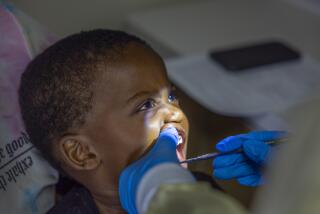
More children are keeping their tonsils
About a year ago, Jamie’s older sister began complaining about the then 3-year-old’s loud snoring. Because Jamie’s tonsils seemed enlarged, her parents took her to an otolaryngologist at Childrens Hospital Los Angeles, who confirmed that the tonsils were indeed large for a child of her age and size.
Several decades ago, such an observation would have been enough to immediately proceed with surgery. Before antibiotics were developed, most physicians thought that removing the tonsils could prevent severe, recurrent infections of the throat and ear (as well as a number of other ailments), so few children got out of school with their tonsils intact. A study of 1,000 New York schoolchildren in 1934 found that 61 percent had already had their tonsils removed; teams of doctors who examined the remaining children recommended tonsillectomies for all but 65 of them.
Even after the development of effective antibiotics, the belief persisted that tonsillectomy was necessary for most children. During the 1970s it was the third most common surgical procedure performed in American hospitals. Some doctors, however, began to evaluate the indications for tonsillectomy. In 1978, an expert panel convened by the National Institutes of Health concluded there was not enough scientific information available to know if the potential benefits of tonsillectomy outweighed the potential risks. The panel recommended more research on the subject.
That research and the subsequent guidelines based on it have resulted in a dramatic decrease in the number of tonsillectomies performed in the United States. Today, tonsillectomy should be considered only when strict medical guidelines are met. The American Academy of Otolaryngology-Head and Neck Surgery (the professional society for ear, nose and throat specialists) published guidelines in 2000 listing the following indications for tonsillectomy in children:
Three or more infections of the tonsils in a year.
Enlargement of the tonsils causing obstruction of the upper airway, difficulty swallowing, sleep disorders, or heart or lung disease.
Enlargement of the tonsils causing dental problems or abnormalities in the growth and development of the mouth and face.
A severe infection (abscess) in or next to the tonsils that does not respond to medical treatment.
Persistent foul taste or breath due to inflammation of the tonsils that does not respond to medical therapy.
The persistent presence of a specific bacterium, Streptococcus, in the tonsil that does not clear with antibiotics.
- A marked enlargement of only one tonsil, which might be a sign of cancer.
In Jamie’s case, because there were no breathing difficulties, her doctor decided an operation was not necessary. He thought that it was possible that the tonsils might shrink as Jamie grew and that the snoring might become less of a problem.
However, Jamie’s symptoms got significantly worse. Although she had no difficulty breathing while awake, she sometimes seemed to struggle for breath when sleeping. (Obstructed breathing occurs during sleep because the muscles of the throat relax, allowing the tonsils to fall together and block the airway.) Because of her breathing difficulty, she began waking up many times each night, which left her drowsy and cranky during the day.
A recent visit to her doctor revealed extremely large tonsils (see picture). Because of her nighttime breathing problems (diagnosed as obstructive sleep apnea), the doctor recommended, and performed, a tonsillectomy.
As with any operation, the procedure is not without risk. Tonsillectomy requires general anesthesia, and may be complicated by postoperative bleeding in about 2 percent to 3 percent of patients. Nearly 10 percent of children become significantly dehydrated after surgery because of pain that makes it difficult for them to drink and eat. Rarely, a child must be readmitted to the hospital for treatment of these complications.
(A new procedure called temperature-controlled radio-frequency tonsillar reduction is undergoing evaluation and may reduce the complication rate; instead of removing the tonsils surgically, several needles are inserted into the tonsillar tissue and a radio-frequency energy is administered which will shrink it over time, about four to six weeks.)
How did Jamie fare with her tonsillectomy? According to her surgeon: The operation was uncomplicated, and Jamie’s postoperative course was fairly typical. She complained of severe throat pain for the first four or five days; difficulty swallowing and earaches for the next four or five days; and seemed unusually lethargic for nearly a week.
According to her parents (one of whom co-writes this column), the operation was well justified: Jamie now sleeps through the night without awakening, and remains alert and highly active throughout the day. According to her older sister, the operation was a great success: Jamie no longer snores. According to Jamie, 10 days of ice cream made it all worthwhile.
Dr. Jonathan Fielding is the director of public health and the health officer for the Los Angeles County Department of Health Services. Dr. Valerie Ulene is a board-certified specialist in preventive medicine practicing in Los Angeles.
More to Read
Get the L.A. Times Politics newsletter
Deeply reported insights into legislation, politics and policy from Sacramento, Washington and beyond. In your inbox three times per week.
You may occasionally receive promotional content from the Los Angeles Times.