Op-Ed: How helpful will the new COVID booster really be?

Last week, the Food and Drug Administration authorized the use of Omicron-specific vaccines and the Centers for Disease Control and Prevention followed, recommending updated boosters for everyone age 12 and up who has gotten at least two doses of the original COVID vaccines. The message to a nation still struggling with the pandemic: The cavalry — in the form of a shot — is coming over the hill.
But for people familiar with the business tactics of the pharmaceutical industry, that exuberant messaging — and the lack of completed studies — has raised an array of still-unanswered concerns.
The updated shots clear the “safe and effective” bar for government approval. But in the real world, are Omicron-specific vaccines significantly more protective than the original vaccines so many have already had? If so, who would benefit most from the new shot? Since the government is purchasing these new vaccines, is the cost worth the unclear benefit?
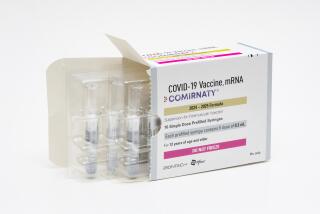
The CDC recommends people ages 12 and older get the new shots, which target the latest Omicron subvariants as well as the original coronavirus strain.
Some members of the CDC advisory committee that voted 13 to 1 to recommend the shot voiced similar questions and concerns, with one saying she only “reluctantly” voted in the affirmative.
Many said they set aside their desire for more information and better data out of fears of a potential winter COVID-19 surge. They expressed hope that the new vaccine — or at least the vaccination campaign to accompany its rollout — would put a dent in the number of future cases, hospitalizations and deaths.
That calculus is, perhaps, understandable at a time when about 500 Americans are dying of COVID each day. But it leaves healthcare providers in the impossible position of trying to advise individual patients whether and when to take the new vaccines, given the incomplete data.
Don’t get us wrong. We’re grateful and amazed that Pfizer/BioNTech and Moderna (with assists from the National Institutes of Health and Operation Warp Speed) developed an effective vaccine in record time to control the deadliest phase of the pandemic when thousands were dying each day. The pandemic isn’t “over,” but thanks in large part to the vaccines, most of America has gone back to a semblance of normalcy.
But as we move into the next phase of the pandemic, the pharmaceutical industry may be headed for familiar territory: developing products that may be a smidgen better than what came before, selling — sometimes overselling — their increased effectiveness absent adequate controlled studies or published data, advertising them as desirable for all when only some stand to benefit significantly, and, in all likelihood, raising the price.
This last point should be a big worry because the government no longer has funds to purchase COVID vaccines after the fall. Funding to cover healthcare provider fees for vaccination and community outreach has already dwindled. This could mean that updated boosters will largely benefit those with good insurance rather than those at highest risk for infection and progression to severe disease.
The FDA had no choice but to authorize the use of the Omicron-specific COVID shots, since its mandated task is just to determine whether a new drug is “safe and effective.” But the FDA cannot weigh in on important follow-up questions such as: How much more effective are the updated boosters than vaccines already on the market? In which populations? What increase in effectiveness is enough to merit an increase in price? (Many countries, such as the United Kingdom, perform such a cost-benefit analysis before allowing new medicines onto the market to negotiate a fair national price.)
Studies have confirmed that these lingering symptoms are real and take a real toll. The next big step will be to figure out exactly what causes them.
The new booster formulations are identical to the original COVID vaccines except for a tweak in the mRNA code to match the Omicron BA.5 virus. Although there is enough science to say these boosters are safe and at least somewhat effective, we lack robust data on their real-world utility. Pfizer and Moderna are just starting to study their updated BA.5 boosters in human trials. Research on earlier versions of Omicron-specific boosters indicated they would yield only slight improvement in effectiveness against symptomatic illness and severe disease compared with the original vaccine, with estimated bumps of about 5% and 1%.
Though the studies of the updated Omicron BA.5 boosters were conducted only in mice, the agency’s authorization is in line with precedent: The FDA clears updated flu shots for new strains each year without demanding human testing. But with flu vaccines, scientists have decades of experience and a better understanding of how increases in neutralizing antibody titers correlate with improvements in vaccine effectiveness. That’s not the case with COVID vaccines.
As population immunity builds up through vaccination and infection, it’s not clear that additional vaccine boosters, updated or not, will benefit all ages equally. In 2022, the United States has seen COVID hospitalization rates among persons 65 and older increase relative to younger age groups. COVID vaccine boosters seem to be cost-effective in the elderly, but they may not be in younger populations. The CDC’s Advisory Committee on Immunization Practices considered limiting the updated boosters to people 50 and up but eventually decided that doing so would be too complicated.
The government negotiated a price of $15 to $19.50 per dose of the COVID mRNA vaccine, which it has been paying during the pandemic. After these purchasing agreements lapse, analysts expect the price to triple or quadruple, and perhaps even more for updated yearly COVID boosters, which Moderna’s chief executive said would evolve like “an iPhone.”
To deploy these shots and dollars wisely, we need less hype and more information.
Céline Gounder, an infectious disease physician and epidemiologist, is a senior fellow at the Kaiser Family Foundation and the editor at large of public health at Kaiser Health News. Elisabeth Rosenthal, a physician, is editor in chief of Kaiser Health News and the author of “An American Sickness: How Healthcare Became Big Business and How You Can Take It Back.”
More to Read
A cure for the common opinion
Get thought-provoking perspectives with our weekly newsletter.
You may occasionally receive promotional content from the Los Angeles Times.