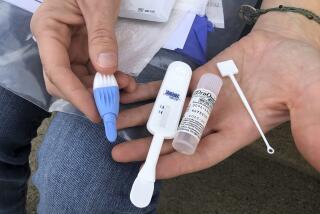
Soldiers of Misfortune : On the Trail of Carriers of Sexually Transmitted Diseases, Public Health Workers Battle Not Only Mistrust and the Clock but Shrinking Funds
- Share via
Cruising slowly in their ramshackle van, the disease detectives prowl the back streets of Los Angeles in search of a contagious hit-and-run artist.
He lived in a makeshift camper. That’s all Dave Sullivan and Vanessa Newton-Pulley have to go on. Their tipster, now cooling her heels in the County Jail on some unrelated charge, had bedded down with him shortly before testing positive for syphilis.
One by one, she had rattled off the names of her lovers. But all she recalled of the tryst at 45th Street and Ascot Avenue in South-Central was her companion’s first name and a vague description of his rig. Within 90 days--the incubation time for syphilis--the man would be infectious, if he wasn’t already. And as he took on new lovers, the daunting task facing the two public health workers would multiply yet again.
And yet half an hour into their search, the two suddenly decide to drop the hunt cold. Already overwhelmed by a mounting caseload, there’s simply no more time to canvass the neighborhood for anyone who might have seen the man.
“Sometimes,” Newton-Pulley says, “you feel like there’s no way to break the chain.”
She has good cause to be frustrated. As venereal disease rates increase nationwide, the number of government health workers is dwindling, a trend experts warn could further jeopardize public safety. The reductions are part of Republican efforts to shift financial responsibility for costly health and welfare programs to state and local agencies.
Newton-Pulley and Sullivan belong to the Los Angeles County Health Department’s sexually transmitted disease program, whose force has been reduced by a third--from 38 to 25--in the past three years. Paid by the national Centers for Disease Control and Prevention, their numbers have been slashed with federal budget cuts.
Health officials say the savings come at the expense of a critical mission. The disease intervention specialists--also known as partner notifiers or DIS workers--locate and sometimes treat people who have been exposed to one of a number of venereal diseases spreading across the country like some sexual chain letter. In the face of such grim work, local DIS workers call themselves the DIS Squad.
Former U.S. Surgeon General Joycelyn Elders says the cutbacks reflect a shortsighted government policy that will come back to haunt the American public. “The reason many of these venereal diseases are still around is that we cut programs before we get rid of the problem. And do you know what happens? The diseases come back with a vengeance.”
Local DIS workers handle thousands of cases each year involving people who lost their gamble with unsafe sex. Day after day, they track a wide range of suspects, all of them clues to an often-baffling conjugal riddle.
The job requires them to be equal parts cop and counselor, nurse and priest. For pay ranging from $25,000 to $35,000, DIS workers frequently draw blood on the street, in living rooms and public restrooms from the sex partners of infected people too busy or too timid to report to a nearby hospital.
With a knock on a door or during an interview at one of dozens of public health clinics across Los Angeles, they face perhaps their most difficult task of all: Doing the follow-up to blood tests. Telling people they have contracted HIV.
“It can be sad, stressful work,” says Newton-Pulley who, like other DIS workers, received two years of on-the-job training. “Every day, we talk to people about intimate aspects of their lives that often they have shared with no one else: How they have sex and who they have it with. That kind of talk reaches the very depths of someone’s intimacy.”
But because of a two-year CDC hiring freeze, there are significantly fewer DIS workers to do the job nationwide. CDC officials acknowledge that they have thinned the ranks of the street soldiers tracking venereal disease--shifting the responsibility to local agencies.
“Community-based organizations need to step forward to become the advocates of behavioral change,” says William Parra, acting deputy director of the National Center for Prevention Services in Atlanta, a branch of the CDC. “They’re the ones who have the best access to the people who are at risk, not us.”
But with Los Angeles County in the throes of financial crisis, there simply aren’t enough local dollars to replace the DIS workers. The county is also cutting by 30% its own staff of about 50 public health workers, who do much the same work as DIS workers in neighborhoods throughout Los Angeles. Educational and health screening programs are also being scaled back or eliminated.
Still, the disease cases keep coming. Today, one in five adult Americans carries some type of incurable viral infection such as herpes. When the curable, bacterial STDs such as syphilis and gonorrhea are included, Americans have at least a one-in-four lifetime chance of contracting an STD, CDC studies show.
And syphilis and gonorrhea are again seeing modest rises in Los Angeles after reaching near-epidemic levels in the mid-1980s. As well, new cases of chlamydia and human papillomavirus are at their highest nationwide levels ever in people 15 to 25.
Says Gary Richwald, director of the county’s STD program: “Los Angeles County has sexually transmitted disease rates that are two to five times the national average--and in some parts of this town 20 times the national average--and yet we do not have the local resources to pick up where the federal government is leaving off to battle this public health problem.”
And so, like gumshoes, the DIS Squad hits the streets, frequenting topless bars, fast-food kitchens, crack houses and gyms, looking to interview bankers, drug dealers, sewer workers.
People often react the same way when facing the news of a venereal disease: Shoot the messenger. Sometimes literally. DIS workers have been met with loaded rifles and baseball bats. They’ve had clients call cops and lawyers.
No matter how they try to gently convince people that this inquiry into their sex lives is for their own good--and that of future lovers--DIS workers say doors still slam in their face.
Says Richwald: “People have an image of the government standing on a street corner below their window, megaphone in hand, saying, ‘We know you’re up there, Shirley Brown in Apartment 5C. We know who you slept with. We have a van down here. Now either you come down or we’ll come up and get you because you’re gonna be locked up.’ ”
*
Irma Ramos recalls one shift in which she told four people they had HIV.
