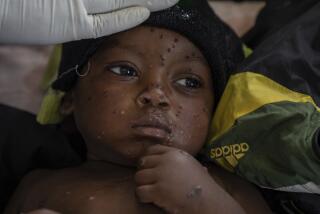
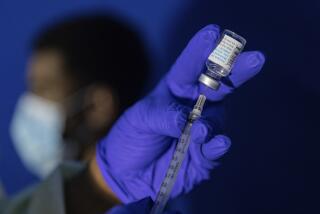
Every day, 170 young people are infected with HIV in West and Central Africa, and many can’t afford treatment
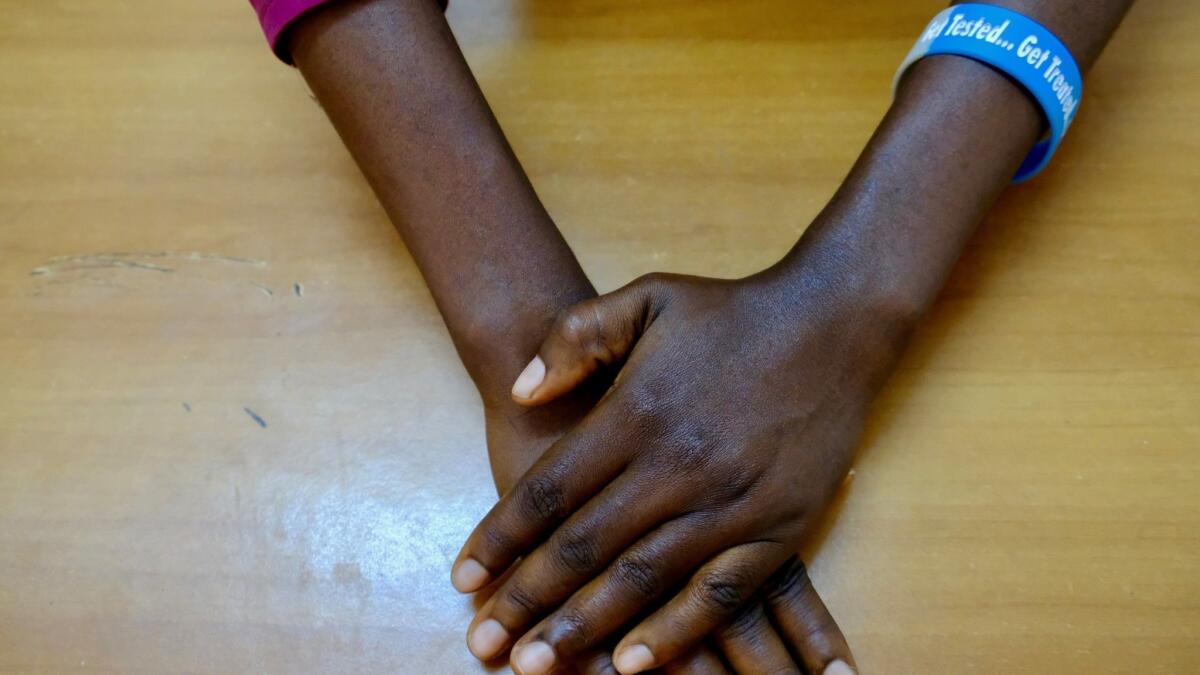
It started with aches, pains and a malaise that Adeola Ajetunmobi tried hard to ignore. With her father out of work and her mother hawking pens and other small items in Lagos, their family barely had enough money to survive. Paying for medical expenses simply wasn’t in the budget.
So for months, Ajetunmobi quietly suffered, even as her skin erupted into a constellation of painful sores.
A concerned friend finally lent the 19-year-old money for bloodwork, and when her results came back, they shocked her: She had HIV. Her illness was so advanced, it would take six months in the hospital for her to get back on her feet.
“At school, they talked about HIV,” Ajetunmobi said. “I thought I was doing everything right.”
She never found out how she contracted the virus, and her boyfriend, who tested negative, left her after her diagnosis. She was only able to pay for her medical expenses with help from neighbors and a sympathetic nurse who petitioned for her to have some treatment for free. But her story is not uncommon.

Sub-Saharan Africa is home to 86% of the world’s HIV-positive children and adolescents. And in West and Central Africa, 80% of infected children are not receiving antiretroviral therapy, making it the region with the world’s lowest rate of access to that type of treatment. According to the most recent UNICEF and UNAIDS research, the crisis there is becoming more fatal for young people: The number of 15- to 19-year-olds dying of AIDS in West and Central Africa increased by 35% between 2010 and 2016, even while it fell elsewhere across the continent.
