For years, African women scarred by female genital mutilation had no hope. A California doctor is changing that
- Share via
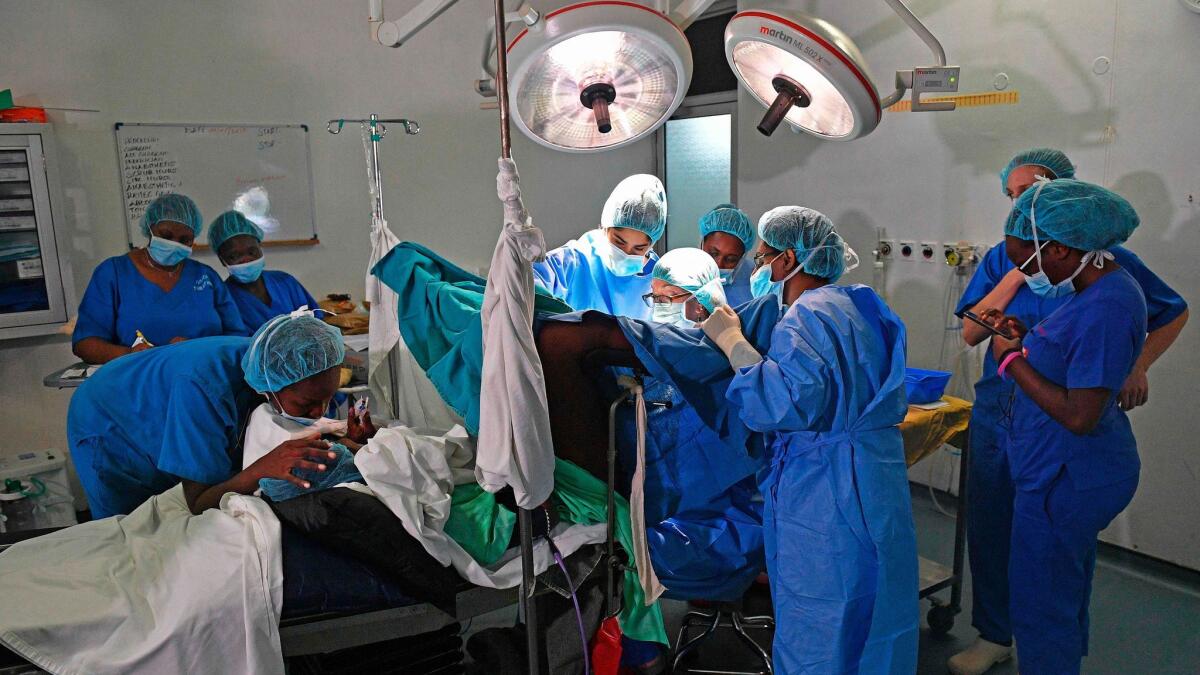
Reporting from Nairobi, Kenya — When she flew into Nairobi airport, Marci Bowers’ huge suitcase was crammed with sutures and medical instruments, everything she could fit inside.
The doctor from San Francisco was bound for a hospital in one of the Kenyan capital’s slums and needed the equipment for the work ahead: repairing women’s bodies, undoing the work of genital cutters who drag young girls from their homes to fulfill an ancient coming-of-age ritual.
It was the first time the operation to address female genital mutilation has been performed in Kenya, where some 5 million women from many ethnic groups are victims.
When women heard about the operation, they boarded buses and queued up from early morning outside the hospital for hours. Some traveled hundreds of miles to get there. Another flew from Ireland. The oldest patient was 64.
“The hospital was inundated with requests. It was beyond my wildest expectations,” said Bowers.
The operation Bowers performs was pioneered by a French surgeon, Pierre Foldes, and though it cannot replace lost tissue, it can improve sexual function by removing scar tissue covering the clitoris and cutting ligaments to allow the clitoris to descend.
Bowers’ Kenyan patients were drawn from an extensive waiting list, but some women who turned up at the clinic were added if the procedure seemed suitable to repair their injuries. The women had to pay about $96 U.S., and the $200 balance was covered by Clitoraid, a Las Vegas-based nongovernment organization, and a local organization, Garana.
