Are skin-cancer checks by doctors worth the trouble?
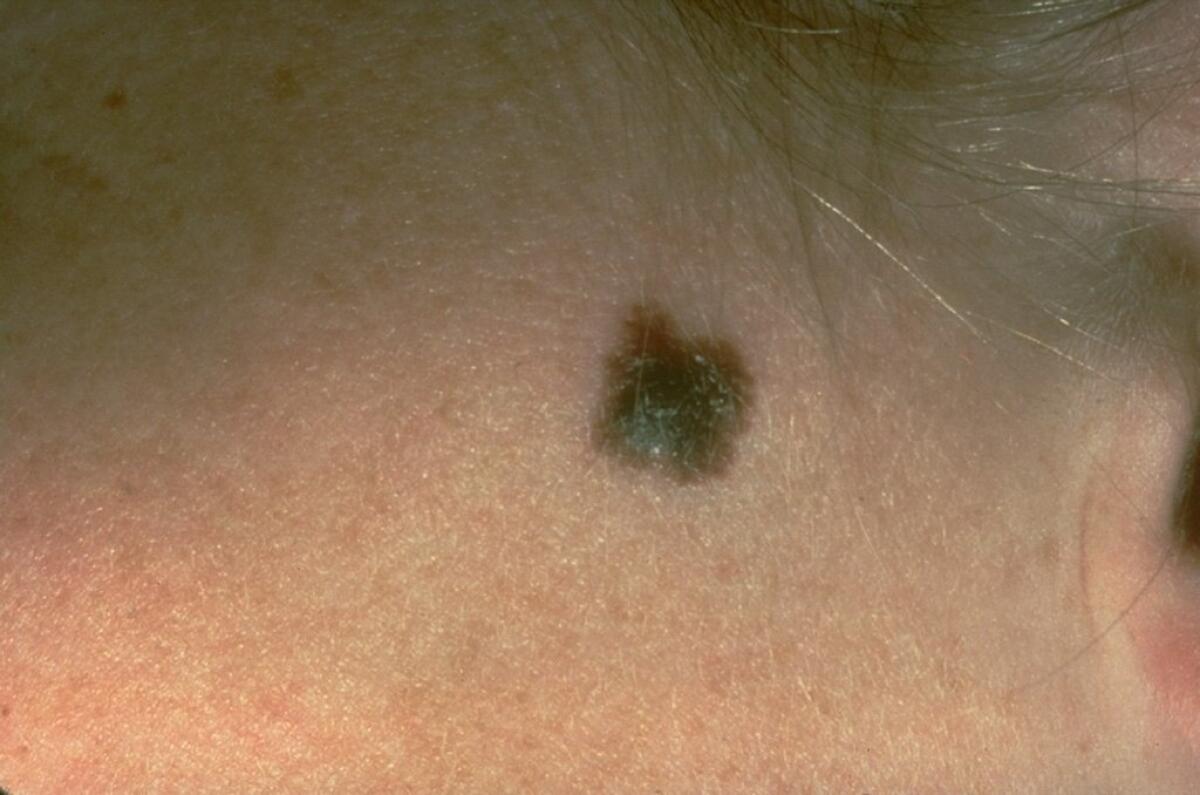
A federal task force that assesses the value of medical screening tests says it can’t judge whether skin-cancer checks by dermatologists are worth the trouble for healthy Americans because good research on the practice is lacking.
The finding of the U.S. Preventive Services Task Force is not a repudiation of the practice recommended by the American Academy of Dermatology, in which a medical professional inspects a patient’s skin for moles, thickening, discoloration or tags that might be cancerous.
But the task force does say there are not enough well-conducted studies to establish the practice saves lives without incurring undue risks for patients. And it could influence health insurers not to cover skin-cancer screenings for people who have no history of the disease.
Each year, 5.4 million new cases of basal and squamous cell carcinomas are diagnosed, and while they are seldom fatal, they can cause disfiguration and metastasize to other parts of the body if left untreated. The most deadly form of skin cancer, malignant melanoma, is diagnosed in more than 76,000 new patients yearly, and claims the lives of 10,000 Americans a year. Its incidence is growing faster than that of any other preventable cancer.
So the task force’s “ehh” finding prompted a chorus of concern.
In a statement released Tuesday, the American Academy of Dermatologists said it was disappointed by the finding.
“Dermatologists know that skin cancer screenings can save lives,” the academy said. Since the Academy launched a skin cancer screening initiative called “SPOTme” 30 years ago, the Academy said, dermatologists have performed more than 2.5 million screenings during which they have found more than 255,000 suspected nonmalignant skin cancers and 28,500 melanomas.
“We know that screenings, which are noninvasive, quick and painless, are the best tool possible to detect skin cancer early when it is most treatable,” the academy said.
At the same time, the dermatologists’ professional society wrote, “we acknowledge the need for additional research on the benefits and harms of skin cancer screening in the primary care setting.”
Writing in JAMA Oncology on the Preventive Services Task Force ’s recommendation, a trio of dermatologists pressed the case for continued screening.
Most patients — even those who have already been treated for melanoma, according to research — don’t check their skin thoroughly for problematic growths, wrote a team of dermatologists led by University of Mississippi dermatologist Vinayak K. Nahar. They overlook places where skin cancers can hide, or don’t use a mirror to get a closer look, or don’t enlist a loved one to help.
And let’s face it: Patients don’t really know what to look for, suggested dermatologists Hensin Tsao and Martin A. Weinstock, who wrote a JAMA editorial on the task force’s finding.
The American Cancer Society recommends that primary care physicians should check for skin cancer in all patients 20 or older during regular checkups.These doctors are armed with the helpful mnemonic “ABCDE” (with which they’re taught to look at moles for Asymmetry, Border irregularity, nonuniform Color, Diameter greater than 6 mm, and Evolution over time).
But even these physicians, wrote Tsao and Weinstock, may overlook melanomas that look benign or masquerade as something else.
In deciding that it had insufficient evidence on which to base a recommendation, the federal task force said it had found only one study of skin cancer screening, conducted in northern Germany. The study found modest evidence that lives were saved. But the study’s design was not the gold standard for weighing the risks and benefits of a biomedical intervention. And follow-up suggested the benefits were more modest still.
Nahar and her colleagues said the short duration of that research — people were screened for skin cancer only for a year in the study — probably resulted in an undercount of the lives it had saved.
And, they argued, the task force’s “insufficient” finding may send a message of complacency about skin cancer at just the wrong time.
“With melanoma’s decades-long increase in incidence and slow-to stabilize mortality, decisions must be made now,” the group wrote. “A recommendation stronger than [insufficient] is needed to emphasize screening as part of regular physical examinations,” the dermatologists wrote.
This is not the first time the federal task force of independent experts has waded into controversy with its findings. In 2009, the group drew the ire of breast cancer activists and many physicians by suggesting that yearly mammograms aren’t necessary for most women and that with some exceptions, women under 50 don’t need mammograms at all. In 2012, it recommended that men not get screened for prostate cancer using a prostate-specific antigen test.
MORE SCIENCE NEWS
Cloned animals don’t age any faster than conventional ones, study says
4 in 10 top-selling sunscreens on Amazon don’t meet dermatologists’ standards, study says
Why the Rio Olympics are not likely to increase the spread of Zika across the world