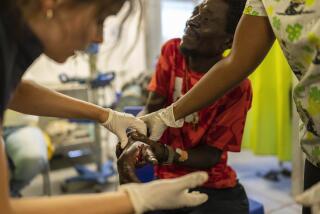
Aid group has set the gold standard on Ebola safety
The decontamination ritual, performed dozens of times a day here at the Ebola treatment unit run by Doctors Without Borders, resembles a slow dance.
Two European medical workers emerge from the high-infection zone and raise their arms, turning slowly in the rain of heavily chlorinated water directed by men with sprayers.
“Take off your mask. Wash your hands.” A colleague supervises each of the workers, calling out more than 20 steps as the exhausted women slowly remove their lethally contaminated protective suits, masks, goggles, boots and two sets of gloves.
They wash their hands eight times during the process, starting with their gloves on. Their lives could depend on doing it all without a single mistake.
Dizzy in the thick tropical heat, one of the women sways, but recovers. She and her companion are dripping with perspiration, their hair sopping, as they wriggle out of the yellow PPE — personal protective equipment — suits.
“You want people, no matter how tired they are, no matter how fuzzy-headed, to be doing things correctly,” said Armand Sprecher, head of public health for Doctors Without Borders, the international medical aid group also known by its French initials, MSF.
How did an aid group working out of white tents in West Africa become the gold standard in Ebola treatment, when hospitals in Dallas and Madrid have struggled to protect the workers they’ve deployed to treat Ebola patients?
Western hospitals, with access to advanced technology like zero-pressure rooms, confront conditions far less trying than the business of treating thousands of desperately sick Africans in tent isolation wards. Here, the line delineating severe contamination danger is not a heavy door, but orange plastic fencing on gravel-covered ground.
Staff members at the Dallas hospital where Liberian Thomas Eric Duncan died recently of Ebola have complained that the protection gear was flimsy and workers lacked proper training, allegations that mirrored those from a hospital in Madrid also treating an Ebola patient.
At the heart of the intense training of staffers working with the MSF in West Africa are the slow, careful procedures of donning the protective gear and, especially, removing it. When putting on the suit, gloves, boots, hood mask, goggles and apron, each nurse, doctor or sprayer has someone spotting them, making sure they don’t leave a tiny gap in their gear. Taking it off, they are again observed and guided by a fellow staff member.
The MSF has two decades of experience treating Ebola, more than any other organization. The group cut its teeth working on outbreaks of the virus in places such as the Democratic Republic of Congo, when the virus was limited to rural villages. It has also handled outbreaks in Uganda, Sudan, Gabon, Guinea and the Republic of Congo.
It was easier to isolate cases in villages and to inform communities of the risks of contact. The MSF was better prepared than most to deal with the current outbreak in Guinea, Sierra Leone and Liberia. But as the virus leaped across borders into crowded urban settings, the organization warned that it was slipping out of control.
The MSF didn’t have an Ebola casualty until the current outbreak, which the organization says has stretched its experience and expertise to the limit.
The humanitarian group’s safety procedures have been adopted by other organizations working on Ebola in West Africa, including the California-based International Medical Corps, which runs a treatment facility in Bong County, Liberia.
But the MSF record isn’t flawless: Two foreign staff members have been infected, including a French nurse who was working at the front gate of the unit in Monrovia, one of the most contaminated areas of the site because of the large numbers of extremely ill patients who arrive there seeking admission, often vomiting or bleeding. The MSF reviewed its procedures afterward, and nurses at the gate began wearing thick plastic face shields when meeting patients.
A Norwegian staff member was recently infected in Sierra Leone, a case being investigated. Commenting on that incident, director of operations Brice de le Vingne said there was always a risk involved in dealing with Ebola, despite the strict protocols.
In addition, 19 local MSF staff members contracted Ebola, 12 of whom died. But the organization believes that “the vast majority” were infected in the community, not at the treatment center, a spokeswoman said. Medical workers often come under intense pressure from friends, family and community members to help sick people.
