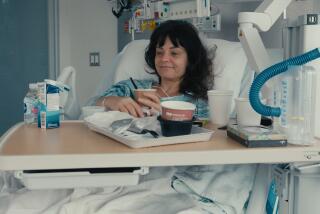
When brain-dead organ donors were cooled, their kidneys worked better in transplant recipients
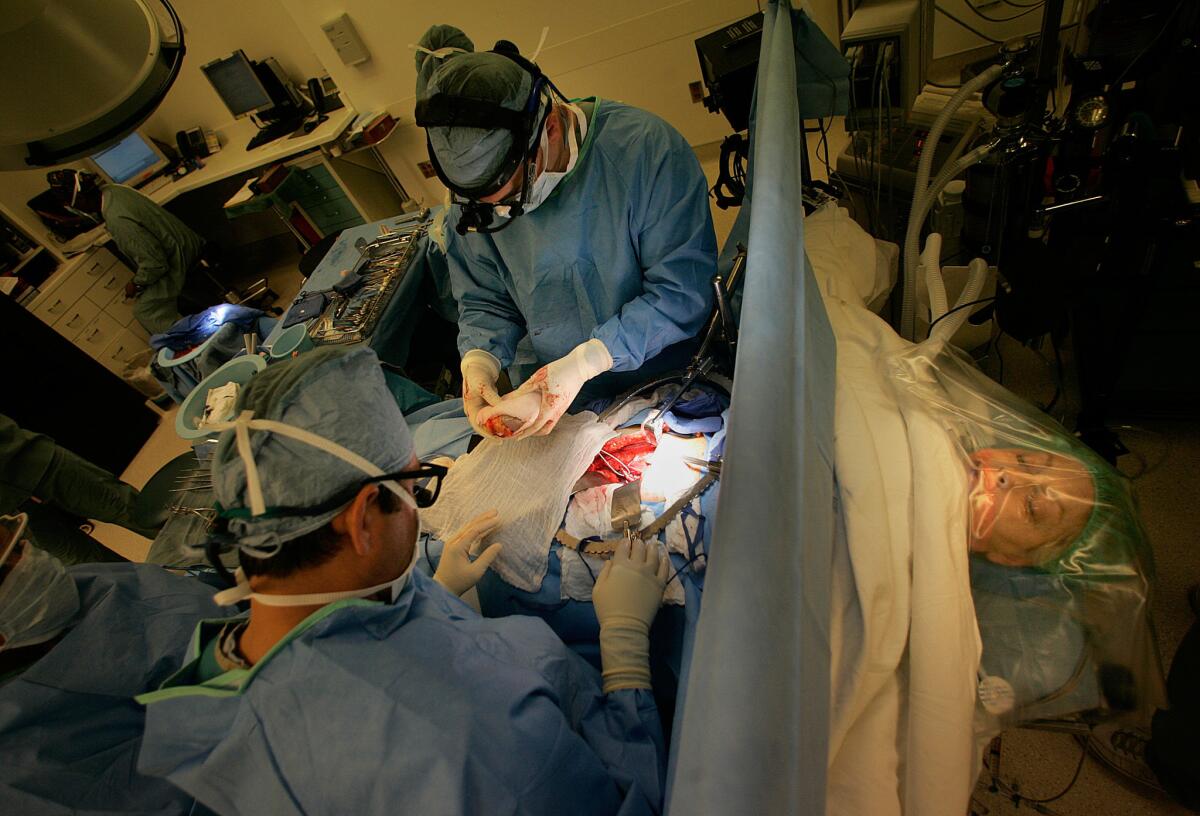
Researchers at UC San Francisco discovered that slightly cooling the bodies of deceased organ donors -- rather than heating them to normal body temperature -- improved the function of kidneys after the organs were transplanted into recipients. Here, UCLA surgeons transplant a kidney from a living donor into a patient.
Allowing brain-dead organ donors’ body temperatures to fall slightly after brain death — rather than following the accepted protocol of keeping donors warmed to a normal body temperature — resulted in more successful kidney transplants in a recent clinical trial, with fewer organ recipients requiring dialysis in their first week after surgery.
Once better understood and if eventually adopted, the simple intervention could improve outcomes for the 40% or so of kidney transplant patients who experience delayed organ function immediately after transplant and continued problems in the longer term. Improvements in transplant performance were particularly pronounced in kidneys harvested from high-risk organ donors, suggesting that the technique could potentially expand the universe of viable kidney donors.
The experiment was detailed in a study published Wednesday in the New England Journal of Medicine.
“This is a free intervention that can be done at any hospital in the world, and tens of thousands of patients worldwide can benefit from it,” study lead author Dr. Claus Niemann, a professor of anesthesia and surgery at UC San Francisco, said in a statement. “It could have a major impact on global health, especially in resource-limited countries, and provide significant cost savings in the United States through less dialysis, shorter hospital stays and potentially less need for expensive interventions.”
Between March 2012 and October 2013, Niemann and colleagues wrote, 394 deceased organ donors were assigned randomly to two groups: one that would be cooled to a state of mild hypothermia (93.2 to 95 degrees Fahrenheit), the other warmed to the clinical standard (97.7 to 99.5 degrees). Donors in the hypothermia group were cooled within 4 hours, and remained so until their organs were removed for transplantation.
In all, 583 kidneys were transplanted from trial participants: 285 from donors in the hypothermia group and 287 from donors in the normal temperature group. In all, 112 recipients who got kidneys from the normal temperature group, or 39%, suffered delayed kidney function. But only 79 recipients who got kidneys from cooled donors, or 28%, did. The relative odds of delayed organ function for patients who got kidneys from the hypothermia group were 38% lower than those for the patients who got kidneys from the warmed donors.
The results were so encouraging, the authors wrote, that the trial was ended early “owing to overwhelming efficacy.”
Cooling seemed to work particularly well in high-risk donors, which added to the approach’s potential.
“It may allow us to consider organs we may otherwise reject, especially at the extremes of age, which would result in more patients benefiting from kidney transplantation,” Niemann said in his statement. He added that there was a mismatch of transplant need and organ supply in the U.S., where 101,000 people are awaiting kidney transplants.
The study did not explore why the kidneys harvested from donors with lowered body temperatures functioned more successfully.
In an editorial published with the report, Drs. Ina Jochmans of University Hospitals Leuven in Belgium and Christopher Watson of the University of Cambridge in England described a complex chemical cascade that takes place in the body when brain death occurs. Much as cooling can limit neurologic damage after a brain injury by interrupting chemical processes in the body, so it might combat inflammatory and clotting processes that take place after brain death that can impact kidney transplant function, they wrote.
Jochmans and Watson, who were not involved in the transplant trial, noted that researchers still needed to learn more about the mechanisms underlying the positive effect, and that they would need to pinpoint procedures for future applications.
But they lauded the findings — and the low-tech nature of the approach.
“The results reported here will be welcomed for many reasons, not least of all because they have shown that, in this era of high-technology medicine and targeted drug therapy, it is still possible to identify a simple, cheap intervention that can have dramatic therapeutic effects.”
For more on science and medicine, follow me on Twitter: @LATerynbrown.
MORE SCIENCE NEWS
Brown dwarf aurora found; could inform exoplanet searches
T. rex and its ilk owed hunting success to special serrated teeth
Devastating floods might be more common than we thought, study says