Missionaries deserved access to untested Ebola drug, expert writes

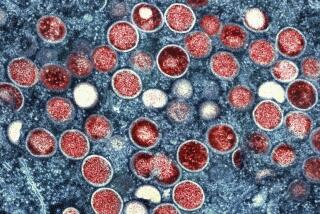
They were given drugs never before used on humans, and then flown to the United States amid fears that they would spark a new outbreak of the dreaded Ebola virus.
Roughly two weeks after a pair of American missionary workers were evacuated from Liberia, debate continues over the decision to treat them with the experimental drug ZMapp, as well as their admission to a special containment ward at Emory University Hospital, in Atlanta.
In two related opinion papers published Monday in the Annals of Internal Medicine, experts wrote that fears of Ebola spreading in the United States were unfounded, and that it was reasonable to treat the infected medical workers with an experimental drug.
However, that did not necessarily mean that the same experimental drug should be used to combat the epidemic in West Africa, an author wrote.
“Ebola virus has ignited some of the worst fears in a globalized world,” wrote Nancy Kass, a professor of bioethics and public health policy at Johns Hopkins Bloomberg School of Public Health.
“The disease spreads quickly, with high mortality, and is crossing borders. More than half of those afflicted have died. Among confirmed cases are two Americans who have become the focus of public attention, because of their heroism, and for the extraordinary measures taken to secure them optimal medical care.”
Kass wrote that medical workers who volunteer for service in West Africa deserved special treatment. Failure to offer state-of-the art medical care to foreign health workers would make it much less likely that they would ever volunteer to treat Ebola patients, Kass argued.
Since Ebola is spread through contact with bodily fluids, healthcare workers face an elevated risk of infection.
“It would be unconscionable to send doctors and nurses to Africa now without Hazardous Material (HazMat) suits; and it would be equally unconscionable not to assure them that, should they contract Ebola, they will be airlifted home to receive the best care available,” Kass wrote.
Kass wrote that because the medical worker’s chances of dying were greater than surviving, and because they likely understood the risks of taking an experimental drug, the decision to use ZMapp was reasonable.
“Which leads to one final question,” Kass wrote. “If it was reasonable to treat these two Americans, shouldn’t the experimental treatment also be provided to African patients? Callous as it may seem, the answer is no, or at least, not yet.”
Kass wrote that giving an experimental treatment to an individual patient was different from deciding to provide it to an entire community, especially when it remained unclear whether the drug actually worked.
In the second opinion piece, lead author, Dr. Carlos del Rio, an infectious disease professor at Emory University School of Medicine, and his colleagues, argue that the American public should not fear the spread of Ebola in the U.S.
“Two recently airlifted patients to Emory University Hospital ... have brought an unprecedented level of media attention to this illness as well as concern for spread in the U.S. population,” Del Rio and his colleagues wrote.
“However, such concerns are unfounded as Ebola ... is not transmitted by a vector and, while highly infectious, is only acquired by direct contact with infected secretions. Even if cases are imported, the likelihood of further transmission beyond the index patient is close to zero as hospital infection control practices are a very effective barrier.”
The authors said that hospitals however should be prepared to isolate patients who show signs of infection and who have recently visited West Africa.
Follow @montemorin for science news