Net gains for Africa
THE ROAD to Uganda’s northeastern Kaberamaido District is not for timid drivers. Maps show it as paved, but it has no shoulders, no painted stripe dividing its two narrow lanes and, in some places, no asphalt. Overloaded trucks and crammed matatus — the minibus-taxis that far outnumber private cars — careen around crater-sized potholes. Last-second swerves to avoid head-on collisions scatter the women and men on foot and bicycle who line the road’s crumbling edges. Even the boldest drivers strive to get off the road before darkness conceals all hazards, not least of all the roving bandits.
Charles Akora leaves the capital, Kampala, at sunrise and makes the 280-mile trek in six bone-jarring hours. Akora, 37, is the malaria program director for the local affiliate of PSI, an international aid group headquartered in Washington. He is overseeing a monthlong campaign to introduce to this remote district insecticide-treated bed nets that kill malaria-carrying mosquitoes.
Driving has its dangers, but malaria is the country’s leading cause of illness and a leading cause of death, especially of children under 5. The mosquitoes that carry the malaria parasite bite mostly at night, which makes sleeping under a treated net a strikingly simple way to prevent the disease. But getting the nets to the people who most need them is anything but simple. And the international aid community is roiled in debate over whether to sell or give away the nets. The feud obscures a tougher challenge: supplying a scattered population that lacks not just basic infrastructure but also basic knowledge about the fever that kills and sickens so many.
The challenge
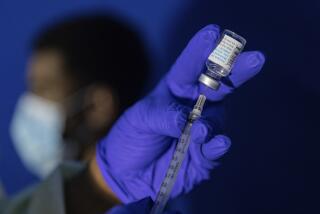
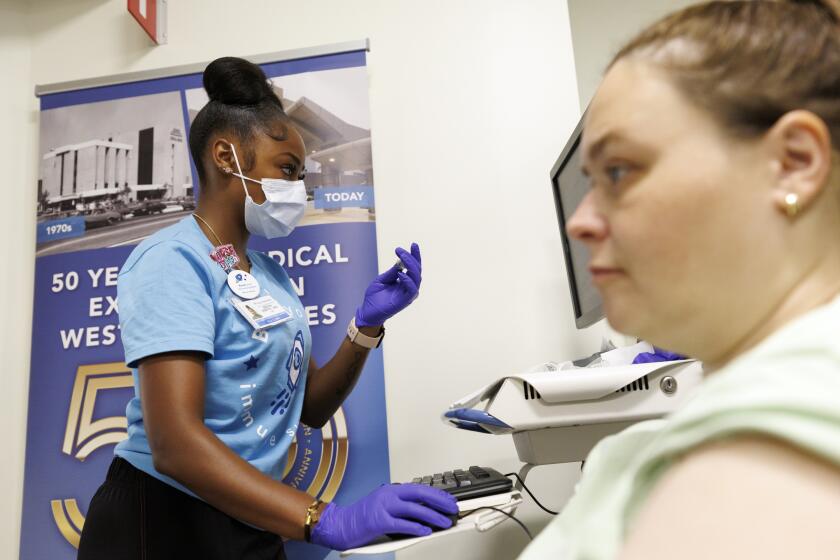
The United States all but eradicated malaria in the 1950s with drugs and the pesticide DDT. But in tropical Africa, where the parasite is widespread and mosquitoes can breed in a cow’s footprint, malaria remains entrenched. The death rate has increased over the last few decades as the parasite became resistant to once highly effective drugs. DDT, banned in the U.S. for harming the environment, is still used in limited circumstances as a house spray, but it is not the miracle worker some suggest it could be if only Western aid groups would get behind it.Today’s weapon of choice in the war on malaria is a net treated with a biodegradable pyrethroid insecticide. The net works not so much because it forms a foolproof barrier against mosquitoes — it doesn’t — but because the insecticide kills the bugs. The most astounding results come when treated nets multiply across a village. When net use reaches a tipping point of about 60% of households, they kill enough mosquitoes that the protective benefits extend even to the households without nets. The Roll Back Malaria Partnership, an alliance of aid agencies and African nations that aims to halve malaria deaths by 2010, set a goal of getting 60% of pregnant women and young children to sleep under insecticide-treated nets.
It sounds so simple. Except it’s not.
Free markets vs. free nets
PSI pioneered the concept of “social marketing” in the 1970s to promote family planning in Kenya. It used all the bells and whistles of an advertising campaign to create a demand for condoms and then supplied them for sale at subsidized prices through shops and health facilities. The aim, embraced by the United States and many international donors, is to create a market that can sustain itself after outside assistance goes away.This approach has its critics. Jeffrey Sachs, the Columbia University economist and author of “The End of Poverty,” is the best-known advocate of giving the nets away. He argues that charging even a token amount puts this lifesaving intervention out of reach for Africans who live in rural villages and urban slums on less than $1 a day. Sachs supports nationwide campaigns such as the one in Togo, which in one week in December gave away 1 million free nets with measles vaccinations.