At 24, she looks like she could still be crossing a college campus, not dispensing such ravaging news.
“That day I got home, I just went into a shell,” recalls the two-year DIS worker. “I took a long walk on the beach. Four people had just learned their lives had changed forever. They had received their death sentence. And I was the one who told them.”
In part because of their dwindling numbers, the partner notifiers concentrate their efforts in six geographic core areas identified as the county’s highest in syphilis infection rates during a 1987 government study.
The districts--which include Compton and Inglewood as well as the south, southeast, southwest and central areas of Los Angeles--are mostly poor neighborhoods where residents often have more pressing issues than dealing with an STD.
“People say, ‘So, I’ve got syphilis? Big deal! I don’t have a job and I don’t have any money to buy food for my kids,’ ” says Sullivan, a district coordinator. “They say they’ll come to the clinic when they’re good and ready.”
For such events, workers carry needles and drugs to treat some diseases on the spot. When they draw blood for tests, they call it bleeding a patient. They also must deal with parents incensed over the legal right of their children to talk directly to DIS workers.
State law allows minors 12 and older to receive information on their sexual health and infected partners without parental consent. But the result is often ugly face-offs between partner notifiers and irked moms and dads.
Such confrontations, DIS workers say, have increased largely because more teen-agers are contracting venereal diseases. National health statistics show one in four sexually active teens will become infected with an STD by 19.
To fight the trend, DIS workers have developed an arsenal of tactics, including access to social service and Department of Motor Vehicle records and cross-directories. Most times, they rely on word of mouth.
They locate partners through jail dockets and homeless shelter lists. At apartment buildings, they befriend children who open gates and direct them to apartments.
Like cops, they develop sources, offering condoms to hookers and cigarettes to the homeless for information.
They take frightened syphilis patients on tours where--hidden from sight--they point out addresses of their lovers. For parents refusing to reveal names of sexual contacts, DIS workers shoot for the heart: They show pictures of infants who contracted syphilis in the womb.
The job fulfills and--often--frustrates them. It also shocks them: Moments after learning he had tested positive for a sexually transmitted disease, one man asked DIS worker Danielle Banks for a date.
“I told him, ‘You’re in here for an STD and you want to know what I’m doing this weekend?’ ” she recalls. “Well, the answer is, ‘Nothing with you, mister!’ ”
*
Louise was in her rocking chair when the caller came.
Fighting cervical cancer, the 44-year-old South-Central woman had suffered repeated tests and operations in recent months. She could not bear any more bad news.
But DIS worker Doris Simpson was there anyway: Louise had contracted HIV.
That morning, Louise sat on the hardwood floor of her sister’s home and cried--about the disease and about how her family, especially her nieces and nephews, would react.
Then Simpson gave the only good word she could offer: No one had to know about her condition. The choice was hers.
“I hugged her and I said, ‘Oh, thank you!’ ” Louise recalls. “Because I know people with this disease. I’ve seen how no one wanted to go near them, how they didn’t want them near their food. Or their children. They don’t want you to even breathe around them. They treat you like you’ve got leprosy, like you’re one big germ.”
Rather than merely solicit names of past lovers, Simpson met with Louise for three months after breaking the news, helping her through the maze of medical assistance for HIV patients.
County health officials say Louise is benefiting from a more compassionate approach to HIV patients that could eventually become a model for health departments nationwide.
DIS workers also contend with a social stigma concerning their work, especially in the gay community--which tends to remain suspicious of the public health worker programs. Gay activists are critical of any government record-keeping of a disease they say is tantamount to a social scarlet letter.
“Look at what infected gay people face,” says Mark Senak, planning director for AIDS Project Los Angeles. “The church and the military reject you. The idea of trusting my name if I’m HIV-positive or the names of people I’ve been with, it’s just not something the gay culture is inclined to do.”
But county health officials say their program is winning friends in the gay community. “DIS workers are becoming like caseworkers, finding ways to assist patients in their treatment and evaluation, and at the same time getting them information about making lifestyle changes, using condoms, being safer about sex,” says one county AIDS counselor.
Says health official Richwald: “We’re being pegged as some sort of medical IRS. And that’s simply not true.”
*
Sometimes, district coordinator Sullivan imagines STDs as this vast polluted river that has broken the dam, flooding the streets, washing away its victims. And he fears there’s no way to stop the water.
With his ponytail and trimmed goatee, he sits in his battered van with the Grateful Dead stickers as partner Newton-Pulley canvasses a nearby block.
The pair have abandoned their search for the camper man, moving on to another syphilis case. As usual, information is scarce: All they know is that he lives in a brown and yellow house somewhere in Watts.
The son of a former venereal disease investigator and public health nurse, Sullivan worked in a psychiatric hospital before following in his father’s footsteps.
Sometimes he regrets the decision, having watched co-workers quit, uncomfortable with the places they go, the people they talk to. “People get burned out,” he says.
The doubts don’t last long--there’s too much work to do.
Newton-Pulley returns to the van. No luck. All they have is a worthless first name of another would-be possible carrier, a case that will go back into the working file. DIS workers call them “unks,” short for unknown.
Sullivan sighs, starts up the van.
“There’s a little saying among DIS workers,” he says. “The unk family is the most infected family in America.”
More to Read
The biggest entertainment stories
Get our big stories about Hollywood, film, television, music, arts, culture and more right in your inbox as soon as they publish.
You may occasionally receive promotional content from the Los Angeles Times.