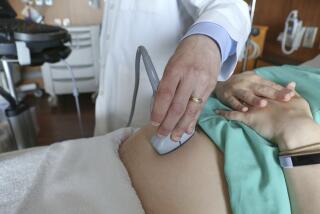
Doctor Working to Ease Infants’ Pain : Medicine: O.C. specialist joins the fight against profession’s traditional reluctance to order drugs for suffering babies.
- Share via
LAGUNA HILLS — As a pediatric resident seven years ago, Dr. Perry Eisner had what would seem simple goals: to stick up for his tiny patients and, as much as possible, protect them from pain.
Turned out not to be so simple.
Eisner recalls being paged in the middle of the night to the bedsides of wailing infants fresh from major surgery. The parents would plead with him frantically: “Can’t you do something for our baby?” But overworked surgical residents, who controlled the infants’ cases, routinely would veto his orders for medication to ease their suffering. “Either they would claim it’s not painful or they would say, ‘It doesn’t hurt in kids like it does in adults,’ ” said Eisner, 34, grimacing at the once-prevalent notion. “I couldn’t stand it. It was awful.”
So awful that Eisner later decided to make pediatric pain relief his life’s work. After completing a fellowship in pediatric anesthesia and critical care three years ago, the young doctor joined a growing contingent of physicians and nurses who attack pain with the vigor their colleagues apply to life-threatening scourges.
Using numbing drugs infused through a catheter, Eisner can block the nerve impulses of his little patients to the point that they feel next to nothing in the days following surgery. The technique, long used in adults but uncommon in children, is just one way of practicing what academics, nurses and some parents have preached for some time: Babies recover best when they don’t hurt.
“The big change has come in the past five or 10 years,” said Dr. Feizal Waffarn, professor of pediatrics at UCI Medical Center in Orange and attending neonatologist. “There is better training, I think, education, and some very nice studies done to show that infants indeed sense pain, feel pain no different than adults.”
But in many hospitals and clinics, the old ways die hard. Five years ago, Eisner had to search high and low for a physician who would use a local anesthetic during circumcision of his newborn son. Now, he describes unmedicated circumcisions as a pet peeve, saying no one but a helpless infant would submit to such an excruciating procedure.
“When you ask why (doctors are stingy with pain medication to youngsters), they say, ‘Well, I’ve done it that way for years,” said Eisner, who is on the staff of Saddleback Memorial Medical Center and Saddleback Valley Outpatient Surgery Center in Laguna Hills.
“Well, that’s not really a good answer. The fact that you can do something without someone dying doesn’t mean it’s a good thing to do.”
Historically, children have received poor “pain management” across the United States, said Dr. Lonnie Zeltzer, who heads the Pediatric Pain Program at UCLA, one of just a few such centers in the country.
“A lot of it has to do with the fear that drugs would be too toxic, and with not knowing how to measure pain” in the very young, who, after all, cannot speak for themselves, she said.
The situation arises most commonly when physicians are treating newborns under 2 months old and premature infants, said Dr. M. Douglas Cunningham, medical director for newborn medicine at Long Beach Memorial Medical Center, who practiced for many years at UCI Medical Center and Saddleback.
The result: Even major surgery, such as spreading the ribs to tie off a blood vessel near the heart in premature infants, has been performed with little or no anesthetic. Not to mention minor procedures such as placing chest tubes or drawing bone marrow.
It has been only seven years since the American Academy of Pediatrics announced that it was unethical to perform surgery on premature infants without an anesthetic.
Doctors’ aversion to pain medications--particularly narcotics--was not a matter of callousness or cruelty, Cunningham said. “A very large part of it was the fear of addiction. . . . That coupled with the fact that infants don’t tolerate meds well (and) a concern about overdosing.
“That’s where Dr. Eisner’s group has really led the way: precise dosage, careful monitoring, focusing on the period when pain is real” and discontinuing medication when it stops, Cunningham said.
Surgeons whom Eisner works with also appreciate his use of local anesthetics because it minimizes the need for narcotics.
“We do a lot of procedures on the genitalia, testicular surgery,” said Dr. Igal Silber, who specializes in pediatric urology. “This is the ideal type of anesthesia. If you just give injections of morphine, Demerol, (infants) still tend to thrash about a lot” in recovery.
The use of local anesthetics has become increasingly common, especially among more recently trained anesthesiologists.
