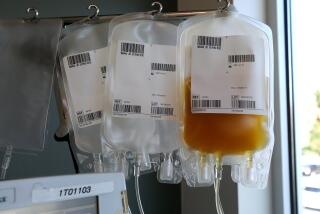
Complete Change of Blood Is a Lifesaver for Some
- Share via
Hippocrates would be proud to see how modern medical magicians have adopted concepts basic to ancient Greek medicine.
Centuries ago, doctors believed diseases were cured by restoring balance in the body’s four fluids, or “humors”: blood, phlegm, yellow bile and black bile.
Blood-letting was one way to do that.
But instead of leech and knife, physicians today have harnessed blood-banking technology for removing blood from the sick. They have added another dimension to this treatment: They can replace what has been removed with new, healthy blood.
Called plasmapheresis, the procedure is lifesaving for some people, said Dr. Harvey Klein, chief of transfusion medicine at the National Institutes of Health clinical center in Bethesda, Md.
Circulated Into Machine
In less than two hours, blood is circulated out of the body into a machine that separates blood’s two components. The cellular component--red and white blood cells--are returned to the body, while plasma--the liquid component containing proteins and antibodies--is not. Either frozen plasma or a salt-protein solution is substituted for the patient’s own plasma.
Although the procedure sounds drastic, patients rarely feel drained of their blood. “They feel good after the exchange,” said Dr. Peter Dau, associate professor of neurology at Northwestern University School of Medicine in Evanston, Ill. “They literally do not know the exchange is going on.”
By removing the plasma, whatever “poisons” that are in it also are removed. Those toxic chemicals may be substances called autoantibodies that attack the body’s own tissues, or potentially harmful byproducts of the body’s chemical processes that through some genetic mishap are not disposed of.
Caused by Disease
Some people have a disease that produces abnormal proteins that make the blood too thick. The slowed flow can cause strokes, but by removing plasma and reinfusing fresh fluid, blood is thinned and strokes are prevented, Klein said.
How frequently and how much plasma must be removed varies.
“If we know what we’re dealing with, we can measure the blood protein level and determine how rapidly it is being made and destroyed. Then we can make rational decisions about when it’s (plasmapheresis) is needed,” Klein said.
Because in many cases physicians don’t really know what the disease agent in the blood is, or how often it needs to be removed, substantiating the value of plasma exchange has been been difficult. The procedure is expensive, and it is often done along with other treatments, such as medication, or as a last resort after all else has failed, Dau said. And there can be side effects.
Reaction From Body
“You can provoke a worsening of the condition with plasma exchange,” he said. The body reacts to the abrupt decrease in the concentration of chemicals in the blood by increasing production of those substances. “In some cases it actually stimulates production, so the level actually goes higher than it was before.”
Each session costs about $1,000, and often sessions must be continued semiweekly for life, like kidney dialysis.
In 1981, Medicare capped the use of plasma exchange by saying that only in four diseases was filtering out either the cellular or the plasma portion of blood proven effective and therefore worth reimbursing.
That list has grown to 10, Dau said, but that is 10 out almost 150 disorders in which there has been some indication that these techniques might help.
For a few diseases, plasmapheresis has cut the death rate from 90% to 10%.
Paralysis Treatment
Recently, controlled studies in patients with Guillain-Barre syndrome, a temporary, albeit serious, paralysis that sometimes requires the patient be kept alive on a respirator, have demonstrated that plasma exchange speeded up recovery by about 50%, Dau said.
But some disorders are so rare and so variable that there aren’t enough people with them to adequately evaluate the procedure’s effectiveness.
For other disorders, such as schizophrenia and amyotrophic lateral sclerosis (ALS), a fatal, degenerative nerve-muscle disease, such evaluations have not panned out despite early indications that plasmapheresis helped.
“With ALS, there have been six published studies and many more unpublished, and none of them shown even a glimmer of hope,” Dau said.
Studies assessing the technique’s value for multiple sclerosis are continuing.
Although Dau said he recognized the need for the federal government and insurance companies to be cautious about supporting such an expensive procedure, he said the strict payment policy could be costing lives.
“If it looks like a promising application, why not let the door be open for a while and let a consensus develop among physicians,” he suggested. “Some of these diseases are too rare to be studied any other way.”