Californians with disabilities are outraged over vaccine de-prioritization

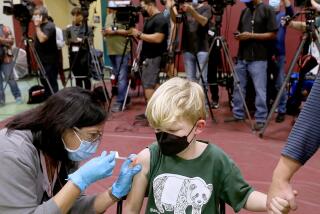
Like many Californians, 47-year-old Ntombi Peters has watched the state’s plodding vaccine rollout with equal parts anticipation and dread. For months, the Long Beach resident believed her turn would be next. Then, last week, Gov. Gavin Newsom announced that disabled and chronically ill Californians were losing their place in the line.
“They act as if we do not exist. Or if we do, we’re expendable,” said Peters, who uses multiple inhalers and daily medications to control her severe asthma and is on immunosuppressant drugs to treat multiple sclerosis, both of which put her at severe risk from COVID-19. “It’s very disheartening.”
Like most states, California had previously planned to deliver vaccines in tiers, with essential workers and people with certain high-risk medical conditions prioritized over healthy, low-risk adults. But that work has been slower here than elsewhere. In response, Newsom abruptly reversed course on Jan. 25, scrapping the tiers in favor of a purely age-based rollout.
Experts say that move could be a shot in the arm for the state’s sluggish inoculation program. But for disabled and chronically ill Californians, the decision sparked confusion, distress and anger.
“Clearly, we are living in a culture that still sees people like me as disposable,” said Alice Wong, 46, a disabled activist in San Francisco, who created the hashtag #HighRiskCA in response to the change. “This is clearly erasure, this is eugenics, and I consider this a form of violence. It is a form of violence against the most marginalized communities.”
Wong has respiratory failure and uses a ventilator to help her breathe. But, she said, many others are also at high risk of complications and even death from COVID, whether or not that risk is obvious.
“That’s a huge misconception that’s very dangerous,” the activist said. “You don’t have to be somebody like me, a ventilator user, to be high risk.”
For example, those with intellectual and developmental disabilities appear to be three times more likely to die from COVID than those without. Caregivers, including thousands of parents of children with autism and Down syndrome, are currently eligible to receive the vaccine in California, while adults who live with those conditions are not.
“It just doesn’t make any sense,” said Reid Davenport, 30, a filmmaker in Oakland who has cerebral palsy. “The California state government has completely overlooked people who are at higher risk for hospitalization and death, and I don’t understand why.”
Neither are those at greatest risk from the virus necessarily able to shelter at home, as Peters, Wong and Davenport do.
“I can count the days I’ve worked from home,” said Lillibeth Navarro, a polio survivor and executive director of Communities Actively Living Independent & Free in Downtown L.A., who spoke at a news conference on Thursday.
Many disabled and chronically ill Californians work in front-line occupations or live with those who do. In fact, many of the same conditions that have made COVID so much more deadly in Black, Latino and Native American communities are tightly linked to the conditions that make illness and disabilities more prevalent there.
Among the most significant is poverty.
“There’s a high correlation between poverty and disability,” said Andy Imparato of Disability Rights California, who also serves on the state’s vaccine advisory committee. “If you grow up poor in a poor neighborhood you generally have less access to healthcare, which can create disabilities. And if you have a disability growing up middle class, you’re more likely to be in poverty as an adult.”
But the calculus of vaccine equity is more complex, experts say. California has so far had one of the slowest rollouts in the country. While the Golden State has put more shots in arms than any other by raw numbers, it has used a smaller percentage of its available doses and has vaccinated a smaller percentage of the total population than other populous states.
Everyone agrees that’s an equity problem, since the burden of unchecked transmission falls disproportionately on those least able to shelter from the virus and those most vulnerable to its worst outcomes. The disagreement is over whether speed or precision matters more.
“We talk about this as a trade-off of efficiency and equity, but I think there’s just issues of general effectiveness,” said Dr. Kirsten Bibbins-Domingo, an epidemiologist and co-founder of the UCSF Center for Vulnerable Populations. “Age is not only efficient, it’s easy for the vaccination sites to confirm.”
A 26-year-old farmworker and a 17-year-old grocery clerk with Down syndrome may be at far greater risk of infection and death than a 62-year-old corporate lawyer, but all of them likely use the same California driver’s license to prove their age. Occupation can be much trickier, and documenting disability status almost always requires a doctor — ideally a primary care physician — which only the lawyer is likely to have.
“There is immense variety in the type of disability that can place you at higher risk from COVID,” said Dr. Alyssa Burgart, a bioethicist at Stanford. “We collect age very frequently in all sorts of spaces, but we are not necessarily collecting disability status in a routine and high-fidelity way that we can use [to allocate vaccines].”
Still, she and others believe it should be done.
“We need to hold people accountable,” said Wong, the activist. “The government is essentially erasing us.”
More to Read
Start your day right
Sign up for Essential California for news, features and recommendations from the L.A. Times and beyond in your inbox six days a week.
You may occasionally receive promotional content from the Los Angeles Times.