OB Anesthesia--if Any--Is Something to Think About
- Share via
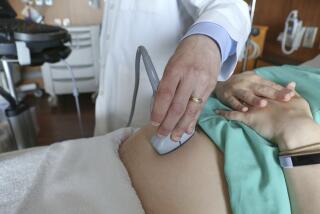
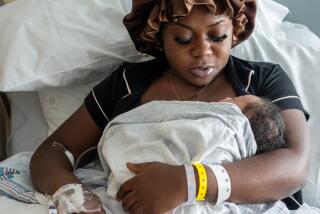
The case of Ozzie Chavez, a pregnant woman denied an epidural for labor and delivery at Northridge Hospital Medical Center in 1997 because she could not pay cash for it, raises a health care issue expectant mothers should think about carefully before childbirth: obstetric anesthesia.
OB anesthesia, which minimizes the pain and anxiety of labor and delivery, allows women to comfortably participate in the childbirth experience. Pain-control options, which range from natural childbirth to narcotic medication, can be incorporated into birth plans and performed during alternative childbirth methods like water deliveries. The choice of anesthesia depends on each woman’s threshold of pain and medical history.
Epidurals Offer Safe, Effective Pain Control
Epidurals provide almost instant relief from labor contractions via a catheter placed in the small of the back. Often used by obstetricians to perform at-risk procedures like multiple-birth delivery, this safe and effective local anesthetic can be administered at almost any stage of labor. Recent research demonstrates that epidurals do not increase the possibility of Caesarean sections or cause spinal injury, as some people mistakenly believe.
Arguably the most popular OB anesthetic, epidurals are not the only method of pain control available. Others include:
Intrathecal: Also known as a “spinal,” this technique relieves pain in the pelvic area and controls discomfort during labor and delivery through an injection to the small of the back. It can also be used to perform a C-section.
Co-Axial treatment: This combination epidural/intrathecal technique provides fast pain relief. Commonly called “walking epidurals,” co-axial treatments permit labor in an upright sitting position but not full patient mobility.
Pudential/paracervical block: A local injection into the walls of the vagina shortly before delivery blocks pain and prepares women for childbirth.
Patient-controlled analgesic: This patient-operated device lets women dispense narcotic pain relief as needed.
Local infiltration: A series of local injections, commonly used to repair tears in the cervix or perform an episiotomy, can prepare women for delivery.
Narcotics or tranquilizers: Administered intravenously or via injection, these drugs reduce but do not eliminate pain.
Natural childbirth: A drug-free method that employs techniques such as focused controlled breathing and coaching to promote childbirth.
Discuss Pain Control During Prenatal Care
Prenatal discussion of pain control better prepares women for the rigors of childbirth and contributes to the development of an overall birth plan. Though many pregnant women participate in prenatal birthing classes, few know the anesthesia options available to them. Prenatal planning gives women time to compare the cost and availability of anesthetic procedures at area hospitals and birthing centers and review health care coverage offered by insurance plans.
Prenatal counseling also affords health care providers the opportunity to review a maternity patient’s medical history and prepare for potential clinical emergencies during childbirth. Preexisting conditions, such as scoliosis, which can impede the delivery of spinal anesthesia, and such common phobias as a fear of needles, can be addressed prenatally.
Obstetricians and Anesthesia Providers Dispense Advice
Both obstetricians and anesthesia providers can answer questions about pain control. Obstetricians, who usually discuss pain control in the third trimester, may refer early prenatal questions and concerns to certified registered nurse anesthetists, who deliver most anesthetics to maternity patients. The following provides a list of questions to help expectant mothers choose among the options available to them.
* What are the anesthesia options available at this institution?
* What is the epidural rate at this institution?
* What procedure do most women request and/or receive?
* What procedure does my obstetrician or anesthesia provider prefer?
* How many procedures of this type have been performed at this institution or by this anesthesia provider?
Expect the Unexpected
Though many pregnant women hope to deliver drug-free, the unpredictable nature of childbirth requires a degree of flexibility in the selection of the preferred pain-control method. A low threshold for pain coupled with unanticipated medical complications may require some use of narcotic medication to control labor pain and promote delivery. Expectant mothers should not view anesthesia as a crutch or character failing since few women deliver drug-free.
*
Scott McGlothlen is a certified registered nurse anesthetist and staff anesthetist at Columbia Presbyterian / St. Luke’s Medical Center in Denver. An OB spokesman for the American Assn. of Nurse Anesthetists, he has performed more than 10,000 epidurals.