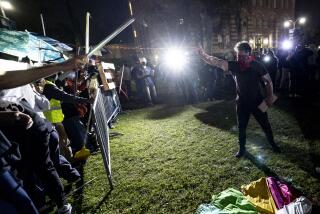Better Pay Lures Doctors Away
The 4-year-old’s blood pressure was falling when she landed in the intensive care unit of a Fresno hospital last week. Her breathing was shallow; she was on the verge of cardiac arrest.
“She had a huge tumor in her abdomen the size of a baseball wrapping around the big vein and artery in her belly,” said Dr. Robert Dimand, a pediatric critical care specialist at Children’s Hospital Central California in Fresno.
Dimand and other physicians administered chemotherapy to shrink the tumor, and then dealt with complications from the chemo. The girl survived, but Dimand is guarded about her prognosis.
He is also cautious about the future of the program that he thinks helped to save her life: California Children’s Services, or CCS, which provides gravely ill children and teenagers state-of-the-art medical treatment, no matter the expense. About 170,000 youngsters with from cancer, cerebral palsy, cystic fibrosis, congenital heart problems, HIV and other ills were treated through the CCS program last year at 13 facilities across the state.
Last week, however, the budget signed by Gov. Gray Davis imposed a 5% cut in the money that doctors are paid to treat CCS patients. The state’s annual budget for CCS is roughly $135 million.
But health advocates worry that the reimbursement cuts could hurt the program by furthering the flow of skilled pediatricians who have left California in recent years for more lucrative jobs elsewhere. The expected result: longer waits to see the doctors.
It’s already often a three-month wait to see a kidney specialist at UC Davis Children’s Hospital, said doctors at the facility. At UCLA Mattel Children’s Hospital, it takes children four to five months to see a neurologist, said Dr. Juan Alejos, director of the pediatric heart transplant program at UCLA Mattel Children’s Hospital. “It’s not acceptable,” he said.
In most cases, CCS patients are from low-income families who have no insurance or rely on Medi-Cal, the state health-care program for the poor. But CCS also pays for the treatment of any child whose medical bills are 20% more than a family’s annual income.
Some well-to-do families have found themselves in need of CCS because some medical procedures or treatments are not covered by private health insurance or their costs can quickly soar over the limits of policies -- even when those limits are $500,000 or $1 million.
The cuts were an unfortunate but necessary way to help reduce the state’s budget, said Dr. Maridee Gregory, who oversees CCS as chief of the children’s branch of the state Department of Health Services.
“We’re hopeful the economy will turn around and the state will turn around and pull itself out of this difficult position,” said Gregory. “I hope that pediatricians hang with us and realize that these are needy children and they need the care.”
Most doctors see CCS patients as part of a larger practice. The less money their medical groups receive from CCS, the less the groups have to hire doctors.
Alejos, at UCLA Mattel Children’s Hospital, said a recruiter from outside California recently called him and asked him to name a salary range. Alejos suggested a salary between $150,000 and $200,000. He said his present salary is barely above $100,000.
The recruiter laughed, then suggested that Alejos could command twice that much. Nonetheless, Alejos chose to stay because he likes his job.
At Oakland Children’s Hospital, however, seven physicians have left in the last year -- four to out-of-state jobs. Most of those Oakland jobs remain unfilled. The hospital has also been trying unsuccessfully for two years to recruit a pediatric dermatologist, but salary remains an issue, said Dr. Leonard Kutnick, a pediatrician at the facility.
At Children’s Hospital San Diego, pediatrician Dr. Erin Stucky said she’s watched a steady stream of colleagues depart for reasons that include salary, quality-of-life issues and cost of living.
“We had a cardiologist leave three months ago to go to the Midwest,” she said, “and another is leaving. There’s an ear doctor who left and a neurosurgeon who left for Florida a month ago.”
Dr. Stuart Siegel, director of the children’s center for cancer and blood diseases at Children’s Hospital Los Angeles, worries that one of the hallmarks of CCS -- a team approach to patient care by doctors -- could be compromised by vacancies.
For many CCS children, “it’s life or death. You either do it right or the result ends up bad,” Siegel said.
As jobs are left empty, Siegel and other doctors predict that the caseload for CCS will increase as the state’s population grows.
They argue that CCS is the best safety net for families who find their world suddenly turned upside down by a devastating childhood illness.
In May 2000, Alexandra Stoffel woke up in her Sacramento home and couldn’t walk. At the time, she was 6 and had been having severe backaches. She was soon diagnosed with a Ewing sarcoma, a tumor wrapped around her spinal cord.
She would require chemotherapy and four operations, plus MRIs, specialized care, piles of medications and seven months in the hospital.
“We had our one nice child heading into yuppie land and bam! -- this happened,” said Alexandra’s mother, Laurie Stoffel. “You should have seen the faces on all the other parents. They were thinking, ‘My God, it can’t happen to us.’ ”
The Stoffels’ medical bills eventually climbed to more than $1 million, including $673,000 beyond their private insurance coverage. But within 72 hours of Alexandra’s diagnosis, a social worker at the hospital had told the family about CCS. The state program picked up the tab for most of her care.
Laurie Stoffel quit her job as an attorney to care for her daughter. The family relied on her husband Richard’s income as a legal consultant in Sacramento.
In the fall, they moved to a single-story home to accommodate their daughter’s wheelchair.
Alexandra is now 10. She still can’t walk, but she’s cancer-free and participates in an adaptive ski program and plays golf and tennis.
“The CCS people told us our job was to focus on her care,” said Richard, 41. “Their job was to focus on the rest.”
More to Read
Start your day right
Sign up for Essential California for news, features and recommendations from the L.A. Times and beyond in your inbox six days a week.
You may occasionally receive promotional content from the Los Angeles Times.