Column: An L.A. doctor races to cure deadly diseases and worries about Trump plan to cut NIH funding

President Trump said he would stop funding 19 agencies entirely under his budget blueprint. (March 16, 2017)
Michael Yeaman’s lab on the Harbor-UCLA Medical Center campus in Torrance is loaded with bacteria, and it’s been that way for a quarter of a century.
Yeaman is a bug detective. To be more technical, he’s a medical science investigator. You should not talk to him if you’re a hypochondriac, because you’ll crawl into a bubble and zip it shut.
“Currently there is an enormous threat of drug-resistant infections,” said Yeaman, chief of molecular medicine at Harbor-UCLA.
Often, these infections are picked up at medical facilities. You go to the hospital for treatment minor or major, and you end up with an infection antibiotics will not cure.
The annual death toll in the U.S. is in the tens of thousands.
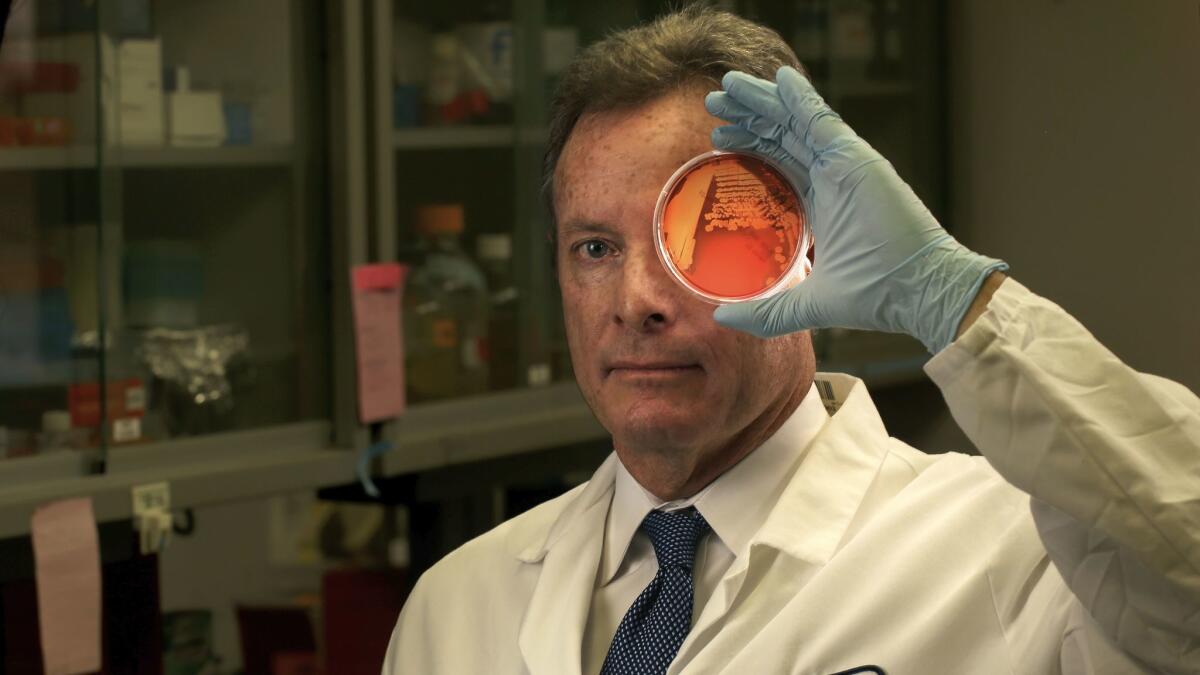
We are at war with bacterial and fungal pathogens, and antibiotics can’t keep pace because the pathogens have been learning how to resist their enemies for billions of years. In hospitals, where there is concentrated use of antibiotics, the resistant pathogens put their advantage to use.
“We are barely keeping pace, in my opinion, or we have a razor-thin edge,” Yeaman said. “If you’re using modern vernacular, we’re sort of at a tipping point in my opinion.”
