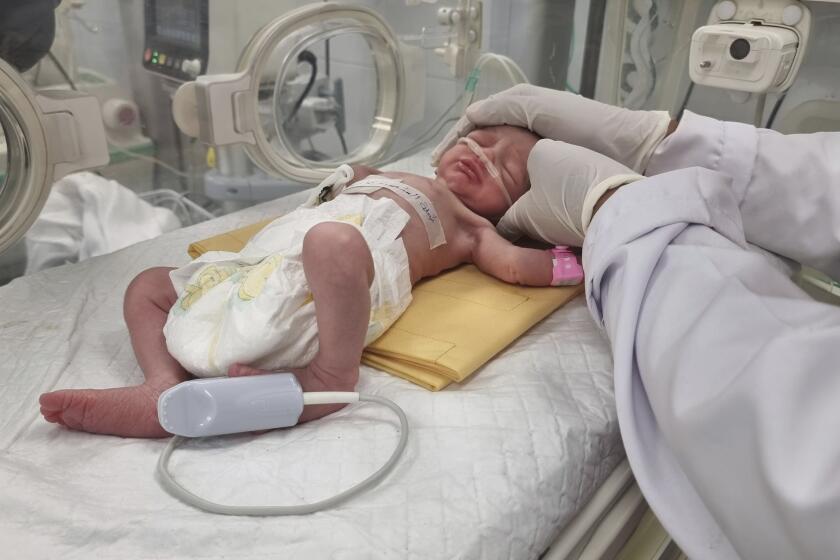
From Guinea to Dallas: Tracing the Ebola threat
It began in a village deep in the forests of southeastern Guinea, when a 2-year-old boy named Emile developed a mysterious illness.
Nothing, it seemed, could stem the child’s fever and vomiting, and he died within days. A week later, the illness killed his 3-year-old sister, then his mother, grandmother and a house guest.
The grandmother consulted a nurse before she died. Friends and family gathered for her funeral, and soon the illness was spreading down rutted dirt tracks to other villages and towns.
Local health officials were alarmed, but it would take nearly three months from the boy’s death in December to identify the culprit: the dreaded Ebola virus. By then, the lethal virus had reached Guinea’s bustling capital, Conakry, and there were suspected cases across the border in Liberia and Sierra Leone.
In June, the international aid agency Doctors Without Borders, one of the leading responders on previous Ebola outbreaks, warned that the virus was already out of control. But the World Health Organization disagreed. Doctors said they were told to avoid causing panic.
Not until August did the WHO concede that the worst Ebola outbreak on record had become an international public health emergency. By then, the deadly tide had reached Nigeria, Africa’s most populous nation, and casualties were beginning to arrive in the United States and Europe.
Ebola’s journey from the quiet village of Meliandou, through crowded, steamy, trash-strewn slums and on to Dallas with the arrival of 42-year-old Thomas Eric Duncan from Liberia last month, was a product of unfortunate geography, ramshackle health systems, and a combination of misunderstanding, denial and fear.
But there were also missed opportunities and questionable decisions that now add up to more than 3,400 dead and a caseload that is doubling about every three weeks, according to the latest WHO estimates.
The United States, Britain, France and other world powers have rallied in recent weeks, committing hundreds of millions of dollars and thousands of personnel to the effort to contain Ebola in West Africa. But the response is still far short of the nearly $1-billion effort that the United Nations says will be needed to get ahead of the epidemic.
Tens of thousands more could fall ill before the outbreak is brought under control, the WHO has warned. It may already be too late to keep Ebola from becoming endemic to the region — and as of now the virus could show up anywhere in the world, when the next Thomas Eric Duncan steps off a plane.
::
Ebola is one of the deadliest known viruses, with no specific cure and mortality rates that can reach 90%. Until now, it was mostly found in isolated rural communities, where it killed its victims so quickly that it didn’t have the chance to spread widely.
This outbreak is different. It struck in an area where the porous borders of Guinea, Liberia and Sierra Leone converge, amid a deeply impoverished and highly mobile population that moves frequently among the countries to visit relatives, go to markets — or attend funerals.
The most recent previous Ebola outbreaks, in 2012 and early 2013, took place thousands of miles away, in the Democratic Republic of Congo and Uganda. How it reached the continent’s western region is not known.
