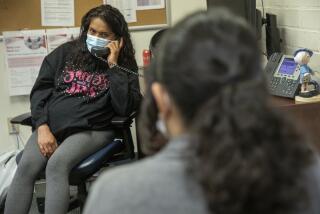California spent $4 billion on Medi-Cal for people who may not have been eligible, audit finds
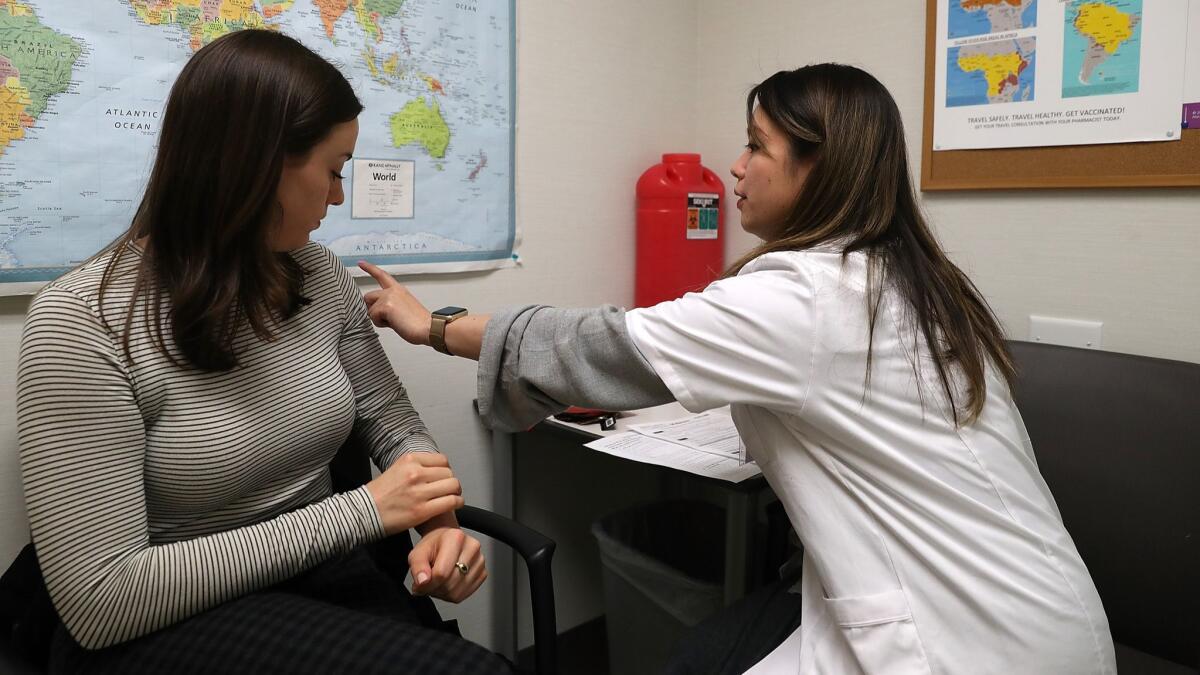
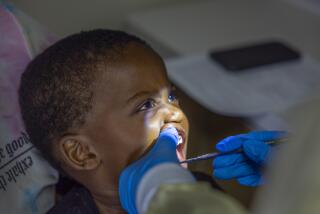
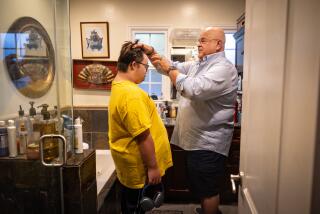
California spent $4 billion on Medi-Cal coverage between 2014 and 2017 for people who may not have been eligible for the government-funded health plan, according to a state audit released Tuesday.
Medi-Cal provides health coverage to 13.1 million Californians, approximately one-third of the state’s population. To qualify, a single adult must make less than $16,754 annually.
County workers typically determine whether someone is eligible for health coverage under Medi-Cal, then send that information to the state. But the records don’t always match up.
The audit found 453,000 beneficiaries who were marked as eligible in the state’s system, but not in the counties’ — indicating that they may not have actually been eligible for Medi-Cal. These beneficiaries may have died, moved or begun making more money and no longer qualified for Medi-Cal.
Yet the state’s Department of Health Care Services paid $4 billion to health plans and doctors for those patients’ medical care over four years. The audit found that 57% of the discrepancies lasted for more than two years.
In one instance, a Los Angeles County resident died in December 2013, yet the state continued to make monthly payments to the beneficiary’s Medi-Cal health plan until August of this year. The state ultimately paid the plan $383,000 for a person who the state “should have known was no longer in need of services,” according to the audit.
“Although Health Care Services has established a process for notifying counties of beneficiary records that require follow-up, gaps in this process allowed the problems we identified to persist,” State Auditor Elaine Howle wrote in a letter to the Legislature accompanying the audit.
The audit also found 54,000 people who were marked eligible in the county system but not the state, which may have delayed or made it difficult for them to access services for which they did qualify.
“These individuals may have experienced hardships in accessing health care services, as they would have been denied benefits until the system discrepancies were resolved,” the audit says.
The audit recommended that the department implement a better system by the end of the year and recover erroneous payments by June. The department said it agreed with the recommendations but could not comply with them within that timeline.
soumya.karlamangla@latimes.com
Twitter: @skarlamangla
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.