California’s early vaccine rollout was chaotic and filled with problems. Here’s what went wrong

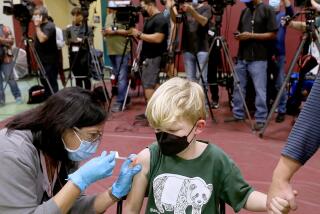
Some twentysomethings with social media jobs are getting COVID-19 vaccines before senior citizens.
More than a third of the Pfizer and Moderna doses in California appear to be unused, but health officials say they can’t give out shots more quickly.
And problems with the state’s data systems have left officials in the dark about how many doses have actually been administered, clouding the picture of the state’s progress.
California has administered more than 3.45 million injections, by far the most in the country, but for weeks ranked among the slowest per capita in vaccinating its population and in using up the doses allocated by federal officials, data show.
By Monday, about 7.2% of California residents had received a first dose, and 60.9% of the state’s vaccine supply had been administered — a dramatic improvement from a week ago, but still behind other big states like Texas, Illinois and New York, and only slightly ahead of Florida.
The Golden State’s early sluggish rollout defies one easy explanation. For weeks, Gov. Gavin Newsom and public health officials limited vaccine access to only health workers and nursing homes, and data snafus complicated the picture of how vaccination efforts are progressing. Experts say the structural barriers of such a large, decentralized state that leaned heavily on 61 local health departments to administer the doses also complicated the response.
The biggest and most persistent problem, though, has been beyond the state’s control. Officials have been hamstrung by vaccine supply shortages and lack of predictability from the federal government and the manufacturers.
“The supply crunch creates this huge unmet demand, which creates chaos,” said Andrew Noymer, associate professor of public health at UC Irvine. “There are just layers and layers of logistical issues that we have today that we didn’t have in previous vaccination campaigns.”
Experts say about most Americans will need to be vaccinated to bring the coronavirus pandemic under control. Track California’s progress toward that goal.
Texas and Florida, early leaders in distributing a high share of their vaccine doses, opened up vaccinations to more people, including senior citizens, in December. New York leaned on large public hospital systems to administer doses to their workers and the general public, and Gov. Andrew Cuomo threatened to fine them or cut off their supplies if they vaccinated too slowly.
California’s initial vaccine plan mirrored federal recommendations by prioritizing nursing home residents and 2.4 million healthcare workers. But as states like South Dakota, West Virginia, Texas and Florida moved on to new groups of patients, California trailed behind.
California has now adopted an age-based distribution system, and the share of vaccine doses used has surged 13 percentage points in a week, bringing the state almost level with the national average. The state has also contracted with Blue Shield of California to oversee distribution. But some experts say the state is still recovering from the first critical early weeks.
The state’s early approach to vaccinations was akin to waiting for every first-class passenger to board an airplane before opening boarding to coach class, and not allowing anyone in the last boarding groups to stand in line before it’s their turn, said Dr. David Lubarsky, the chief executive of UC Davis Health.
“What you’d end up with is a plane that never left the airport,” Lubarsky said.
One reason it has taken so long to inoculate healthcare and front-line workers is that many have been reluctant to take the shots. The state, public health officials and critics say, should have better anticipated that hesitation and provided more funding for vaccine education and outreach — or moved on to other groups more quickly.
Though about 84% of workers at Cedars-Sinai Medical Center have been vaccinated, the rate is closer to 65% at Keck Medicine of USC and at UCLA Health, officials said. Only 55% of Los Angeles firefighters have gotten the shot.
“It would be a mistaken assumption to say you don’t need to do education even among healthcare workers,” said California Sen. Richard Pan (D-Sacramento), who has worked to tighten California’s childhood vaccine laws. His hope is that some healthcare workers who resisted the vaccine at first change their minds once their peers create “more of a social norm around it.”
Also hampering the rollout has been a shortage of workers to give vaccines. In Southern California, the surge of COVID-19 cases has left intensive care units at capacity, leaving overwhelmed medical workers with less time to administer doses.
Some vaccination sites are using nursing students. A healthcare tech start-up assisting with L.A.’s mass vaccination sites is urgently hiring more than 150 nurses and medical assistants. And Orange County is actively enlisting volunteers — including acupuncturists and chiropractors — even if their license or certification has expired.
“It’s really an all-hands-on-deck situation,” said Richard Dang, an assistant professor at the USC School of Pharmacy who is overseeing a city vaccination clinic in Lincoln Heights.
Another resource unexpectedly in short supply? Orange cones. David Ortiz, public information officer for the L.A. Fire Department, said there are at least 21,000 cones at Dodger Stadium to route cars through the site and off the street, but that still isn’t enough. His organization has had to rent cones, borrow them from other city departments and accept private donations.
Workers at the sites and in public health departments have also grappled with systemic data collection problems that have prevented officials from observing how many doses are being administered.
Kim Saruwatari, the public health director for Riverside County, said the data problems have slowed down the ability to distribute additional doses to various sites.
“We aren’t able to see how quickly our providers are able to get vaccine out,” Saruwatari said.
The process for getting a COVID-19 vaccine varies county to county.
