More than just a pesky cough
- Share via
The chronic, spastic cough started with what appeared to be a cold. A few months later, it was ruining Zachary Graham’s life. The 16-year-old Sunapee, N.H., resident was often left gasping for air, gagging and unable to sleep. During one particularly ghastly coughing spell, Betty May Graham, Zachary’s mom, feared her son was about to stop breathing.
That incident led the family to a lung specialist who delivered a diagnosis that stunned the Grahams: Zachary had pertussis, also known as whooping cough, a disease far better known in the 1930s than today.
“When the doctor said whooping cough, it kind of blew my mind,” the teenager says.
Adds his mother: “I had never heard of an adolescent having whooping cough. I thought, ‘He had his shots for that; how could he get whooping cough?’ ”
Doctors now believe they know.
They’ve found that the pertussis vaccine routinely administered to babies wears off in five to 10 years. As a result, a disease that was thought to be a relic of the past has reemerged and is finding fresh targets -- primarily teenagers and young adults.
Pertussis ran rampant in the early part of the 20th century, with around 250,000 cases -- and about 7,500 child deaths -- reported each year in the United States.
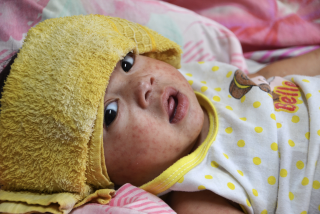
A highly contagious bacterial infection that causes severe coughing, the disease derives its common name from the “whoop” sound that infected infants make as they struggle to breathe while coughing. The infection often resembles a cold in its early stages, producing a mild fever, runny nose and cough; the cough then typically worsens and can last for two or more months.
A vaccine introduced in the 1940s sent pertussis cases in this country plummeting to a low of 1,010 in 1976. But the disease roared back in the 1990s. According to the national Centers for Disease Control and Prevention, about 10,000 cases were reported in 2003.
Experts say that number may be extremely low because many cases of pertussis go unrecognized.
Teens and adults almost always recover fully from pertussis, but that’s not the case with infants who have not yet been vaccinated or who are only partially vaccinated.
So far, few infants have died. Although physicians and public health experts say those numbers could grow if the problem is not confronted, they also believe a yet-to-be-approved booster shot could help keep the disease in check.
“For a vaccine-preventable illness, it is very concerning that this should even be happening,” says Dr. Jill Hoffman, a pediatrician at Childrens Hospital Los Angeles. An infectious disease specialist, she recently cared for two infants who were critically ill with the disease.
“Children die of pertussis,” she says. “We have about one death each year just in this hospital.”
The disease has probably been underestimated for many years, experts say. However, a recent upswing in cases -- pertussis outbreaks occur in cycles, with peaks emerging about every three years -- has brought new attention to the disease’s presence. Better lab tests have also made it easier to diagnose.
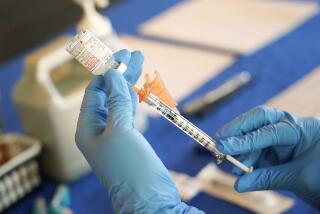
“The vaccine only lasts a short period of time,” says Dr. James Cherry, a professor of pediatric infectious diseases at the David Geffen School of Medicine at UCLA and a national authority on childhood vaccines. The vaccine, a combination diphtheria-tetanus-pertussis shot, is given in five doses -- usually at 2, 4, 6 and 15 months of age, with a final dose at 4 to 6 years.
“The biggest problem is older people taking it [the disease] home to newborns, where it can be fatal,” Cherry says.
Public health officials hope they can soon stop the rise of the disease. Two pharmaceutical companies have asked the Food and Drug Administration to approve a diphtheria-tetanus-pertussis booster shot that would confer an additional 10 or so years of immunity.
Vaccine maker Sanofi Pasteur is seeking approval to sell its booster, Adacel, to people ages 11 to 64. GlaxoSmithKline has asked the FDA to approve its shot, Boostrix, for those 10 to 18.
The FDA is expected to rule on the boosters this spring. Other than the five-dose diphtheria-tetanus-pertussis childhood vaccine, there is no licensed pertussis vaccine for people older than 7.
“This [booster] vaccine has the potential to be really helpful in controlling these outbreaks of pertussis,” says Dr. Amy B. Middleman, an assistant professor of pediatrics at Baylor College of Medicine in Houston. “The really important time to cover people is in the adolescent years. That seems to be where the incidence is rising the highest.”
Adults can get pertussis too. But outbreaks seem to be most common among teens and young adults who share crowded classrooms and dormitories.
Whether older adults also should receive a booster is the subject of much debate among experts. Cherry says his studies have shown that about 13% of adults with chronic coughs are actually infected with pertussis. The disease is transmitted by airborne droplets when the infected person coughs or sneezes. If one member of a household is infected, up to 90% of the other family members probably will develop the disease.
“The majority of infants who get pertussis get it from a family member over the age of 10, and 30% to 40% get it from the mother or father,” Cherry says.
A booster shot may be recommended for teens as well as any adult who could come in contact with an infant, such as adults who may have a baby, infant day-care workers and pediatric healthcare workers.
The pertussis boosters are similar to infant pertussis vaccines and are considered safe, says Cherry.
In fact, an effort to make vaccines safer in the 1980s may have contributed to the current pertussis upswing.
Before 1996, pertussis shots were made of the whole killed bacterium. The shots were linked to occasional reactions that included high fever and redness and swelling at the injection site.
The newer acellular vaccines, which contain only parts of the pertussis bacterium thought to be important for immunity, are considered safer. But some of the acellular vaccines were not as effective, Cherry says. The low risk of side effects from the acellular vaccine should be reassuring to parents whose teens may be targeted for booster shots, says Middleman.
“The booster is not a new vaccine,” she says. “It’s already used. I think it would be considered as safe in a teenager as it would in an infant.”
Some parents, however, harbor concerns about the safety of childhood vaccines and choose to forgo immunization. Other infants simply do not get regular healthcare. As a result, 15% of children in the U.S. do not get the diphtheria-tetanus-pertussis series, the CDC says. Theoretically, the unvaccinated children could be contributing to the rise in the disease, experts say.
The reemergence of pertussis should serve as a cautionary tale for people who are against immunizations, says Middleman.
“It’s always better to immunize than be concerned about the minimal risk of side effects,” she says. “The disease is always worse. But the public health value of immunization has been consistently underestimated since the immunizations themselves began to diminish cases of these horrid diseases.”
Doctors are also hoping that heightened public awareness about pertussis will lead to more timely diagnosis and aggressive treatment. Antibiotics, if given early enough, can make the infection less contagious, although they may not alleviate the symptoms.
“What happens with [adults] is that sometimes these people have been coughing for months and may be pretty sick. But adult physicians are not really trained to think about pertussis. They are not trained to treat it,” says Hoffman.
Adults who cough for longer than two weeks should be seen by a doctor, Middleman says. Pertussis can be diagnosed with a simple blood test. Adults with coughs should stay away from babies younger than 6 months of age.