Scientists suspect the virus spends most of its time in fruit bats. It can also infect apes and has been known to move into humans when they hunt or butcher infected animals. The same risk could apply to handling infected bats, which are also hunted in West Africa.
Scientists believe the region’s upheavals have driven the bats from their natural habitats and closer to human settlements. When civil wars broke out in recent decades in Liberia and Sierra Leone, refugees poured over the border into Guinea. Trees were felled to build houses and make charcoal. Mining and timber companies also exploited the area’s resources.
It was, perhaps, only a matter of time before the virus found its way onto the hands of a crawling toddler. Once the boy became ill, his bodily fluids could infect others, becoming more dangerous as his symptoms worsened.
“Alarm bells might have gone off had any doctor or health official in the country ever seen a case of Ebola,” the WHO said in a recent retrospective on the outbreak.
But no one had, and they had neither the training nor equipment to avoid infecting themselves and other patients. Doctors, nurses and midwives began falling ill and dying.
In its early stages, Ebola’s symptoms are similar to any number of tropical diseases. When cases began to appear at the hospital in Gueckedou, the town where Emile’s grandmother went looking for help before she died, doctors suspected a more familiar culprit: cholera.
The hospital ran tests on nine samples; seven came back positive for cholera, the WHO said. But these patients all had fevers, which is not generally associated with the disease. Could it be malaria? The symptoms still didn’t add up.
As the mysterious illness began popping up in more locales, the local health authorities sought the help of foreign professionals, including the WHO and Doctors Without Borders.
Some began to suspect Lassa fever, a viral disease endemic to West Africa that can also produce bleeding.
Deeply worried, Doctors Without Borders officials forwarded the results of a medical investigation to Dr. Michel Van Herp, an epidemiologist with the group and one of the world’s leading experts on hemorrhagic fevers. He suspected Ebola.
At the time, there were no labs in Guinea equipped to test for the virus. So blood samples had to be flown to the Pasteur Institute in France. On March 20, Van Herp’s hunch was confirmed.
::
Three days later, the WHO published an official notification of a “rapidly evolving” Ebola outbreak in Guinea with 49 cases reported, including 29 deaths.
By this time, the WHO said, it had already shipped supplies of personal protective equipment to Conakry and had activated a state-of-the-art center to track the outbreak. Experts deployed by the WHO, Doctors Without Borders, the U.S. Centers for Disease Control and Prevention and others started to arrive within days.
There is no Ebola vaccine to contain an outbreak. Public health officials can only isolate the victims, then track down their contacts and monitor them for 21 days, to see whether they too develop symptoms. These methods were effective in previous outbreaks. But by this time, there were hundreds of contacts to trace.
It seemed the only thing more contagious than Ebola were the rumors spread about it. The disease was invented to get the government money, the rumors went. Ebola treatment centers were death traps. Inside, you would be administered green and yellow poison and your organs would be harvested.
In some areas, frightened and angry residents attacked health workers sent to disinfect public places or search for contacts, convinced that the deadly scourge was being brought by the strangers in yellow protective suits who carried loved ones away, never to be seen again.
Doctors Without Borders had to temporarily suspend operations in some Guinean villages when hostile groups of men began blocking the way, sometimes pelting them with rocks. Last month, a team dispatched by the Guinean government to the village of Womme to educate residents about Ebola was sent fleeing into the forest when a mob attacked, news reports said. Eight members, including officials and journalists, were killed and their bodies stuffed into latrines.
It soon became apparent that public messaging wasn’t helping. “Ebola is very serious, it destroys family and nation quick quick quick,” read one poster in Liberia.
“That kind of message doesn’t inspire patients to seek care, because it removes any hope that they might get better,” said Sean Casey of the International Medical Corps. When people did start to seek treatment, there weren’t enough beds. Only a few new patients were allowed in each morning — to replace those who died in the night.
Among those turned away was a desperately ill, pregnant 19-year-old in the Liberian capital of Monrovia. With her was Duncan. He helped take her to the hospital, and then carry her back into her house, where she died a few hours later.
::
One of the most tragic aspects of Ebola is its ability to exploit long-cherished customs and basic human instincts: A good Samaritan’s offer to help an ailing neighbor, a parent’s urge to cradle a sick child, or the wish to give lost loved ones a dignified farewell.
Ebola victims become more infectious as the disease progresses; a corpse, still full of infected body fluids, is like a “viral bomb,” experts say.