Although illegal in most parts of Africa, female genital mutilation, which involves removing part of the clitoris, has proved to be tenacious. In many communities there is no other path to adulthood. Kenyan Christian missionaries tried to eradicate the practice in the late 1920s, but met strong community opposition.
The women ... grabbed my legs and pinned me against the wall. Then an old woman performed the cut.
— Cynthia Simantoi, 23, forced to undergo female genital mutilation about age 12
Girls who flee female genital mutilation may be shunned as “dirty,” seen as unmarriageable and taunted as eternal children. One major reason parents force their daughters to undergo the procedure is to avoid social stigma.
Cynthia Simantoi’s parents both opposed ritual cutting, yet she was still forced to undergo it against their wishes. Bowers operated on the 23-year-old university student from the Masai community.
One December evening in 2007, Simantoi was at home alone washing the dishes when seven women, including her aunts and other relatives, came for her. Her father, a government administrator, and mother, a schoolteacher, were away from home.
“There was nothing I could do,” Simantoi recalled. “It was so abrupt. There were no signs at all, so I couldn’t have escaped.” About 12 at the time, she struggled in vain.
“The women who were not so old grabbed my legs and pinned me against the wall. Then an old woman performed the cut. It was painful. I passed out, and when I woke up I was overwhelmed.
“I felt so bad, so hopeless. I cried the whole evening. They tried consoling me and telling me I am now a big woman.”
But she felt violated and betrayed, and as years passed, the bitterness never left her.
“I felt like I had lost my self-esteem,” she said. “I didn’t want to do it. In fact it affected me psychologically.” Around the same time she was cut, Simantoi added, one of her cousins died because of complications in childbirth caused by the scarring left by female genital mutilation.
Bowers said that the practice can leave women traumatized for years, even decades. When they were cut, her patients were often warned not to show pain or speak about the cutting.
“A lot of communities tell them if they cry, they’ll bring shame on the family,” she said.
The secrecy around female genital mutilation makes it difficult to eradicate, with men often unaware that is extremely painful and may lead to complications, such as infection or childbirth difficulties.
Even Dr. Abdullahi Adan, a Nairobi plastic surgeon who initiated the Clitoraid project after patients sought help, was unprepared for what he learned. As he and Bowers held counseling sessions with patients, he realized how his mother and aunts, all of whom underwent cutting, had suffered in silence.
“I learned a lot,” he said. “I was ignorant about a lot of these things. It has made me a better man. What struck me was that all of them felt less of a woman than other women who have not had the cut. Literally, all of them said, ‘I want to feel like a full woman.’ It had scarred their minds.”
Bowers was part of an unsuccessful Clitoraid effort in 2014 to establish a hospital in Burkina Faso, West Africa, to perform female genital mutilation reversals. The hospital was built, but the government withdrew permission for it to open and canceled the visas of Bowers and other members of the medical team.
A doctor trained by Bowers has recently begun to carry out the procedure in Burkina Faso, but not at the Clitoraid hospital.
According to UNICEF, about 125 million girls and women, mainly in Africa and the Middle East, have undergone female genital mutilation, usually around age 5.
It is most prevalent in Egypt, Sudan, Mali, Guinea and Sierra Leone, where 80% of girls and women ages 15 to 49 have been cut, according to a 2013 UNICEF report. About 27% of Kenyan women in that age group have undergone the procedure, even though the Kenyan government banned the practice in 2011.
Some immigrant communities in the U.S. and Europe also carry out the practice, often on small girls. A Detroit doctor, Jumana Nagarwala, was charged in April with performing genital mutilation on girls as young as 7 at a clinic in Livonia, Mich.
When Simantoi had the operation to reverse it, she did not tell her family “because they may think I am against our culture. I feel better now and after going through the counseling I know my body well. I hope there will be more awareness about the operation.”
In all, Bowers spent two weeks in Nairobi and operated on 44 women. She trained six local doctors, including Adan, in the procedure, while 12 more doctors observed.
Hundreds of women who had come seeking help had to be turned away, and put on a waiting list. It is not clear when, or if, they will be helped.
Twitter: @RobynDixon_LAT
To read the article in Spanish, click here
ALSO
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.