A key development paving the way for longer-term treatment of infants’ pain was the introduction of longer-lasting local anesthetics and the development of preemptive analgesia--pain medication given before an operation to reduce pain afterward, said Dr. David Steward, director of anesthesiology at Childrens Hospital Los Angeles.
“It stops the noxious stimuli from ever getting . . . to the spinal cord or brain,” he said, even after the surgical gas wears off.
Other research has led the once-standard notions to crumble: that children do not feel pain as acutely as adults, that they don’t remember what they do feel, and that they are so resilient that any unpleasant experience is of no long-term significance.
“Some studies have been done over the past five or six years showing that when you don’t use anesthesia, not only is it ethically a bad thing to do, there are real medical consequences,” Eisner said.
One such study, published in the New England Journal of Medicine in 1992, found that newborns lightly anesthetized during cardiac surgery fared much worse than those who were heavily anesthetized.
According to the study, by K.J.S. Anand and his team, the babies who received less anesthesia experienced a much greater stress response--such as higher levels of the hormones epinephrine and cortisol--and had a significantly higher post-operative death rate.
In the same issue that carried this research, the Journal issued a challenge to its audience, seemingly wondering why clinicians have been so slow to act on the latest science.
“It seems that we are better able to tolerate an infant’s pain than to deal with our own discomfort and insecurity about the correct dose of pain medication to give the infant,” the Journal concluded in the introspective editorial.
“Now that the benefit of pain relief has been so clearly demonstrated, it is our responsibility to treat pain in neonates and infants as effectively as we do in other patients.”
Studies on rats suggest that if babies experience significant pain, it disturbs the growth and development of the nervous system and can make them more susceptible to pain as adults, UCLA’S Zeltzer said.
The overall objective, Eisner said, is to make the hospital or clinic visit “completely non-stressful.” That means not only using the best medications in the best dosage, but treating the child and parents with sensitivity.
For example, he said, it is not a good idea to separate a child from his parents and hold him down--probably kicking and screaming--to place an anesthesia mask over his face. He remembers with chagrin his rotations at Childrens Hospital Los Angeles, when terrified youngsters would ask him, “You’re not going to use the mask, are you?”
Better to give a child a mild sedative and sometimes even allow his parents to hold and rock him. Then apply the mask.
“Ninety-nine percent of the time, they don’t cry at all,” he said.
Eisner can’t ask his infant patients whether they appreciate his approach, but he said they have their ways of letting it be known when they don’t: Grimaces, fixed stares and a high-pitched wail, for example.
Parents are grateful when they don’t have to hear that.
“It’s blood-curdling,” said Tracy Garrison of Irvine, who has learned to discern her 5-week-old son Joshua’s I’m-in-pain shrieks from the I’m-hungry and I’m-wet varieties.
But the boy emitted nary a whimper after testicular surgery last week for which Eisner numbed his lower body.
“He’s as happy as he could be,” the baby’s father, Mac, said as the child tugged on a bottle only an hour after the outpatient operation.
To prevent post-operative pain involving long-term recovery, Eisner often performs what is known as an epidural. He injects local anesthetic through a catheter placed in children’s lower backs, which is fed into the epidural space surrounding the spinal cord. A local anesthetic, Marcaine or lidocaine, and a low concentration of narcotics are infused to numb nerves leading to the incision. During the days after leg, chest or abdominal surgery, youngsters often don’t feel a thing, he said.
Although the procedure has been used for years on adults, he said, physicians are often loath to risk it on young children because of its limited track record. Eisner estimated that 10% of anesthesiologists use the technique on youngsters.
Experts like Steward of Childrens Hospital Los Angeles stress that the technique is only one means of pain control and cannot be used for all types of surgery. Also, it requires training and expertise, and the patients must be closely watched.
Finally, to many doctors who treat children, the procedure has yet to prove itself.
“There’s always been a caution in applying things in new age groups, particularly when what you’re doing is complicated,” Steward said. “You’re dealing with smaller needles, a smaller catheter, a different anatomy in the epidural space. . . .”
“We haven’t decided what the place of epidural anesthesia is in the neonate. People are waiting to see what the safety record is.”
Eisner said he has never had a complication and expects use of epidurals in young children to become routine--that is, as long as health insurance companies will pay for it.
“I think with kids it’s going to be equally as safe as with adults, if not more so,” he said.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.