Around May 10, a woman famous for her traditional healing powers was buried in Koindu, a Sierra Leone diamond-mining town near the border with Guinea. As Ebola spread across the frontier, desperate patients had sought her help, and she, too, became infected.
The funeral drew mourners from near and far. At least 14 women were infected among the healer’s following, said Stephen Gire, a research scientist at Harvard University who studies the evolution of viruses.
The women probably handled the body, which tradition holds must be washed before burial. But many others would have placed their hands on the body. Health authorities believe as many as 365 Ebola deaths can be traced back to that one funeral.
One of those infected showed up two weeks later at a Sierra Leonean government hospital in Kenema after a bloody miscarriage. She was among the country’s first confirmed Ebola cases, but she survived.
The hospital collaborates with foreign laboratories to study Lassa fever, so doctors and nurses were alert to possible danger and avoided contaminating themselves. But they were soon overwhelmed, working round the clock to treat as many as 90 people at a time, Gire said.
One after another, they too fell ill. Many died. Among them was Dr. Sheik Humarr Khan, Sierra Leone’s leading virologist, who treated more than 100 Ebola patients before his death July 29.
Across the border in Liberia, two American missionaries who contracted the virus while working at a Monrovia hospital were fighting for their lives. Dr. Kent Brantly and Nancy Writebol, like a colleague who fell ill after them, would make full recoveries, after receiving experimental treatments that may have helped and follow-up care in the U.S.
So many healthcare workers have died in the outbreak that some hospitals have closed because the surviving staff members and patients are afraid to go in. The result is that even treatable diseases such as malaria are now claiming lives. How many, no one knows. Their victims simply disappear.
::
To the experts at Doctors Without Borders and a few other organizations, it was clear early on that this outbreak was different. The Geneva-based group issued its first public warning on March 31, saying the “unprecedented” geographic spread was greatly complicating the response.
For months, it lobbied behind closed doors to get regional governments and international health authorities to acknowledge what seemed obvious to its experts: The outbreak was out of control and would need many more resources than they could muster on their own.
But when the organization said as much publicly on June 23, it was criticized for doing so. “People were saying, ‘Look ... you are fueling the panic. It’s not good,’” said Brice de le Vingne, the group’s operations director. “We met resistance at many levels, including the WHO.”
Others also sounded the alarm. “Members of our team from very early on were shouting from the rooftops that this was not like other outbreaks,” said Gire, who worked with researchers at the Kenema hospital. “The WHO wasn’t listening. They were still trying to communicate to the public that it was under control.”
Officials at the WHO acknowledged a difference of opinion. “I don’t think we ever said we don’t want to cause a panic, but I don’t think we agreed that things were out of control, either,” said Daniel Epstein, a spokesman.
It would be another month before the caseload started to climb exponentially, he said. By then, the virus was racing through Monrovia, a densely packed city of more than 1.3 million people.
Airlines and transportation companies were refusing to service the affected countries, making it increasingly difficult to bring in supplies and personnel. Bodies were left in the streets for days because there weren’t enough teams in biohazard suits to collect them. Soon people would be buying forged death certificates in a bid to get loved ones a “decent” burial.
In the midst of the chaos, a Liberian Ministry of Finance official with U.S. citizenship ignored medical advice and boarded a flight from Monrovia to Lagos, Nigeria, on July 20. During the trip, he became violently ill. He died five days after landing in Lagos. Soon, another man would evade surveillance in Guinea and flee by road to Senegal, becoming that country’s first and only Ebola case.
As the caseload continued to grow, Dr. Margaret Chan, the WHO’s director-general, convened an emergency committee of experts, which on Aug. 8 declared the outbreak a public health emergency of international concern, finally triggering a worldwide hunt for resources.
The following month, the U.N. Security Council unanimously approved a resolution declaring Ebola a threat to international peace and security, and calling on member states to urgently send help. But it was late. “The disease got out of hand, and everyone came in after that,” said Tolbert Nyenswah, Liberia’s assistant health minister.
The countries’ leaders resorted to increasingly desperate measures, putting entire districts under quarantine. Clashes erupted when Liberian security forces sealed off a sprawling seaside slum in Monrovia for 11 days, after residents looted an Ebola holding center and chased away sick patients.
The draconian move, which was imposed against the advice of the WHO and Doctors Without Borders, fueled a pervasive mistrust of government structures and helped drive Ebola further underground.
