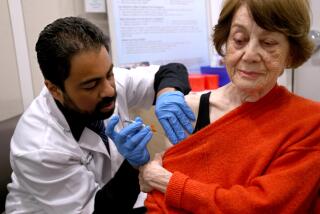
As infections rise, the San Joaquin Valley becomes the land of the eternal COVID surge

This is what the COVID-19 pandemic looks like in the part of California where the Delta variant surge refuses to let up.
In Fresno County, understaffed hospitals have been so clogged that ambulance crews have stopped transporting people unless they have a life-threatening emergency.
In Tulare County, a Visalia hospital — which has been treating more COVID-19 patients in recent days than any other medical facility in the state — declared an internal disaster last week on a day 51 patients in the emergency room waited for a bed to open up.
And this week, sparsely populated Kings County, which has one of California’s lowest vaccination rates, had one of the state’s highest per capita COVID-19 hospitalization rates.

Over the last year and a half, the rural, agricultural San Joaquin Valley has been a perpetual hot spot for the virus — the land of the eternal COVID-19 surge.
Case numbers and hospitalizations plummeted across California, including in Los Angeles and the San Francisco Bay Area, after the height of the summer surge. But not in the San Joaquin Valley.
“We kind of have been feeling like the forgotten area of California as we read that, statewide, things are improving,” Gary Herbst, chief executive of Kaweah Health Medical Center in Visalia, told The Times. “It’s like we’re almost in a different country, even though we are right here in the middle of the state.”
The San Joaquin Valley this week has the state’s highest rate of COVID-19 hospitalizations. For every 100,000 residents, the region had 24 people hospitalized with COVID-19. Southern California, by comparison, had eight per 100,000 residents hospitalized with the virus. The San Francisco Bay Area had four.
In Fresno County, the region’s most populous, the vast majority of patients now hospitalized with COVID-19 are unvaccinated. They are mostly people in their 30s, 40s and 50s, and are often the primary financial providers for their families.
There are many reasons the region is continuously besieged, but the primary culprit, public health officials and hospital administrators say, is a low rate of vaccination.
Kings County has the third-lowest inoculation rate in the state, with just 39% of its 150,000 residents fully vaccinated, compared to 63% of all Californians.
On Tuesday, the county had the state’s highest per capita COVID-19 hospitalization rate, with 34 patients per 100,000 people. By comparison, Los Angeles County, which has 64% of its 10 million residents fully vaccinated, had 6.5 patients per 100,000 people.
There’s also politics. The San Joaquin Valley is largely conservative, and, nationwide, rural residents and Republicans are among the least likely people to be vaccinated against COVID-19, surveys show.
Fresno City Councilman Garry Bredefeld — who has tweeted “Let’s go Brandon,” code for “F— Joe Biden”, multiple times in recent days — said he and his constituents believe the government has overstepped its bounds with business lockdowns, school and church closures, and mask and vaccine mandates.
Bredefeld said he is vaccinated and that he encourages people to get vaccinated if they want to. But he called it “experimental” and said no one should be forced by the government or their employers to get it.
“This is still America, land of the free, and that means freedom to make your own decisions for yourself, your children and your family,” he said.
The valley’s essential workers in agriculture and food processing — who are primarily Latino, often live in crowded housing, and never were able to work remotely — have been hard-hit by the virus.
The San Joaquin Valley is plagued by a chronic shortage of doctors, and there are fewer hospitals and pharmacies across vast rural areas.
And the region has a high level of poverty. With that, medical officials say, comes high levels of chronic health conditions that make residents more vulnerable to COVID-19 hospitalization and death: diabetes, congestive heart failure, asthma and obesity.
“We’re dealing with decades of health disparities, and we’re trying to fix it all during an emergency response, and the results aren’t there, to be quite frank,” Fresno County interim health officer Rais Vohra told reporters last week.
Last month, health officials were optimistic that trends were headed in the right direction after the Delta surge peaked in August.
In Fresno County, some public health staffers planned vacations for November, hoping for a brief respite before an anticipated winter surge.
As the strain on emergency rooms seemed to be lessening early last month, public health officials eased a policy that limited ambulance rides to seriously ill or injured patients.
