabria, Tom Curwen and Taryn Luna contributed to this report.
More to Read
Start your day right
Sign up for Essential California for news, features and recommendations from the L.A. Times and beyond in your inbox six days a week.
You may occasionally receive promotional content from the Los Angeles Times.