Editorial: The ethics of creating GMO humans
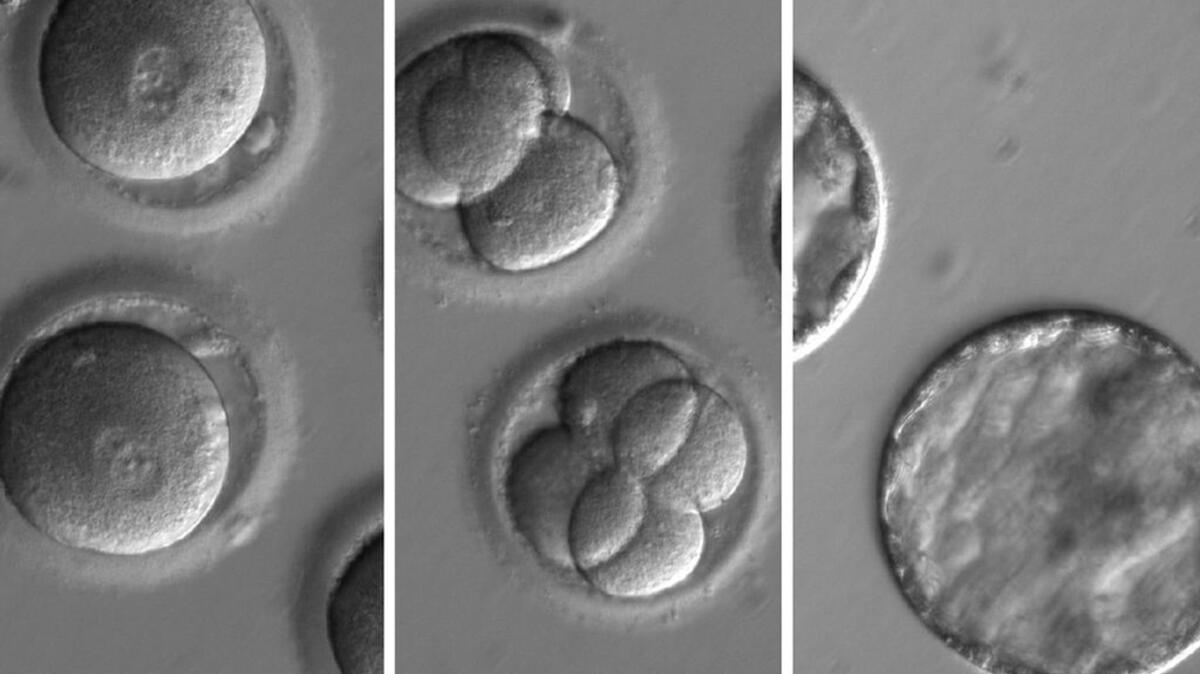
In a process that can be likened to the creation of GMO crops, scientists have edited genes in human embryos in order to eliminate a mutation that causes thickening of the heart wall. The embryos were created solely for the scientists’ study and will not be implanted. Nonetheless, the research offers hope that in years ahead, science could prevent many serious genetic diseases at the stage in which people are a microscopic cluster of cells in a petri dish. What’s more, because those edited genes would be carried forth into new generations, the disease might eventually be eliminated altogether.
Is this a glorious new frontier or a troubling situation? Unequivocally, the answer is yes to both.
The research results by an international team of U.S., Chinese and South Korean scientists were enormously exciting medically. Beyond the technical achievement involved, the team’s work hastened the arrival of a revolutionary form of treatment: removing genes that can lead inexorably to suffering and premature death.
Public policy and the field of bioethics have not caught up with the science of genetic intervention.
But there is also a great deal we still don’t know about how minor issues might become major ones as people pass on edited DNA to their offspring, and as people who have had some genes altered reproduce with people who have had other genes altered. We’ve seen how selectively breeding to produce one trait can unexpectedly produce other, less desirable outcomes. Remember how growers were able to create tomatoes that were more uniformly red, but in the process, they turned off the gene that gave tomatoes flavor?
Another major issue is the ethics of adjusting humans genetically to fit a favored outcome. Today it’s heritable disease, but what might be seen as undesirable traits in the future that people might want to eliminate? Short stature? Introverted personality? Klutziness?
To be sure, it’s not as though everyone is likely to line up for gene-edited offspring rather than just having babies, at least for the foreseeable future. The procedure can be performed only on in vitro embryos and requires precision timing.
But even with this early study, problematic issues already are evident. Gene editing isn’t the only method to protect against certain hereditary conditions such as hypertrophic cardiomyopathy, which was “edited out” in this study. Children stand a 50% chance of inheriting the condition; if a couple produces several embryos through in vitro fertilization, half of those already would theoretically be free of the mutation, and those are the ones that would be selected for implantation. Gene editing made the process more efficient, but it did not offer hope where there was none, Jennifer Doudna, a molecular and cell biologist at UC Berkeley, observed.
In fact, six months ago, the National Academies of Science, Engineering and Medicine recommended that scientists involved in germline editing — that is, making changes that would be passed down to future generations — should limit their work to diseases for which there are no other reasonable treatments. The most recent embryo study began before that recommendation was delivered.
That’s emblematic of the real problem: Public policy and the field of bioethics have not caught up with the science of genetic intervention. Yes, federal money can’t be spent on research involving human embryos even when they are still at the stage of a clump of undifferentiated cells. FDA approval would be needed for any actual human therapies, which would be years off.
Still, the technology is advancing more rapidly than society’s discussions about human genetic engineering, the specter of eugenics and even the seemingly mundane topics of who will own the patents on customized genes and who will have access to gene editing once it is approved.
The answers aren’t easy, but the discussions have to take place and decisions need to be made, probably through an international convention that includes governments, researchers, physicians and consumer advocates. Taking the research to the next level should mean experimentation with animals rather than humans. They should then be followed for generations to see whether unexpected health issues arise. Gene editing on humans should be introduced one step at a time, starting with the most disastrous diseases and conditions that cannot be tackled in any other way, then tracked long term to ensure safety.
We all would love to eliminate disabling deformities, painful conditions that shorten lives or genetic mutations that predispose us to various fatal diseases. Although science has a long way to go before such miracles are achieved, research is moving fast. It’s paramount that we get human gene editing right rather than just getting it soon.
Follow the Opinion section on Twitter @latimesopinionand Facebook
More to Read
A cure for the common opinion
Get thought-provoking perspectives with our weekly newsletter.
You may occasionally receive promotional content from the Los Angeles Times.