“People will say, ‘It’s typhoid,’” said Bishop Amos Sesay, who is part of a team that traces the contacts of Ebola victims in the Paynesville neighborhood, outside Monrovia. “Our team lost a lot of opportunities because of misinformation.”
If relatives of Marthalene Williams hadn’t insisted that she had malaria, their Paynesville neighbor, Thomas Eric Duncan, might not have helped carry her to a taxi or accompanied them as they searched the capital for a hospital or clinic that would take her.
Four days later, on the afternoon of Sept. 19, Duncan arrived at Monrovia’s airport to catch a flight to the United States, beginning with a connecting flight to Brussels. Like all travelers exiting the Ebola zone, Duncan’s temperature was checked by a Liberian official who had been trained by CDC experts. Duncan’s temperature was an unremarkable 97.3. He filled out a form crafted by the CDC and Liberian authorities to alert them to potential Ebola cases. It asks travelers whether they have had contact with people who might have Ebola.
It’s not known whether Duncan suspected that Williams had Ebola, but health officials in Liberia say he did not disclose his encounter with her. He was waved onto the jet, and then spent several hours on a layover at the Brussels airport, a busy hub that last year handled more than 19 million passengers.
Duncan then flew out on United Flight 951 to Washington Dulles International Airport. He arrived about 2:30 p.m. on Sept. 20, then boarded United Flight 822, which landed in Dallas about 5:30 p.m.
From there, he got a ride in a private car to the northeast Dallas home of his girlfriend, a Liberian nursing-home worker named Louise Troh, the woman’s daughter said.
Troh, who is a U.S. citizen, met Duncan years ago in Ivory Coast, where the two had gone to flee Liberia’s civil war, according to the daughter, Youngor Jallah.
When Duncan arrived, the family did not throw a party, Jallah said — her mother had to work. Staying with them in Apartment 614 at the Ivy Apartments, a second-floor unit in the city’s Five Points neighborhood, were a 13-year-old son, Timothy Wayne; a family friend, Jeffrey Cole; and Oliver Smallwood, one of Duncan’s relatives.
Jallah, who also works in a nursing home, lives in a nearby apartment complex. She brought her children over one night when she and her husband were both working. Another night, she brought Duncan a treat: a West African dish known as palaver stew. But he did not have much of an appetite; he was starting to feel sick.
On Sept. 25, Jallah’s mother took him to Texas Health Presbyterian Hospital, where they informed the medical staff that he had been to Liberia, Jallah said.
The hospital acknowledges that information about his time in Africa was recorded, but said his symptoms, including a fever and abdominal pain, weren’t specific to Ebola. He was sent home with antibiotics.
Three days later, Jallah went over to take care of Duncan while her mother was at work. She fixed him tea and crackers, but when she asked him to come eat in the living room, she said, “He told me he was cold and I should take the tea to his room.”
Worried, she drove to a nearby Wal-Mart and bought him a brown comforter, which he crawled under while still wearing two shirts, shorts and socks. She thought at first that he might have malaria, or some other tropical disease, but not Ebola.
Then she took his temperature — 100.4 — and noticed that he was using the bathroom frequently. Most troubling of all, she had seen redness in his eyes that alarmed her. “I told him it was not right.”
So she called 911. When paramedics arrived, they headed straight toward Duncan. “I told them to stop, because they were going to rush,” she said. “I said, ‘He’s from a virus country — Liberia — so you need to wear your masks.’”
She didn’t mention Ebola because, she said, “I wasn’t sure — I’m not a doctor.”
She followed as paramedics loaded Duncan into the ambulance, then drove ahead of it with Cole, planning to meet Duncan at the hospital. They brought his new brown comforter.
At the hospital, the staff directed them to Duncan’s room, No. 42. But there was a sign on the door that said “isolation.”
“The nurse at the station said, ‘You cannot go in there,’” Jallah recalled. “I said, ‘Can I give him the blanket?’ She said no.”
molly.hennessy-fiske@latimes.com
Dixon reported from Monrovia, Zavis and Morin from Los Angeles and Hennessy-Fiske from Dallas. Times staff writers Tina Susman in New York and Deborah Netburn in Los Angeles contributed to this report.
More to Read
Start your day right
Sign up for Essential California for news, features and recommendations from the L.A. Times and beyond in your inbox six days a week.
You may occasionally receive promotional content from the Los Angeles Times.