Flu could be far worse in L.A. this season. Here’s why

More than 2½ years into the battle against COVID-19, officials are warning that this fall and winter could see the rebound of a more traditional foe: the flu.
Influenza has been largely dormant the last two seasons, a development some attribute to the infection-prevention protocols put in place to ward off the coronavirus.
But with measures such as mandatory masking, physical distancing and limitations on business and social activities having been put aside amid improved pandemic conditions, California could be in line for a more active flu season this year.
“It’s not clear what this fall and winter will be like. However, because there are fewer masks being worn and there’s more intermingling, we’re likely to see much more influenza than we’ve seen in the past two years,” Los Angeles County Public Health Director Barbara Ferrer said.
“Getting both vaccines at the same visit increases the chance that a person will be up to date with their vaccinations,” the CDC says.
This raises the possibility of which some officials have previously warned but that has yet to materialize in the United States: a landscape in which the coronavirus and the flu are circulating at elevated levels simultaneously.
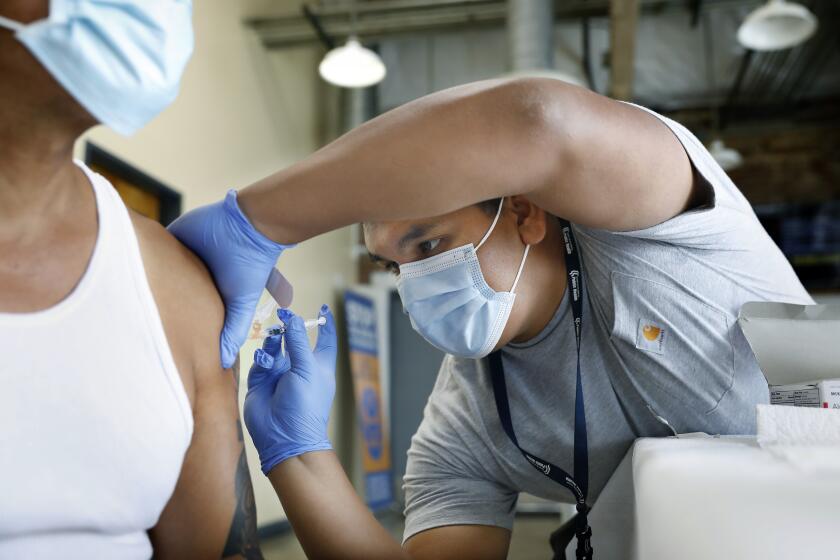
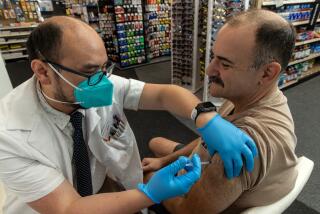
“We could experience lots of transmission of both influenza and COVID at the same time,” said Ferrer, who urged residents to get both their annual flu shot and the updated COVID-19 booster that is designed to protect against the most recent circulating coronavirus strains.
One warning sign comes from Australia, which saw its winter peak of lab-confirmed flu cases hit a level not seen since at least 2017, according to data Ferrer presented. Australia, in the Southern Hemisphere, has its autumn begin in March, and its winter begins in June.
“They experienced a relatively severe flu season dominated by [the variant] H3N2, which is what’s circulating here. And it also started earlier than usual this year, in late April, and then ... cases increased sharply. The flu season also ended earlier than usual, with cases trailing off considerably by the end of July,” Ferrer said.
California sees COVID retreat now, but new variants bring caution as colder weather nears.
According to the California Department of Public Health, flu activity typically begins to ramp up nationally in late November or December. As a result, officials recommend everyone 6 months and older get a flu shot sometime this month — since it takes a few weeks for the vaccination to reach full potency.
Dr. Peter Chin-Hong, a UC San Francisco infectious diseases expert, has suggested that those eligible get both the flu shot and the updated COVID-19 booster no later than October, or as soon as possible after that.
“If you’re trick-or-treating for Halloween and you haven’t gotten your flu shot or your booster yet, that’s probably the time that you should really run out and get it,” he said.
As with COVID-19, older people are at greater risk of developing severe disease from the flu. Also at heightened risk are those who are immunocompromised, who have underlying health conditions or whose work requires them to be in contact with a lot of people, especially in situations where ventilation is poor.
“Flu vaccinations keep people out of the hospital, keeping our healthcare system open to help with other illnesses during the winter,” Dr. Tomás Aragón, California’s public health director, said in a statement.
Residents can visit MyTurn.ca.gov to book a flu vaccine appointment or search for a walk-in clinic. Officials say you can receive both a flu vaccine and an updated COVID-19 booster during the same visit.
While there’s no shortage of pundits, politicians and other prognosticators clamoring to declare the end of the pandemic, the ultimate call is up to the World Health Organization.
It’s possible there’s a larger pool of people in the U.S. more susceptible to the flu this fall and winter, given that the low rate of infections during the last few years gave people less chance to develop immunity outside of getting a flu shot, Ferrer said.
During the 2020-21 season, a bit more than 49% of Californians ages 6 months and older received the flu vaccine, according to estimates from the U.S. Centers for Disease Control and Prevention.
Nationwide, there is an average of roughly 35,000 flu deaths each year. That has ranged from an estimated 12,000 deaths during the 2011–12 season to 61,000 deaths during the 2017–18 season.
The last two winters in L.A. County have been very quiet for flu, in large part due to mandatory masking orders and a general atmosphere of caution amid steep seasonal surges of coronavirus cases and hospitalizations.
Once L.A. County ended its universal public indoor mask mandate in early March, flu cases started climbing and peaked in May — unusually late in a typical season. At the height, about 15% of respiratory specimens at L.A. County’s sentinel surveillance labs detected flu.
As officials in California and beyond try to assess how severe a fall-and-winter coronavirus wave may be, one key factor is the growth of several new subvariants now emerging.
Officials say the fall and winter seasons provide opportunities for the spread of both the coronavirus and flu, in part because people spend more time indoors as temperatures cool and daylight hours shorten.
“Starting around Halloween and lasting through New Year’s Eve, families and friends tend to gather more often and travel farther to see each other for the holidays,” Ferrer said. “As a result, people spend more time socializing indoors, where respiratory viruses can accumulate more and can jump more easily from person to person, especially if the ventilation is poor.”
Increasing travel for the holidays, she added, means “that respiratory viruses can travel longer distances, hopscotching across the country and the globe.”
Cooler weather also increases the viruses’ ability to spread.
“As the days get shorter in the winter and the air is cooler, it holds less water on average, and the absolute humidity in the air tends to be lower,” Ferrer said. “When absolute humidity gets lower, aerosolized droplets containing virus tend to contain less water too. They become smaller, lighter, and they can travel farther.”
That means cooler temperatures allow viruses to remain viable in the air longer, ready to infect more people. Cooler air also tends to put more strain on our respiratory systems, and there’s less blood flow and less ability to clear out invading viruses, Ferrer said.
A recently published study that examined weather and COVID case rates from 455 cities across 20 countries for much of 2020 found that “overall lower temperatures, and lower absolute humidity, were associated with these higher COVID-19 case rates,” Ferrer said.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.