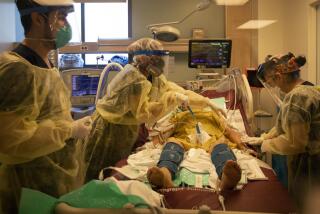
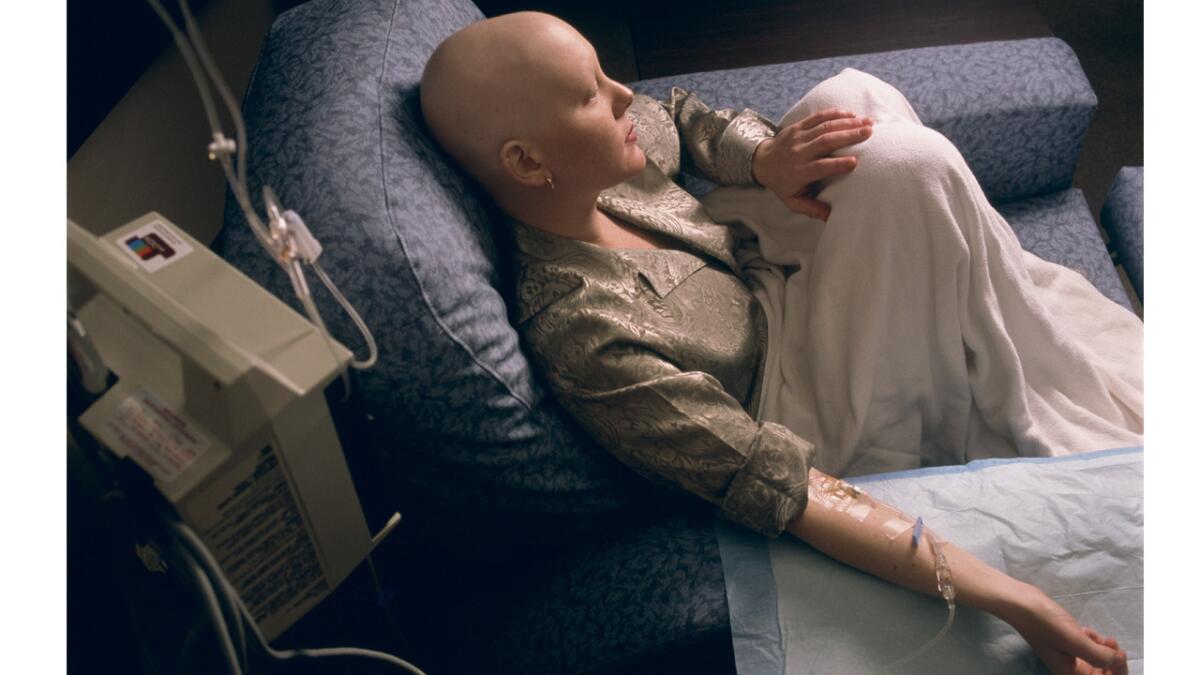
The death rate from cancer is falling for American men, women and children of all backgrounds
- Share via
Cancer is the No. 2 cause of death in the U.S., but a comprehensive new report says that it is affecting — and killing — fewer Americans with every passing year.
The gains have been seen in men, women and children, as well as across racial and ethnic groups. However, depending on the type of cancer involved, some Americans benefited more than others.
There are also some cancers that are becoming more common in the U.S., even as the overall incidence is declining.
These findings are based on cancer registry data from 42 states that account for 89% of the U.S. population. They were published Tuesday in the journal Cancer.
The report was compiled by researchers from the American Cancer Society, the Centers for Disease Control and Prevention, the National Cancer Institute and the North American Assn. of Central Cancer Registries.
Here are some of the highlights:
Cancer is becoming less common
Between 2010 and 2014, 453.8 new cases of cancer were diagnosed for every 100,000 people each year, on average. That incidence declined by an average of 1% per year during that period.
Cancer incidence is higher for men than for women
Doctors diagnosed 502 new cases of cancer per 100,000 men annually between 2010 and 2014, on average. That compares with an average of 420.6 new cases per 100,000 women each year during the same period.
But men saw their cancer incidence fall …
Between 1999 and 2008, the incidence of new cancers in men dropped by an average of 0.6% per year. It then fell by an average of 2.2% per year through 2014.
… while women did not
Cancer incidence remained stable for women over the entire 15-year period, according to the report.
Fewer Americans are dying of cancer
In the years 2010 to 2015, there were 163.5 cancer-related deaths for every 100,000 adults in the U.S. That mortality rate fell by an average of 1.5% per year during the period.
This was true for both men and women
The mortality rate for men declined by an average of 1.8% per year between 2010 and 2015. For women, it fell by an average of 1.4%.
Cancer mortality rates were higher for men than for women
Between 2010 and 2015, 196.7 out of every 100,000 men died of cancer each year, along with 139.5 out of every 100,000 women, on average.
The incidence of some types of cancers declined …
Men experienced lower rates of seven of their 17 most common types of cancer. These included cancers of the prostate (which declined by an average of 7.6% per year), lung and bronchus (2.4%), larynx (2.3%), colon and rectum (1.9%), esophagus (1.6%), bladder (0.8%) and brain and nervous system (0.2%).
