DIY or die: How an Australian outback nurse diagnosed his own heart attack and saved his life
For a nurse in one of Australia’s most remote corners, it is DIY or die.
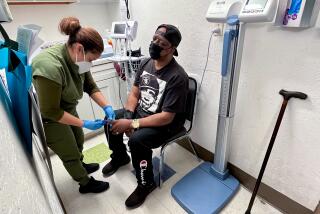
Alone at his station, more than 600 miles from the city of Perth and 100 miles from any hospital at all, the 44-year-old man experiences a sudden bout of dizziness and severe chest pain.
What he does next is remarkable, life-saving and — to a considerable degree — instructive.
He hooks up electrical leads to his upper body, records a heart-rhythm graph and sends it over a phone line established in 2012 to bring medical care to Australia’s remote hustings.
Hundreds of miles away, emergency physicians pore over the spikes and spindles of his electrocardiogram to confirm that a clot — probably a breakaway blob of fatty plaque — has likely lodged itself in his right coronary artery.
With its supply of oxygenated blood constricted, the nurse’s heart had fired off a volley of erratic and dangerous electrical signals.
His pulse is racing, and his life is very much in danger.
A second electrocardiogram, sent by the nurse 50 minutes later, confirms his dire situation. Sinus tachycardia — runs of rapid-fire heartbeats — suggests the vessel has gone from partially blocked to completely blocked.
In other words, things are bad, and getting worse.
If blood flow to the heart is not restored very soon, the result will likely be a barrage of lethal heart rhythms, according to Dr. John Osborne, a cardiologist at Dallas Cardiovascular Center and a volunteer for the American Heart Assn.
Once those runs begin, Osborne says, the nurse’s likelihood of dying rises by 10% with every minute that blood flow remains blocked.
If the patient survives, Osborne adds, the scarring and damage to his heart muscle will likely weaken it — increasing the prospects that his heart will fail before too long.
But the patient is undaunted.
He sinks an IV line into his own arm, chews a full-strength aspirin, and puts himself on a trio of first-line medications for heart attack: a tablet of the anti-platelet drug clopidogrel (known commercially as Plavix), a dose of nitroglycerine under the tongue, and an IV bag of the blood thinner heparin.
Then, he assembles a McGyver-esque toolkit of emergency cardiology medicines.
There’s a clot-busting drug called tenecteplase, which is in limited use nowadays as cardiologists make wider use of clot-retrieval devices in hospital cath labs. Syringes of adrenaline, atropine and amiodorone are prepared to stimulate and stabilize the faltering currents of a heart muscle starved of oxygen. An opioid pain medication is added to the mix, because things could go south in a hurry.
Finally, the ailing man attaches defibrillator pads to his own chest, ready to shock his heart back into rhythm if that becomes necessary.
But then a reprieve: The tenecteplase, a so-called thrombolytic drug bioengineered from the ovarian cells of Chinese hamsters, seems to have succeeded in dissolving the clot. There was only a 50-50 chance that this would work.
Even better: The nurse has not suffered bleeding in the brain, the drug’s most fearsome side effect. This occurs in 5% to 7% of patients and can cause a potentially devastating stroke.
“Do not try this at home, kids,” warns Dr. Osborne.
He notes that patients living within a two-hour drive to a hospital will more likely have their electrocardiogram read while they’re en route in an ambulance, and have their plaques removed by a clot-retrieving device rather than dissolved with tenecteplase. Even in remote parts of the United States, emergency medical technicians, emergency physicians and cardiologists are devising ways to speed the clearance of coronary arteries blocked by clots and plaques.
But the Australian nurse’s speed and resourcefulness can be inspirational to the rest of us, Osborne says.
Know your family history and minimize your risks by quitting smoking and treating high blood pressure, worrisome cholesterol and diabetes.
When you suspect something’s wrong (or have any of these symptoms), don’t wait.
“If you have chest pain, call 911,” Osborne says. “Get it done. You make the wrong call, you die.”
Follow the Australian nurse’s example and chew a full-strength aspirin (325 milligrams). This is a recommended first step for patients who believe they’re suffering a heart attack.
Driving home the urgency of acting quickly on heart attack symptoms, Osborne offers these facts:
• In half of men and two-thirds of women, the first symptom of heart disease is death.
• In 2018, strokes and heart attacks will account for 40% of deaths in the United States — and closer to 75% of deaths among those with diabetes.
• Someone in the U.S. will die of stroke or heart attack every 40 seconds.
How does the nurse’s story end?
He lives to be airlifted by the Royal Flying Doctor Service to a cardiology unit in Perth. There, cardiologists confirm severe narrowing of his heart’s mid-right coronary artery and mild left ventricular systolic dysfunction.
A stent — a tiny device that opens the patient’s occluded artery — is threaded to the spot of bother and deposited there to keep it open. A mere 48 hours later, the man returns to his remote outpost in Coral Bay, Western Australia.
His true story is recounted in a case study published in this week’s edition of the New England Journal of Medicine.
“In the absence of other trained medical personnel or resources, the actions of this patient are likely to have had a substantial beneficial effect on the clinical outcome,” write three treating physicians at Sir Charles Gairdner Hospital in Nedlands, Western Australia.
“However,” they say, “a person’s self-management of a myocardial infarction cannot be considered medically appropriate if any other option is available.”
MORE IN SCIENCE
Brain tissue samples from people of all ages suggest we stop growing new neurons in our early teens
For all their risks, opioids had no pain-relieving advantage in a yearlong clinical trial
Deep gas bands, shapely cyclones — NASA’s Juno reveals more of Jupiter’s secrets