High Levels of Virus Tied to Quicker Onset of AIDS
- Share via
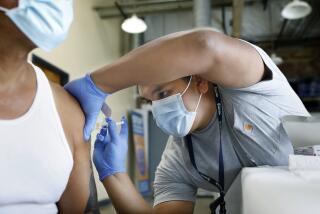
WASHINGTON — Scientists reported Tuesday that infected persons with high levels of human immunodeficiency virus develop AIDS much more rapidly than those with lower amounts of the virus, a finding that likely will affect how individual treatment decisions are made.
Addressing the Third Conference on Retroviruses and Opportunistic Infections, researchers said that measuring viral load is a much more accurate predictor of disease progression than the current method of counting CD4 cells, the key immune system cells that are the primary target of the virus.
“Our findings . . . can predict disease progression as far as 10 years into the future,” said Dr. John W. Mellors, the study’s lead investigator. “You can actually define the individual risk of AIDS before it occurs. This gives us a real handle as to where the individual patient is.”
The levels of virus should “absolutely” have “more weight” in assessing a patient’s prognosis than gauging the strength of the immune system through CD4 levels, Mellors said.
“You can actually see a doubling of [viral] levels at least two years before you see a 100-cell decline in CD4 levels,” he said. It is viral reproduction that ultimately depletes CD4 cells, leading to the destruction of the immune system.
In the largest study of its kind, researchers at the University of Pittsburgh Medical Center used a new test developed by Chiron Diagnostics to analyze blood plasma samples collected every six months from 181 HIV-positive individuals over a 10-year period.
They determined that the risk of developing AIDS symptoms after seven years was less than 10% among those with the lowest levels of virus. On the other hand, 60% of those with the highest viral load progressed to AIDS.
Viral load measurement also proved to be an accurate predictor of survival. In subjects whose levels were the lowest, none died within five years of the measurement, compared to 65% of those with the greatest levels.
“The survival data were just as powerful” as the progression findings, Mellors said.
While many experts believe that early drug therapy ultimately will be the most effective strategy against AIDS, they also stress that treatment should be tailored to each patient.
Using an analogy to cancer, Mellors urged clinicians to “stage” AIDS by measuring viral load, rather than CD4 counts, to determine how quickly a patient is likely to develop AIDS. “No oncologist in his right mind would treat cancer without staging it,” said Mellors, an associate professor of medicine and director of the Pitt Treatment Evaluation Unit.
Mellors and his colleagues studied 181 infected gay or bisexual men who enrolled in the study between April 1984 and March 1985 and measured the levels of viral RNA (ribonucleic acid, the virus’ genetic material) in their blood. They used a Chiron test called branched DNA assay. The test has not yet been licensed by the Food and Drug Administration, although it is available through clinicians for research.
After measuring the RNA, the men were divided into four groups: low (meaning those with fewer than 5,000 copies of viral RNA per cubic milliliter of blood); moderate (between 5,000 and 13,000); moderate-high (between 13,000 and 35,000), and high (above 35,000).
The median time to develop AIDS was eight years for the low group; 6 1/2 years for the moderate group; 4 1/2 years for the moderate-high group, and 2 1/2 years for the high group, Mellors said.
All of the individuals were at various points in time after infection; that is, few, if any, knew exactly when they had become infected.
This made the RNA measurements “very much predictive of the consequences of HIV infection in the real world,” Mellors said, meaning that physicians could be comfortable using the technique in their practices.
Mellors said that scientists still do not know why the virus is produced in such different quantities in different patients. The levels are the result of “the relative balance between virus and host [the patient],” Mellors said.
This could involve numerous factors, among them, the type of viral strain, the immunogenetic characteristics unique to the particular patient and environmental influences, all of which can affect the production of virus, he said.
“That balance is very critical,” Mellors said.