Women experienced reductions in seven of their 18 most common cancers. These included cancers of the colon and rectum (which fell by an average of 1.7% per year), ovaries (1.6%), lung and bronchus (1.2%), cervix (1%), bladder (0.8%), brain and nervous system (0.7%) and non-Hodgkin’s lymphoma (0.4%).
… while it increased for others
Men saw higher rates of eight common cancers, including those of the liver (which increased by 2.8% per year, on average), myeloma (2.5%), thyroid (2.4%), melanoma of the skin (2.3%), leukemia (1.6%), oral cavity and pharynx (1.3%), kidney (1.1%) and pancreas (1%).
Women experienced higher rates of cancer at 10 of their most common sites, including the liver (with a 3.8% average annual increase), thyroid (1.9%), myeloma (1.6%), leukemia (1.4%), uterus (1.2%), melanoma of the skin (1.2%), pancreas (1.1%), oral cavity and pharynx (0.8%), breast (0.4%) and kidney (0.4%).
The obesity epidemic helped fuel the increase in some of these cancers, including those of the breast, kidney, endometrium and pancreas, the study authors noted.
Some kinds of cancer became more deadly …
Between 2011 and 2016, mortality rates increased for seven of the 18 most common types of cancer in men. These included non-melanoma cancers of the skin (whose mortality rate rose by an average of 2.8% per year), liver cancer (1.6%), cancers of the oral cavity and pharynx (1%), soft tissue cancers (0.8%), brain and nervous system cancers (0.5%), and pancreatic cancer (0.2%).
For women, mortality rates rose for cancers of the liver (with a 2.7% average annual increase), uterus (1.9%), brain and nervous system (0.5%) and pancreas (0.2%).
… and others became less so
Death rates dropped for 11 common cancers in men. These included cancers of the lung (the mortality rate dropped by an average of 3.8% per year), melanoma of the skin (3%), larynx (2.5%), colon and rectum (2.5%), prostate (2.2%), leukemia (2.2%), non-Hodgkin’s lymphoma (2%), stomach (1.6%), esophagus (1.1%), myeloma (0.9%) and kidney (0.5%).
Women saw mortality rates decline for 14 types of cancer, including those of the colon and rectum (a 2.7% average annual decline), non-Hodgkin’s lymphoma (2.7%), melanoma of the skin (2.6%), lung (2.4%), ovary (2.3%), leukemia (2.3%), stomach (1.8%), breast (1.6%), esophagus (1.6%), kidney (1.4%), oral cavity and pharynx (1.3%), gallbladder (1.3%), cervix (0.7%) and bladder (0.5%).
The role of cigarettes
More than 1 in 4 cancer deaths in the United States can be traced to cigarette smoking, the study authors wrote. This is despite the fact that smoking rates have fallen by half since 1964.
Racial and ethnic disparities in cancer incidence
Black men were diagnosed with 558.2 cancers per 100,000 people between 2010 and 2014. That was the highest incidence of any group of men, according to the study. For the sake of comparison, there were 500.1 cancer cases per 100,000 white men, 446.8 per 100,000 American Indians and Alaska Native men, and 309 per 100,000 men who were Asians and Pacific Islanders.
Among women, cancer incidence was highest among whites, with 428.7 cases per 100,000. They were followed by American Indians and Alaska Natives (409.9 cases per 100,000), black women (406.8 per 100,000) and Asians and Pacific Islanders (295.8 per 100,000).
For both men and women, cancer incidence was lower for Latinos than for people classified as “non-Hispanic.”
Cancers of the prostate, breast and lung were largely responsible for the differences in cancer incidence among demographic groups, the authors wrote.
Disparities in cancer deaths
Between the years 2011 and 2015, black men experienced a higher rate of cancer-related deaths (239.9 per 100,000) than white men (196.4 per 100,000), American Indian and Native Alaskan men (181.4 per 100,000) and Asian and Pacific Islander men (120.4 per 100,000).
The pattern was the same for women. Between 2011 and 2015, the cancer mortality rate was 159 per 100,000 black women, 140 per 100,000 white women, 127.6 per 100,000 American Indian and Native Alaskan women, and 87.7 per 100,000 Asian and Pacific Islander women.
Adults deemed non-Hispanic had higher cancer mortality rates than their Latino counterparts. The differences were 201.4 versus 140 deaths per 100,000 men, and 143.4 versus 96.7 deaths per 100,000 women.
A mixed picture for children
Between 2010 and 2014, American children became more likely to be diagnosed with cancer — but they were less likely to die as a result.
For every 100,000 children ages 14 and under, 16.6 were diagnosed with cancer each year and 2.1 died of it, on average. The overall incidence of childhood cancers increased by an average of 0.8% each year, while the mortality rate fell by an average of 1.5% per year.
Cancer mortality rates for children were similar across all racial and ethnic groups. On the low side, there were 1.7 deaths per 100,000 Asian and Pacific Islander children; on the high side, there were 2.2 deaths per 100,000 black children.
Disparities were more pronounced for cancer incidence, with a low of 12.6 new cases per 100,000 American Indians and Native Alaskan children to a high of 17.3 new cases per 100,000 white children.
Follow me on Twitter @LATkarenkaplan and “like” Los Angeles Times Science & Health on Facebook.
MORE IN SCIENCE
Yes, President Trump, there is a difference between HIV and HPV. Here’s a handy tipsheet
The U.S. birthrate hits another record low. Even women in their 30s are having fewer babies
To prevent recurrent strokes, should aspirin have a wingman? Maybe not