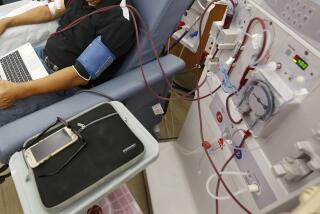
How Families Are Treated May Hold Key
- Share via
WASHINGTON — Two families at two hospitals confront the death of a child. Asked about organ donation, one says yes, the other no.
As the waiting list for organ transplants grows but donation rates remaining the same, the transplant community is trying to determine what makes the difference.
Much of it, they’ve concluded, depends on what happens at the hospital in the hours before death.
In-depth interviews with families who agreed to donation and those who said no, contained in a recent study, found donor families significantly more likely to believe that their loved ones received the best possible care and that everything was done to try to save them.
Conversely, many families who didn’t donate showed “a great deal of anger . . . as to how they were treated,” said William DeJong of the Harvard School of Public Health, who coauthored the study.
The study also confirmed how important it is for a family to know the deceased’s wishes.
Polling indicates many Americans are likely to donate organs if they believe that’s what the deceased wanted. But many people who say they would like to be donors have not told their families.
That concept is at the center of a national campaign to promote organ donation: “Share your life, share your decision.”
But the federal government and the private groups that run the transplant program are also focusing on what happens at hospitals. Among the concerns:
* A family is asked about donation too soon.
Sometimes well-meaning doctors and nurses mention donation before a family has been told that the loved one has died, often because the medical staff knows death is virtually certain. This plays into the fear that doctors won’t really try to save someone if they can get their organs instead.
The family survey found that only 46% of non-donor families said donation was brought up at the right time.
* Families do not understand brain death.
Most donors have died because their brains are no longer functioning, not because their hearts stop beating.
But that’s tough to understand when the person looks as if he’s sleeping or in a coma.
The survey found 45% of non-donors believed a brain-dead person was “in a coma” rather than dead, versus 28% of donor families who held that inaccurate view.
And only 60% of non-donors knew that “someone who is brain dead is dead even though his or her heart is still beating.” Eighty percent of donor families knew that.
* A hospital never notifies the local organ procurement group that a potential donor has died.
About one-third of the families of people who are medically suitable to donate are never even asked.
Some states have laws requiring hospitals to notify procurement officials after every death. The federal government plans to adopt a similar, nationwide rule--over the objections of hospitals.