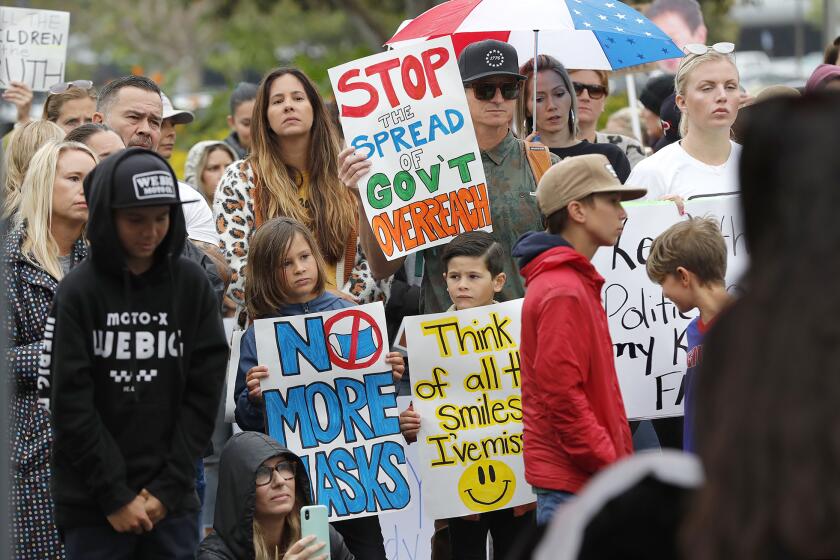Commentary: The challenge of treating an addiction epidemic during a global pandemic

- Share via
When my colleagues and I first heard of the novel coronavirus, not much, if anything, changed. We knew that the virus was causing severe illness and death in an older population because that’s what was mostly being reported. Initially, previous outbreaks like H1N1 in 2009 and Middle Eastern Respiratory Syndrome (MERS) in 2012 came to mind. We’ve worked through them before, so I figured we’d work through this. Then, a few weeks later, the coronavirus was declared a pandemic, and lockdowns and curfews were instated.
When the team and I realized that this virus was much more serious than originally believed, we held a meeting and asked ourselves, “What does this mean for us?” We had no knowledge on the coronavirus, and the information we did have changed almost daily, so we had very few hard and fast rules to establish protocols from. How will we treat patients? What’s the best way to keep everyone safe? What other guidelines will we have to put in place? Are we essential workers? Will PPE be available for us?
We as addiction treatment providers were not placed high on the list of healthcare workers, which was somewhat surprising to me. We now know through many reports that people with substance use disorders have a higher likelihood of catching the virus due to substance abuse itself, the medical issues often accompanying their addiction and living conditions that make them more susceptible to the disease in general. Despite that information, the fact that we were treating patients who had been discharged from emergency rooms after overdosing and the country was experiencing substantial rise in the number of people addicted to opiates, we still had to make the argument that we were deserving of PPE.
We ended up being much more fortunate than others. I was in charge of gathering the supplies needed to be able to treat our patients, and each day I prayed that we’d be able to get through the day as safe as we could with the equipment we had. Everything about our job defined us as essential workers, but it took some time for others to see it that way.
We also encountered another roadblock: vaccine administration. By the time the vaccine was available, it was widely reported, and an undeniable fact, that addiction and mental health issues had skyrocketed during the pandemic. Still, we could not sign up to receive the vaccine because addiction and behavioral health providers were not on the priority list of healthcare workers.
Many people have a preconceived notion of what an addict looks like — that the people we treat are “just addicts,” and that perception was embedded in many more people than we thought. I was personally asked a question that I think many thought but didn’t ask out loud: “Why do you continue to go to work every day and risk your health to treat people who aren’t adequate contributors to society?” I am still as shocked by the absurdity as I was the first time the question was posed. How dare we decide who’s worthy of living? Not only is this a gross generalization, but no medical professional or healthcare provider on the planet would have thought for a millisecond that treatment for COVID-19 should be based on societal contributions. Why in the world would that metric be applied to addiction treatment? The notion itself is vile.
Hundreds of parents and children rallied outside the Costa Mesa office of the Department of Education Monday to protest mandates requiring children to remain masked at school.
While we may not be in the emergency rooms and ICUs, the treatment and care we provide our patients is just as valuable and necessary. Through our work, a mother somewhere was able to sleep peacefully for the first time in a long time knowing that her son or daughter was safe and receiving treatment. An entire family who had their lives completely upended after a parent relapsed felt the comfort of knowing that a return to some sense of normalcy was a possibility.
Treating the disease of addiction during the pandemic has been physically, emotionally and mentally taxing on all of us addiction nurses and providers, and the same is true for just about every healthcare professional. I became a nurse because I wanted to help save people and improve their lives, and I can confidently say I was given that opportunity many times over during the pandemic.
I’ll say this about COVID-19: after enduring the last year, I have never been more proud to be an addiction nurse. Aside from having children, providing treatment to patients and their families during this time is the most selfless thing I’ve ever done, and I know my nurses share that same sentiment. Even though it’s been hard, heartbreaking and lonely, it has been incredibly rewarding to impart even the smallest amount of change to a person and their family. That’s exactly what nursing is about — giving of yourself for the betterment of someone else. It’s about helping people heal, improving their lives, and at times, actually saving them. Providing addiction treatment in the midst of a national epidemic and a global pandemic has been one of the most challenging times of my career, but at no point have I ever been more proud of what I do every day.
Lynnette Mitchell, RN, is the Director of Nursing at Laguna Treatment Hospital in Aliso Viejo.
All the latest on Orange County from Orange County.
Get our free TimesOC newsletter.
You may occasionally receive promotional content from the Daily Pilot.