I went to see Yeaman because much of his work — which includes some promising breakthroughs — is funded by the National Institutes of Health. People in medical science shivered last week when President Trump — who is keen on neither art nor science — proposed a 20% cut ($5.8 billion) in NIH funding. Maybe Trump thinks of the cut as a down payment on his plan to increase military spending by $54 billion, even though we already spend more than the next eight nations combined.
Yeaman does his research at LA BioMed, a nonprofit research institute that is affiliated with Harbor-UCLA and has been coming up with medical advances for more than 60 years. The list includes breakthroughs in treatment of Tay-Sachs disease, thyroid deficiency in infants, therapies for metabolic disease and for end-stage renal disease, and advances in understanding the link between menopausal hormone therapy and breast cancer.
“Our budget is probably close to 40% funded by the NIH, and we have 30 to 35 research groups working on 600 projects,” said David Meyer, president and chief executive of LA BioMed.
L.A. County Supervisor Mark Ridley-Thomas said medical research in Los Angeles is crucial not just to the county, “but to the entire world,” and he called Trump’s hatchet plan “completely foolish.” The investment in research not only pays off in greater public health, Ridley-Thomas said, but it also bolsters the U.S. stake in a growing global industry.
At the moment, Trump’s plan is nothing more than a proposal Congress will kick around for a while. Government-funded research has always had critics who see it as play money for scientists, or an advance on private profit for Big Pharma.
The government shouldn’t throw money at risky ventures, Meyer said, but when it comes to finding cures for disease, “planting the seeds and fertilizing research and development is major. If that goes away, we’re all” in trouble.
Yeaman said when he went into medicine, he chose research because a physician nobly treats one patient at a time, but with a breakthrough, a medical investigator can have an impact on multitudes.
Yeaman said he feels like he’s in a race, and always has been. Research requires momentum, and any interruption can delay discoveries and prolong the process of clinical trials and getting drugs to market, even as lives are lost. We need to not only sustain current research, he said, but also expand it.
“We know there are emerging pathogens, things we’ve never seen before, like the Zika virus and different strains of flu virus,” Yeaman said.
Penicillin and other “cillins” have a common structure, and bacteria have cracked the code, thanks in part to our overuse of them. They see an antibiotic and say, “You know, I’ve seen that before,’ and it’s a shorter time” before the bug resists the cure. Meanwhile, an aging population means more medical treatment, and more opportunity for infection.
The NIH awarded a $10-million grant to Yeaman, and colleagues at UCLA’s Westwood campus and Duke University, to decode the relationship between pathogens and the people they infect. We need to know more not just about the pathogens, Yeaman said, but why some immune systems are better able to resist them.
In 2003, Yeaman and his team — including UCLA’s Dr. Jack Edwards and others — had what he called a Eureka moment while studying the potentially lethal fungus known as Candida, another scary hospital-acquired pathogen. Candida produces a protein that attaches itself to the inside of human blood vessels, and Yeaman’s team discovered that the protein was structurally similar to the protein in MRSA, or methicillin-resistant staph infection.
This led to development of a single vaccine to treat both pathogens, and in the second of two clinical trials, the vaccine was effective on 30% to 40% of the patients infected.
“It was the first vaccine ever to address a fungal organism,” Yeaman said, and this led to new information on how to attack Candida in life-threatening cases. “It’s the first step to something that could be a massive breakthrough.”
But that will take time, a bigger clinical trial and more research support. Sometimes, venture capital investments are available, but Yeaman is hoping the NIH survives budget cuts in good enough shape to help fund the next phase of his project.
Yeaman, by the way, is an accomplished composer, pianist and guitarist, with an interest in the intersection of science, art and healing. I noted that he is both a scientist and a musician at a time when science and the arts are under attack.
Naturally, he defended both.
“Saving lives and improving lives is meaningful and important and necessary,” he said, but art, poetry and music are gifts of their own. “It’s one thing to keep people alive. It’s another thing to offer them something to live for.”
Get more of Steve Lopez’s work and follow him on Twitter @LATstevelopez
ALSO
Why Trump’s budget proposal may not be a blueprint for economic growth
Gun injuries cost Americans $730 million a year in hospital bills
This is where all of California’s House Republicans stand on the GOP healthcare bill
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.