The rate of new infections is falling but at a slower rate: In the same age group, 170 people are infected with HIV in the region every day.
The regional differences reflect a disparity in funding. In recent years, almost five times as much money was invested in HIV/AIDS response in eastern and southern Africa than in West and Central Africa, creating a disparity that has left West and Central Africa lagging behind on both treatment and prevention. Many young people now dying of AIDS in the region may have been born HIV-positive but have not had the resources to diagnose and treat the virus before it was too late.
The threat of untreated HIV looms particularly large in Nigeria, Africa’s most populous nation, and home to the second-largest population of HIV-positive people in the world (South Africa has the largest). More than half of the West African country’s 190 million people are under the age of 30 — but much of the money put toward treatment is focused on adults, leaving youth at risk. And it’s girls and young women who bear the greatest burden of HIV infection, as they make up the majority of 10- to 19-year-olds infected with HIV in the region, often contracting the virus through unprotected sex.
Experts say the infection rate is largely fueled by a lack of infant diagnoses and unequal access to testing and treatment. (There had been fears that President Trump’s proposed $800-million cut to the President’s Emergency Plan for AIDS Relief could lead to millions of additional deaths, but funding was ultimately restored in Congress.)
Despite efforts to create public awareness about HIV, fear of stigma still prevents many Nigerians from sharing their status, even though disclosure would potentially protect those around them.
Dr. Anslem Audu, an HIV/AIDS specialist working with UNICEF in Nigeria, said some parents, fearing ostracization, keep their children’s HIV status a secret from the youngsters even as they give them antiretrovirals — which the children may believe are vitamins or other medications — to keep them alive. When those children become sexually active teenagers, they can put others at risk of contracting the virus.
“Why don’t they want to disclose?” Audu said. “Because they don’t want the child to speak out and let people know he is HIV-positive, then neighbors will know there is HIV in the family and before you know it, they will start stigmatizing them.”
One 18-year-old woman who asked that her name not be used because she is not open about her HIV-positive status, was probably born with the virus. She grew up in an orphanage and, from a young age, took antiretrovirals without knowing what they were. It wasn’t until she was 16 that she asked the missionaries she stayed with why she had to keep taking medication.
“These drugs, you have to take them in order for you to survive, in order for you to do normal things that other people are doing,” she said they told her. “When I said, ‘OK, what is the reason for the drugs?’ They said it was HIV.”
HIV unawareness is compounded by a Nigerian law that prevents minors from seeking blood tests without their guardians’ consent, except under special circumstances. Even teens who recognize the threat of HIV will avoid testing because they do not want their parents to know they are sexually active.
Still, many high schools in Nigeria mandate HIV testing for their students. The 18-year-old found this out the hard way when she enrolled in a boarding school and was asked to leave when her test came back positive. With help from a nonprofit called Positive Action for Treatment Access, she has since found a new school and learned more about her own health. Most of her friends still don’t know about her diagnosis, but she said she practices abstinence and makes sure she is quietly taking measures to prevent transmission.
But it is Ajetunmobi’s life post-diagnosis that illustrates why so many parents want to hide their children’s positive status. Her father died of unrelated causes soon after she was diagnosed, and when she tried to move in with his side of the family in Lagos after she was released from the hospital, they told her that they didn’t want an HIV-positive person in the house. She stayed outside their compound instead, sleeping just steps away from the street, and begging during the day to earn enough to pay for her medications. “It was for survival, that is the reason why I was doing that,” she said.
Then, on one stormy night, she asked her relatives’ neighbor to let her stay inside his house to escape from the rain. He agreed, then raped her. “I was screaming and there was no one to save me,” she said.
Ajetunmobi soon realized she was pregnant, adding another layer of worry and distress to her already difficult situation: Would her child be born with HIV?
Prevention of mother-to-child transmission is one of the areas where the region has most improved. The number of new infections in children ages 0 to 14 in Nigeria has been reduced by 16% in recent years, although Nigeria still accounts for the largest number of new infections among children in all of West and Central Africa.
Two years ago, Ajetunmobi, now 23, gave birth to a healthy baby girl. Still, much of her family continues to ostracize her. She and her daughter have no choice but to squat in a single room they share with seven people.
But through the nonprofit , Ajetunmobi found access to free antiretrovirals. She also participates in support groups that connect young people living with HIV and has found comfort in becoming more open about her status.
“It’s people like me. I see them as my family, my blood,” she said. “When I go to the support group, I don’t want to go back home.”
ALSO
Two years after West Africa was declared Ebola-free, health and financial burdens persist
As Africa grows more prosperous, obesity grows as a problem
As parts of Zambia beat back malaria, the nation sets a lofty goal: zero transmissions
O’Grady is a special correspondent.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.