When other humanitarian groups hesitated to send workers to West Africa after the Ebola outbreak was identified in March, the MSF scaled up dramatically. It was among the few. The infection of three American staff members from the charity Samaritan’s Purse in West Africa apparently deterred other groups from involvement.
A smell like a public swimming pool drifts across the MSF compound in Monrovia. Ebola, contagious and potentially deadly when it touches human skin, is quite easily killed with chlorinated water. The virus can be picked up by contact with the bodily fluids of a symptomatic person, or from a surface an infected person touched, or from clothing or bedding.
People with backpacks filled with strongly chlorinated water walk around the MSF compound spraying the high-risk areas where patients are treated, the orange plastic barriers around those areas and the gravel in and near the isolation ward.
Everyone who enters or leaves the compound has their boots sprayed. Hand-washing tubs filled with chlorinated water stand on every corner.
Inside the isolation zone, staff in PPE suits burn every contaminated item, from the clothing of patients to the used suits and gloves.
Nothing sharp that could pierce a suit, like a knife for patients to cut food, is allowed inside the facility.
American nurse Monia Sayah, who has worked on Ebola response here and in Congo, said in a recent interview that she never felt afraid when caring for Ebola patients in West Africa.
“I feel like if we follow the procedure, I feel very safe. We have very strict infection-control measures. When we use personal protective equipment, we use a set of behaviors,” she said. “We have a rule: We don’t shake hands, we don’t hug.”
Sayah said her biggest fear was a needle stick injury. But she feels that it would be easier to pick up the virus outside the isolation ward, while visiting a market or interacting with people outside, for example, a view echoed by Sprecher.
“Out in the world, you don’t know where the virus is,” he said. “You get into a cab, you don’t know if somebody with Ebola had vomited on the seat.”
The MSF puts the safety of staff first, above even patient welfare. Until recently, it didn’t offer intravenous drips to patients in the Monrovia facility because of the risk to workers. A spokeswoman in Monrovia said that the facility has begun offering IVs, but only to patients unable to drink fluids.
Workers heading to West Africa are trained at a facility in Brussels, training that is duplicated for local staff in Africa. After receiving lessons on how to avoid infection when dealing with patients and how to don and remove protective gear, workers spend time in a simulated Ebola treatment unit learning how to handle the kinds of situations they’ll face in the horrors of a real facility.
The group has more than 3,000 staff members in West Africa, including 240 foreign workers, operating six treatment units with 549 isolation beds. It has treated more than 2,400 patients, out of the total 8,997 cases, with a survival rate of 37.5%, higher than the overall average of 30% that was cited Tuesday by the World Health Organization.
The MSF has shipped in more than 670 tons of equipment, much of it chlorine and protective gear. By the end of the year, it will have spent $60 million fighting Ebola.
Its health workers spend a maximum of a month working in isolation wards and then are rotated out. They work in shifts of only an hour at a time, because of the intense stress and heat involved.
At other facilities in the region, particularly under-resourced government facilities, the safety record has been poor: About 427 doctors and nurses have been infected, mainly in government facilities, and 236 of them have died, a catastrophic loss in West Africa, where doctors are scarce.
There were so many infections in government facilities that dozens of workers fled this year and treatment collapsed in many areas. The number of casualties has continued to climb steadily in recent weeks.
In Liberia this week, staff confidence in government Ebola facilities wobbled again when some doctors and nurses went on strike over inadequate hazard pay.
One government staff member, Eric K. Jacobs, told the Liberian news website Front Page Africa that he had seen a colleague infected with Ebola after a patient attacked him and tore his suit with his fingernails.
“Many of our colleagues are dying; they are getting infected with the virus,” Alphonso Williams, a hygienist at a government facility, told the site. “This work is not a normal hospital. This work we do here is something that is between life and death for us.”
Dixon, who is based in South Africa, reported recently from Liberia. Times staff writer Alan Zarembo in Los Angeles contributed to this report.
More to Read
Start your day right
Sign up for Essential California for news, features and recommendations from the L.A. Times and beyond in your inbox six days a week.
You may occasionally receive promotional content from the Los Angeles Times.