BODY WATCH : Labor Saving
- Share via
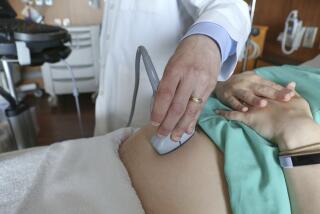
There is something about the sight of a pregnant woman that inspires complete strangers to recount labor and delivery horror stories. These bloodcurdling tales, however, are rarely a harbinger of things to come. Women today have a variety of safe, effective alternatives to pain during childbirth.
Although not all women will want or need pain relief, for those who do, anesthesia can turn a difficult experience into a positive event--one in which they feel alert and involved.
Over the years, pain-relief methods have become increasingly sophisticated, so it’s a good idea to talk with your obstetrician beforehand to make an informed decision. Here is a guide to what’s out there.
INTRAVENOUS MEDICATION
What it is: A narcotic--usually Demerol--is used to relieve, but not eliminate, pain. Demerol has fe When it is given: Usually in early labor. Babies are most affected if Demerol is given three to four hours before delivery. IV medication is avoided when labor is progressing rapidly.
How it is given: Through an IV or by injection. Obstetricians usually give it or oversee its administration by a labor nurse.
Pros: Pain is somewhat diminished, letting you conserve energy for the second stage of labor.
Cons: You are confined to bed because if you try to sit up or walk, your blood pressure may drop. You may experience nausea or vomiting and feel groggy, sleepy or disoriented. May slow labor if given too early. Often depresses the baby’s respiratory system. Although this is transitory, the newborn may require special attention after birth.
EPIDURAL
What it is: For labor or during a Cesarean. Usually composed of a local anesthetic or a combination of local anesthetic and high-potency, short-acting narcotic.
When it is given: In general, after a woman has dilated three to four centimeters.
How it is given: The doctor numbs the skin on your back. You curl up or bend over from a sitting position and a needle is inserted between the vertebrae of the lower back into the space surrounding the spinal-fluid sac. Anesthetic is injected via a catheter, which remains to convey medication as needed.
Pros: Can often eliminate labor pain completely while letting you push during the second stage of labor. Does not alter or blunt consciousness. Minimal health risks for the mother and baby.
Cons: Keeping still during insertion of the needle can be uncomfortable during a contraction. You are confined to bed because the local anesthetic may lower blood pressure if you stand. Pushing may be less effective if you can’t feel the contractions, but this can be controlled by receiving less medication while you push. In rare cases, an epidural may cause a spinal headache.
SPINAL
What it is: For labor or a Cesarean. A small amount of narcotic is used for labor; a local or a combination local and narcotic is used for a Cesarean.
When it is given: During a vaginal delivery when birth is expected within a few hours, or when a Cesarean becomes necessary.
How it is given: Same as for an epidural except the needle is inserted through the spinal-fluid sac. Small quantities of medication are injected into the cerebrospinal fluid. The needle is then withdrawn.
Pros: Greatly eliminates pain while letting you remain awake and alert. Minimal health risks for the mother and baby. If the spinal is used for labor, you may be able to walk after it has been administered.
Cons: Keeping still during insertion can be difficult. When used for labor, may provide pain relief for only two to three hours. In rare cases, leakage of cerebrospinal fluid may cause a spinal headache. Although it can be severe, this type of headache is treated with a blood patch (an epidural injection using your own blood), or oral or IV fluids, analgesics and bed rest.
COMBINED SPINAL-EPIDURAL
What it is: Regional anesthesia that combines the advantages of the spinal and the epidural. A recent development, it is not available at all hospitals.
When it is given: In general, after a woman has dilated three to four centimeters.
How it is given: Aspects of the epidural and spinal procedures are combined. A narcotic is injected into the cerebrospinal fluid, the spinal needle is removed, and a catheter is inserted into the epidural space to provide more medication as needed.
Pros: Eliminates or greatly diminishes pain while not altering consciousness. Minimal risks for the mother and baby. You may be able to stand or walk for two to three hours.
Cons: If the epidural option is needed, you will have to remain in bed because the local anesthetic may cause low blood pressure if you sit or stand. Spinal headache, though rare, is possible.
PUDENDAL BLOCK
What it is: A local anesthetic injected into the vaginal wall.
When it is given: Just prior to delivery if an episiotomy is necessary, or after delivery to repair vaginal tears.
How it is given: An injection done by the obstetrician.
Pros: Provides lack of sensation during a minor surgical procedure.
Cons: Some discomfort during the injection.