But COVID-19 hospitalizations ticked right back up.
Just three weeks after the ambulance policy was relaxed, it was reenacted last week because emergency rooms were so crowded that it frequently took two to four hours to offload patients, according to the Fresno County Department of Public Health.
Paramedics who respond to 911 calls now assess patients and, if they are not critical enough to be transported, refer them to their primary care doctors, urgent care or telehealth.
Despite extensive outreach, the inoculation rate remains stubbornly low in Fresno County, in part because of widespread misinformation about the vaccine, Vohra said.
“We are just not having productive conversations about how to keep people safe, how to plan your holidays, how to talk about boosters and risk levels,” he said.
A troubling sign for the weeks to come, he added, is that demand for booster shots has been low.
“We’ve kind of hardened ourselves to the reality that we’re going to be in for a hard winter. There’s a level of exhaustion that I haven’t really seen in my whole career among medical staff and my colleagues.”
Gurvinder Kaur, the medical officer for Adventist Health in the Central Valley — which includes four small community hospitals in Kings, Tulare and Fresno counties — said that staffing issues that already existed before the pandemic have just been made worse by the barrage of COVID-19 patients.
Recruitment has long been a challenge in rural areas in the San Joaquin Valley and beyond, she said. And now, during the pandemic, it is a challenge to even attract travel nurses to the Central Valley because they prefer to work in places like Los Angeles or San Francisco.
“We can have a bed, but if you don’t have the nurse to take care of the patient, that bed is of no use,” Kaur said.
On Thursday, Kaur said, there were 51 COVID-positive patients at Adventist Health Hanford, a 173-bed acute-care medical center that is the largest of Adventist’s hospitals in the region.
By comparison, the 600-bed Los Angeles County+USC Medical Center has averaged 21 COVID-19 patients over the last week.
In Tulare County, where just 47% of residents are fully vaccinated, the 435-bed Kaweah Health Medical Center in Visalia has averaged 111 COVID-19 patients over the last week — more than any other hospital in the state.
The hospital declared an internal disaster, called a Code Triage, for two days last week, before the state sent extra nurses to help the overburdened staff.
During the Delta surge, some patients have waited in the emergency department for days for beds to open up, Herbst said. Some received treatment for a day or two in the waiting room.
Even before the pandemic, the region had a lot of people hospitalized because of chronic health conditions, Herbst added. Having around 100 COVID-19 patients for weeks on end has pushed the staff to the brink, he said.
Exhausted healthcare workers have quit in droves in recent months, and the hospital is relying heavily on travel nurses.
The Kaweah Health system employs 5,100 people — and currently has 700 job openings, Herbst said. It has only 80 applicants.
“There’s a ‘Help Wanted’ sign in front of virtually every department in our organization,” Herbst said.
About 80% of Kaweah’s employees are vaccinated, Herbst said. The beleaguered medical staff has struggled with burnout and compassion fatigue, he added. Almost all of the COVID-19 patients in the hospital are unvaccinated, he said.
San Joaquin Valley, he said, “is largely conservative in political beliefs, religious beliefs,” and many residents do not trust the government or the vaccine.
Bredefeld, the Fresno city councilman, said the government’s messaging has focused too heavily on vaccination, with not enough emphasis on treatments like monoclonal antibodies.
“You are not going to vaccinate your way out of this,” Bredefeld said.
But Hernan Hernandez, executive director of the Delano-based California Farmworker Foundation, argued that more employee mandates are needed in the San Joaquin Valley, especially among agricultural workers and Latinos, who have been disproportionately affected.
“Farmworkers are no different than teachers, than nurses,” he said. “They’re human. They’re not going to change jobs if they’ve been working a job 15 or 20 years and they’re comfortable there. They’re going to get the vaccine.”
The virus’ impact among rural Latinos in the region has been devastating, Hernandez said. These days, about every farmworker he talks to has a story about someone in their family dying or getting sick.
He was frustrated about what he sees as the unequivocal reason the region keeps seeing coronavirus surges, even as other areas improve.
“At this point, it’s the vaccination rate,” he said. “There are no other explanations.”
Times staff writers Rong-Gong Lin II, Luke Money and Sean Greene contributed to this report.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.