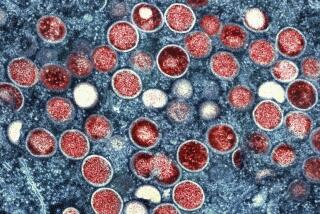
Ebola drug trials starting in West Africa as early as December

Three separate clinical trials for Ebola virus treatments are set to begin in West Africa as early as December, Doctors Without Borders announced Thursday.
The international medical aid group, also known by its French initials MSF, will host the trials in three of its Ebola treatment centers in the region, which has been ravaged by the deadly disease.
The trials will go forward with the goal of evaluating 14-day survival rates in patients, and will be open to all patients who consent.
“This is an unprecedented international partnership that represents hope for patients to finally get a real treatment,” Dr. Annick Antierens of Doctors Without Borders said in a statement. “MSF is taking part in these accelerated clinical trials to give people affected by the current outbreak a better chance of survival.”
To date, the Ebola outbreak in West Africa is believed to have killed 5,160 people and infected nearly 15,000 others. The death rate of the disease has been as high as 70% in the three most affected countries: Guinea, Liberia and Sierra Leone.
One trial being headed by the French National Institute of Health and Medical Research will test the effectiveness of the antiviral favipiravir in Gueckedou, Guinea. Researchers plan to enroll about 200 patients there.
The Antwerp Institute of Tropical Medicine is leading a second study of up to 100 patients in Conakry, Guinea, which will use blood and plasma therapies derived from the antibodies of recovered Ebola patients, a method endorsed by the World Health Organization and used to treat Dr. Kent Brantly and others in the United States.
A third study will look at the antiviral drug brincidofovir, an oral antiviral developed by drugmaker Chimerix Inc. of North Carolina. The University of Oxford, which is leading that study, has not decided where the trial will take place but has said it will involve 140 adults.
“Conducting clinical trials of investigational drugs in the midst of a humanitarian crisis is a new experience for all of us, but we are determined not to fail the people of West Africa,” said Peter Horby, a chief investigator on the University of Oxford trial.
Food and Drug Administration officials said last week that they believed randomized controlled trials, in which one group of patients receives treatment and a control group receives a placebo, should be used for Ebola drug trials in West Africa, calling it the “gold standard” for drug assessment. But researchers for all three trials have said they will not be using placebo control groups.
“We have an obligation to provide a lot more than hope,” said Dr. Luciana Borio, director of the FDA’s Office of Counterterrorism and Emerging Threats.
Horby says the decision to forgo a randomized controlled trial will help researchers quickly evaluate experimental drugs and prioritize testing.
“We’ve got a list of drugs, none of which we know if they work or not, and what we want to do is cycle through them quickly to get an answer,” Horby told reporters at a news conference Thursday in Geneva. “There’s substantial uncertainty about the feasibility of doing randomized controlled trials.... This is a very difficult humanitarian crisis with lots of uncertainties.”
Doctors Without Borders says researchers are in the final stages of developing test protocols and that the first trials could begin in a few weeks, as soon as early December. The trials are being designed so that researchers can make rapid adjustments and adaptations as conditions change. Initial results could come as early as February.
Favipiravir was used to treat Spanish nursing assistant Teresa Romero, who contracted the disease after caring for two Spanish priests who fell ill while working in West Africa and later died at the Madrid hospital where she worked. Romero survived and was released from the hospital last week.
Brincidofovir is designed to stop the virus from replicating. In the U.S., brincidofovir has made it to Phase 3 testing against two other viruses – adenovirus and cytomegalovirus. It has shown some promise against Ebola in lab experiments. The drug was used to treat Thomas Eric Duncan, the Liberian man who died at a Dallas hospital, as well as cameraman Ashoka Mukpo and Dr. Craig Spencer, both of whom survived.
The two drugs in the planned trials were culled from a list of experimental Ebola treatments flagged by the World Health Organization as priority drugs for testing.
Other promising drugs, including Zmapp, which has been shown in primate experiments to be effective against Ebola, were not included in the Doctors Without Borders-hosted trials, mainly because of the lack of availability, researchers said.
“We need to keep in mind that there is no guarantee that these therapies will be the miracle cure,” Antierens said in a statement. “But we need to do all we can to try the products available today to increase the chances of finding an effective treatment against Ebola.”
In the meantime, Doctors Without Borders is asking manufacturers of the drugs to scale up production to avoid gaps in treatment if the trials do show the medicines to be safe and effective against Ebola.
For more breaking news, follow me @cmaiduc