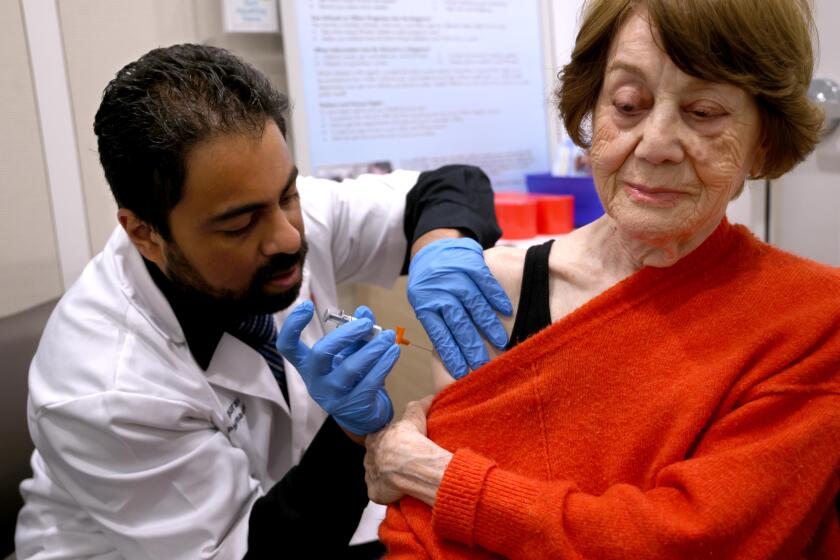
Medi-Cal recipients warned they could lose day healthcare benefit

State healthcare officials are warning certain Medi-Cal recipients that they are in danger of losing their ability to attend adult day healthcare centers, where they receive nursing care, social services and meals.
To continue receiving the benefit, officially called Community-Based Adult Services, eligible Medi-Cal beneficiaries must be in managed care, according to state officials. Nevertheless, thousands of eligible patients have opted out of managed care, said Jane Ogle, a deputy director at the California Department of Health Care Services.
Ogle said many Medi-Cal patients incorrectly believe that if they move to managed care, they will lose their Medicare doctors. “There is a bunch of misinformation,” she said.
FULL COVERAGE: Seeking healthcare
The state has started aggressively reaching out to doctors, patients and centers to better educate them about the transition to managed care. The healthcare services department is also extending the deadline for the transition from Oct. 1 to Nov. 1.
About 40,000 people originally attended the adult day healthcare centers. The state determined that roughly 28,000 were eligible to continue receiving the Medi-Cal benefit.
There is “mass confusion” among patients, said Lydia Missaelides, executive director of the California Assn. of Adult Day Services. “It has really been a challenge to get authoritative and accurate information out to these beneficiaries and help them make a decision based on facts rather than myths or fears,” she said.
If too many people opt out of managed care and can no longer attend the centers, some could close, Missaelides said.