PSI, for its part, points to Malawi, where it sold 1 million subsidized nets last year and which is now on track to meet net-use targets. It also argues that paying even a token sum has a value that goes beyond building a sustainable system. When people decide to buy a net, they commit to using it and signal that they understand why and how it’s used, which has not always been the case when nets were given away free, only to be used as wedding dresses and fishing nets.
The latter examples anger free-net advocates such as Kevin Marsh, director of the Kenya Medical Research Institute. “I’ve lived in Africa for 20 years,” said the British expat, “and I’ve never seen an African use a mosquito net as a fishing net.” But in an office next door, Kenyan entomologist Charles Mbogo says he has — and as pillows too.
Mbogo believes the argument over how to distribute nets misses a crucial point. Widespread use of nets means unlearning the lessons of generations that malaria is a mysterious and unavoidable fact of life. “I always hear about scaling up nets,” Mbogo said, “not about scaling up education.”
Another reality check on net distribution: Only two manufacturers are authorized by the World Health Organization to make insecticide-impregnated netting, and they do not produce enough to meet demand. So even as aid agencies debate whether it’s possible to create sustainable markets in the remotest villages of Africa, the international community has failed to ensure sufficient supply. In a coming editorial, we will suggest what donor countries must do to address this supply problem.
Roadblocks to use
Given the enormity of the need, there is little reason to categorically reject one of the two conflicting distribution models for anti-malaria nets. “The reality on the ground is that most people recognize the need for something in the middle, a segmented market where some nets are market-priced, some are subsidized and some are free,” said Chris White, malaria director for the Nairobi-based African Medical Research Foundation.The challenge is to find that balance — and figure out how to deliver both nets and education in a cost-efficient way. As PSI-Uganda’s campaign in Kaberamaido shows, it isn’t easy. In one typical village of round huts with grass roofs and walls of mud and dung, Charles Akora makes his pitch. Beneath the shade of two mango trees, about 100 children sit on the ground in a half-circle around Bella Akello, a local woman recruited and trained by Akora. The 21-year-old is explaining that what she and every other villager learned from their grandmothers is wrong: Omusujja, or fever, comes not from eating too many mangoes but from the mosquitoes that, like the harvest, follow the rainy season.
As adults drift over to see what’s going on, Akello pitches a rectangular net on four bamboo stakes over a woven grass sleeping mat. She shows how to treat another net with insecticide, something that must be done every six months (though a new line of nets can go three years without re-treatment). Or rather, she recruits a volunteer from the audience to do the honors, drawing gales of laughter by choosing a husband for a job no man would normally do. Following Akello’s instructions, the villager measures water into a dishpan, slips plastic bags over his hands (gloves aren’t much of a concept in this tropical land) and empties a packet of insecticide into the water. The children leap to their feet, and the two dozen men and women sitting at wooden desks in the back tilt forward to see.
This is entertainment, Kaberamaido-style, and both Akello and her volunteer/victim prove to be natural performers. After he soaks the net, she makes him hike across the dirt schoolyard to empty the used water into the latrine. When she orders him back a second time to rinse the pan, he drags his feet in mock protest. Afterward, she quizzes her audience, rewarding correct answers game-show style with T-shirts that sport an ominously huge mosquito and the words: “Protect your family from malaria.”
The presentation is engaging and educational. But it nets just one sale, on top of eight sold at an earlier meeting. Having primed interest, the next step will be to find shopkeepers to stock the nets year-round. But although Akora pronounces himself pleased with the 1,500 nets sold in the monthlong rollout, that’s a paltry return on the time and effort he’s invested.
Pricing is one reason. Free-net advocates argue that Akora should just be giving the nets away, but the real problem here is that PSI-Uganda is charging $3 a net, a hefty subsidized price set under pressure from the government to protect the profits of private net importers. This is just the sort of hiccup on the ground that can derail the grandiose pledges made at such lofty settings as the recent G-8 summit.
In neighboring Kenya, net sales quadrupled when PSI dropped the price to 65 cents. And Malawi sells highly subsidized nets to pregnant women and children at prenatal clinics, which eliminates the added expense of getting out to each small village.
Both sides in the bitter debate over net distribution want clearer guidelines from the World Health Organization. The WHO should provide stronger leadership in steering countries toward models that have already been shown to work, and in changing direction — fast — when they don’t.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.