Despite rising demand, transplant surgeons get pickier with donor hearts
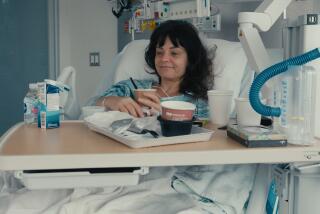
As the number of patients in need of heart transplants has grown, surgeons have gotten pickier about the organs they’re willing to use, a new study finds.
In 1995, 44% of available hearts ultimately found their way into new bodies, data from the Organ Procurement and Transplantation Network show. By 2006, that figure had dropped to 29%. As of 2010, it had rebounded somewhat to 32%, according to the study published this week in the American Journal of Transplantation.
In those years, the number of patients with end-stage heart disease who were waiting for new hearts grew steadily, the study authors noted. Experts estimate that the demand for donor hearts tops 20,000 per year, yet only 1,949 heart transplants were performed in the U.S. in 2011.
Without nationwide standards for judging the suitability of donor hearts, transplant surgeons have wide latitude in accepting or rejecting them on behalf of their patients. And indeed, the study authors found that some doctors were more accepting than others.
Surgeons in the United Network for Organ Sharing’s Region 1 – which includes Maine, New Hampshire, eastern Vermont, Massachusetts, Rhode Island and Connecticut – were consistently above the nationwide average in accepting donor hearts. On the flip side, surgeons in Region 9 – which includes western Vermont and New York state – were consistently below average in their donor heart acceptance rate.
This regional variability is probably a sign that in some parts of the country, suitable organs went unused, they wrote. It also highlights “the need for updated consensus guidelines on donor heart acceptance,” they added.
There may be some good explanations for why doctors on the whole have rejected so many donor hearts, especially in more recent years. The average age of potential donors rose from 40.3 years in 1995 to 43.2 years in 2010, the researchers found.
In addition, the proportion of would-be donors with chronic diseases went up during the 15-year study period. For instance, only 3.5% of them had diabetes in 1995; by 2010, that figure was 13.7%. Similarly, the prevalence of high blood pressure rose from 23.3% to 38.9%.
Hearts from women were less likely to be accepted by transplant doctors than hearts from men, the study authors found. Although the proportion of female would-be donors remained about the same, doctors declined these hearts at increasing rates during the study period.
Changes in the donor pool weren’t the only possible factor, the researchers noted. The doctors who take care of patients on the transplant list have benefited from the invention of good alternatives, which may have made surgeons feel less urgency to accept hearts they deemed of marginal quality.
Chief among them is the invention of the left ventricular assist device (LVAD) and other machines that can take over much of the function of a failing heart. “The option of stabilizing a patient with mechanical support as a bridge to transplant may make donor hearts with one or more undesirable features less likely to be accepted for transplantation,” the researchers wrote. But this probably isn’t the whole story, they said, because the decline in transplant rates began before these devices entered wide use.
Another possibility is that increased scrutiny of transplant centers from the Centers for Medicare and Medicaid Services has scared doctors away from using potentially problematic hearts, according to the study authors. If so, this would be an “unintended consequence” of “federal oversight,” they wrote.
If surgeons really are holding out for healthier donor hearts, it would be reasonable to expect that the outcomes for transplant patients improved over the study period. The researchers found a 3% increase in both 30-day and one-year survival, but they couldn’t say whether better organs deserved the credit. Improvements in medical and surgical care between 1995 and 2010 probably played some role as well, they wrote.
For more medical news, follow me on Twitter @LATkarenkaplan and “like” Los Angeles Times Science & Health on Facebook.