Study: Pregnant women with COVID-19 are 10 times more likely to die, but few are getting vaccine

- Share via
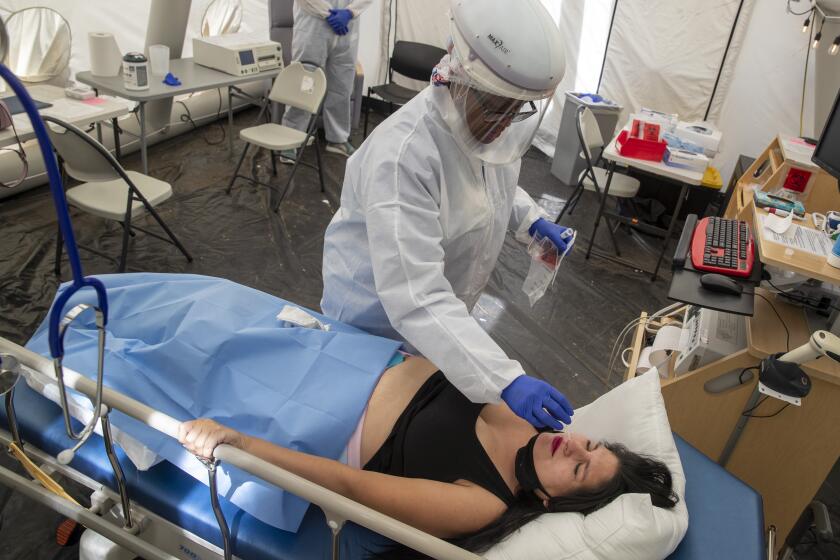
Women’s health specialists are urging pregnant women to get vaccinated, after a study found those who become infected with the virus are more likely to deliver prematurely, require intubation or mechanical respiration and die in childbirth.
Published in the American Medical Association’s JAMA Network Open, the study looked at the health outcomes of 869,079 women who delivered in university-based hospital systems between March 1, 2020 and Feb. 28, including 18,715 flagged in a national database as having been infected with COVID-19.
Infected patients were 40% more likely to deliver prematurely and were admitted into hospital intensive care units at a rate six times higher than non-infected patients, the study found.
During childbirth, about 5.2% of COVID-19 patients required intubation and mechanical ventilation, compared to .9% of their counterparts, and were 10 times more likely to die in the hospital, data indicated.
The number of pregnant women becoming infected with COVID-19 in Los Angeles and Orange counties has increased in the last few weeks, officials report.
Dr. Jennifer Jolley, an associate professor of maternal and fetal medicine in UCI Medical Center’s OB/GYN department, co-authored the study as part of a team that included UCI Health surgeon Dr. Ninh T. Nguyen. In an interview Thursday, she said the findings confirm what obstetricians have been seeing among their own patients.
“We actually don’t know that pregnant women are more likely to get COVID-19,” Jolley said. “The issue is those who do get it are more likely to have the severest manifestation of [the disease] — if they get it, they get sicker than women who are not pregnant.”
And because expectant mothers pass along vital nutrients and oxygen through the placenta, maternal respiratory weakness and failure — hallmarks of the disease — can threaten fetal health.
Jolley said doctors may decide to deliver a baby before it has come to term so it can be hooked up to a machine that will provide adequate oxygen, instead of forcing it to rely on a compromised uterus.
“If that system is broken, then the fetus is at risk,” she said.
The study also found patients with COVID-19 were more likely to be Black or Latina, compared to uninfected patients, and pointed out racial disparities in maternal health, due to discrimination, health care access and a disproportionate burden of underlying comorbidities that have likely been augmented by the pandemic.
Medical experts say there’s no evidence that any vaccination, including the COVID-19 vaccination, influences your chances of getting pregnant.
Data collection took place before COVID-19 vaccines were widely available to the public. Jolley said obstetricians, lacking evidence on the potential impacts of a vaccine to an expectant mother or fetus, initially supported a pregnant woman’s choice regarding vaccination.
But now, things are different.
The CDC earlier this month reported that data from three safety monitoring systems found no safety concerns for pregnant people vaccinated late in pregnancy or their babies, including no significant increased risk of miscarriage or infections.
“The benefits of receiving a COVID-19 vaccine for pregnant people outweigh any known or potential risks,” CDC officials stated in an Aug. 11 release.
“The increased circulation of the highly contagious Delta variant, the low vaccine uptake among pregnant people and the increased risk of severe illness and pregnancy complications related to COVID-19 infection…make vaccination for this population more urgent than ever,” the release continued.
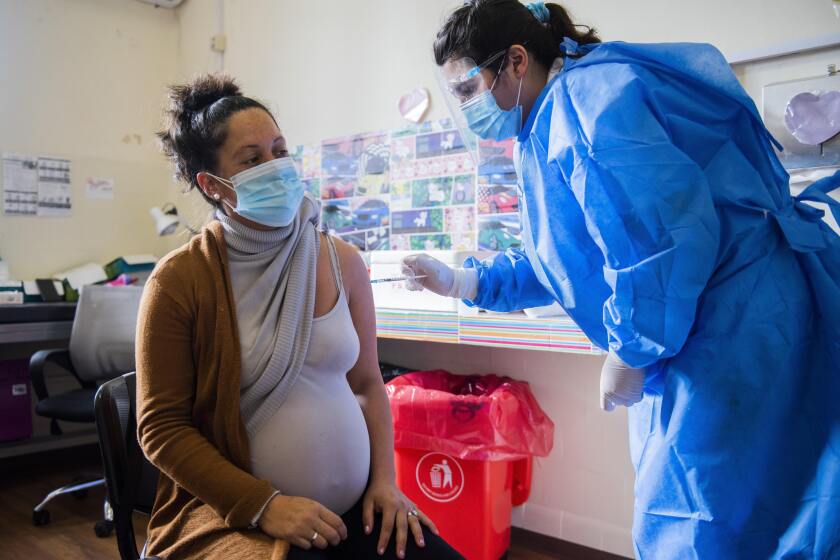
Despite the increased risk COVID-19 presents during pregnancy, Jolley noted CDC figures from mid-August showed only 23.8% of pregnant women had been vaccinated — far below the nearly 71% of all eligible Americans who’ve received at least one dose.
“When I see a number like 23.8%, that means to me I have 76.2% of my patients still to counsel,” she said, acknowledging a high level of hesitance about the vaccine among pregnant women.
Because there is no ideal point in one’s pregnancy to get vaccinated, Jolley recommends her patients get inoculated as soon as possible. In addition to possibly saving their own lives, they can build antibodies that can be shared with a fetus in utero or, later, through breast milk.
“I want them to get the vaccine as soon as they can moving forward, for their health and for the health of their family,” she said.
All the latest on Orange County from Orange County.
Get our free TimesOC newsletter.
You may occasionally receive promotional content from the Daily Pilot.