Some records that should have been submitted to a state clearinghouse were not, which forced local health officials and hospitals to double-check and reenter data multiple times. A coding error involving a major vaccine provider led to some underreporting on the number of doses administered, the extent of which is not yet clear, officials said.
Barbara Ferrer, the head of L.A. County’s public health department, said she had been forced to dispatch “data teams” to “many sites” to independently verify how many vaccine doses had been distributed and how many were still in storage after the state’s system showed a “big discrepancy” between the numbers.
The issue has appeared at hospitals and health clinics, a department spokesman said.
The data problems have complicated the county’s efforts to drill down on which facilities still have unused doses, and if so, why. On Jan. 25, data shared with reporters on the number of vaccines administered were 13 days old and based on weekly surveys of inventory filled out by healthcare providers.
The data problems left health officials unable to determine whether Newsom met his goal of administering 1 million vaccines in 10 days. In L.A., said Dr. Paul Simon, the chief science officer at the Los Angeles County Department of Public Health, the number of doses administered could be as much as 20% higher than what’s been publicly reported.
Health officials have also struggled to keep up with unexpected changes in the state’s vaccine plan, which are not always accompanied by enough details or logistical support to carry them out.
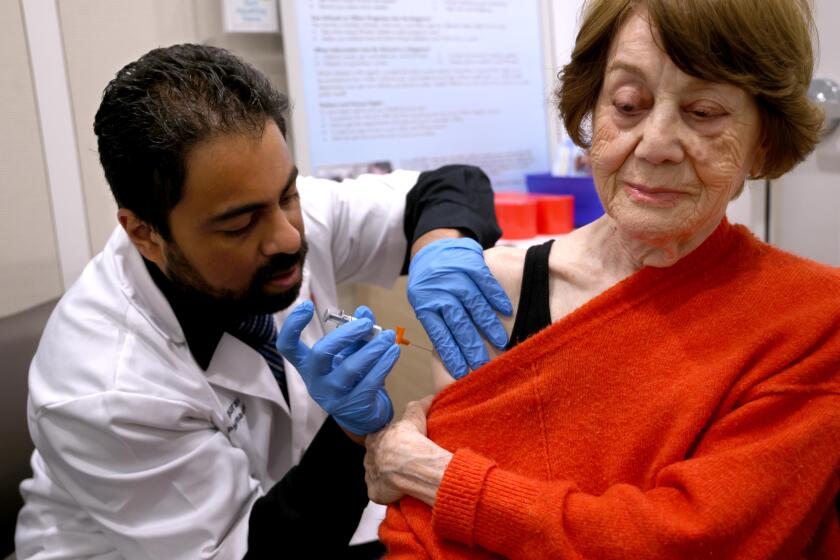
Many seniors were furious after lining up at pharmacies following Newsom’s announcement Jan. 13 that people 65 and older could get the vaccine, only to find out that many counties were not equipped to offer them doses.
Newsom explained the decision, saying the guidelines still should allow for flexibility depending on how many doses each county has available.
Adjusting to the shifting announcements about vaccine eligibility from the governor’s office has been tough, Saruwatari said.
“We’re the ones who are having to message to our community and help them understand why things are changing, and what the rationale or reasoning is for the changes, and I think that sometimes that’s challenging,” she said.
Those issues have been compounded by the state’s decentralized healthcare system, which relies heavily on 61 local health departments in 58 counties. Each agency administers the vaccine locally, and can make decisions that differ from federal or state guidance.
“We’re a big and complicated state, and it’s a famously fragmented healthcare system,” said Anthony Wright, the executive director of Health Access California. That makes it hard to generalize about went wrong with the early rollout, he said, because populous counties could be struggling with different problems.
“There’s a minimal level of state control, and a maximal level of local control,” said Lubarsky, the UC Davis Health executive. “All of a sudden you dump mass vaccination and credential verification and supply chain issues onto a very stressed public health system that’s been underfunded for decades — it’s not the best way to do things.”
Unwieldy county governments also are at a disadvantage in emergencies that demand quick decision-making. Most California counties are governed by an elected board of supervisors, meaning there’s no single executive in charge.
“The weakness of the county governance structure reveals itself when there’s a life-and-death issue like coronavirus,” said Zev Yaroslavsky, a former L.A. County supervisor.
He noted that L.A. County’s population size is similar to North Carolina’s, but someone would be “laughed out of town” if they proposed North Carolina do away with its governor and instead be run by a board.
L.A. County’s enormous size — 10 million people — is a barrier, but not an insurmountable one. Israel, with 9 million habitants, has the highest COVID-19 vaccination rate in the world, with nearly a third of residents given at least one shot. The country has a universal healthcare system and struck a deal with Pfizer for a stable pipeline of doses in exchange for patient data.
“You have to have someone in charge who is the field general who says, ‘We’re marching this way. I’ve taken into account all the evidence,’ Yaroslavsky said. “And everyone marches in lockstep.”
Times staff writers Soumya Karlamangla, Melody Gutierrez, Sean Greene and Vanessa Martínez contributed to this report.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.