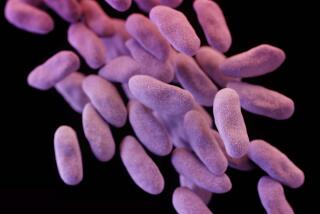
Infection Is Growing in Scope, Resistance
- Share via
It all began with what looked like a spider bite on Eileen Moore’s left thigh. Nothing to worry about, she figured.
Within 24 hours, the “bite” became a 6-inch welt with a bubble of pus that eventually ripened into a black wound. Over the next few months, scabs dotted her face. A hangnail caused her middle finger to bloat like a sausage. Her pierced ears oozed pus.
The cause of Moore’s ordeal was a bacterium known as methicillin-resistant Staphylococcus aureus, which in its most severe form can turn into a fatal flesh-destroying scourge.
For decades, the infections were found only in hospitals, where the constant use of different antibiotics, including the potent methicillin, made it resistant to many of the most powerful antibiotics.
In the last few years, it has emerged in gyms, jails, schools -- and just about anywhere bacteria can grow. It has become a simmering problem that is largely unknown by the general population.
“I would characterize it as widespread, and in some areas it is epidemic,” said Jeff Hageman, an epidemiologist at the Centers for Disease Control and Prevention and a coauthor of two studies on staph published last year.
There are few statistics on the disease, because resistant staph infections are not routinely reported to the CDC. But one study published last year in the journal Emerging Infectious Diseases estimated there were about 126,000 cases from 1999 to 2000 -- twice the number of hepatitis B cases each year.
“The rapidity with which this has emerged over the last two to three years is probably unprecedented,” said Donald Low, a microbiologist at the University of Toronto who was one of the key scientists who dealt with Toronto’s SARS outbreak in 2003. “When you look at the numbers, this way outstrips other so-called new infectious diseases.”
Its victims are legion.
Five football players with the St. Louis Rams developed lesions on their elbows, forearms or knees, where turf burns had opened up their skin in 2003. Players from a competing team also developed sores after playing against the Rams.
San Francisco has seen a surge of this antibiotic-resistant bacteria in intravenous drug users and homeless people.
In 2004, actress Hilary Swank found a blister on her foot while training at a Brooklyn boxing gym for her part in the film “Million Dollar Baby.” It turned out to be a staph infection.
Moore, a 38-year-old La Canada Flintridge software consultant, has no idea where she got her infection. All she knows is that it took four debilitating months with three increasingly powerful antibiotics to rid herself of the disease.
These days, she views every rash and pimple with suspicion.
“I’m a germophobe now,” she said.
*
A large part of the problem in combating the staph bacterium is that it is ubiquitous.
More than 30% of Americans carry some kind of staph infection in their nose. About 1% have the methicillin-resistant strain, and half of those have an even newer strain that is less resistant, but more damaging. Many carriers never develop a skin infection, either because they have some unknown immunity or because the bacteria never have an opportunity to penetrate their skin through a wound or rash. But carriers can still spread the disease.
Staphylococcus aureus was first identified in the 1880s. It was named aureus, or golden in Latin, because of its distinctive color.
It survived as a relatively undistinguished microbe until the mid-20th century. The introduction of the first antibiotic, penicillin, in 1941 set the bacterium on its deadly journey of mutation. It took just two years for reports to trickle in of the bacterium’s resistance.
In the early 1960s, doctors deployed a new antibiotic, methicillin, against the disease. The first signs of resistance appeared in less than a year.
The resistant strain became ingrained in hospitals in Europe, Australia and the U.S.
By the early 1990s, methicillin-resistant staph infections became the leading cause of hospital-acquired skin infections in the U.S. Recent studies have shown that this kind of staph bacterium has also colonized hospitals in Egypt, Taiwan and South America.
It was inevitable that the resistant bacterium would emerge elsewhere.
The first smattering of cases of what came to be known as community-acquired methicillin-resistant Staphylococcus aureus appeared as early as 1990.
The community strain is genetically different from that found in hospitals. Because it has not been bombarded by as many antibiotics, it is less resistant to drugs, but is more virulent.
To gauge the prevalence of the strain, researchers at Olive View-UCLA Medical Center in Sylmar analyzed skin infections that showed up in their emergency room. In 2002, methicillin-resistant staph caused 29% of those infections. Two years later, the rate was 64%.
A study published last year in the New England Journal of Medicine estimated there were about 26 community-acquired cases per 100,000 people in Atlanta and 18 per 100,000 people in Baltimore.
It is a hardy bug. The bacterium likes to grow in warm, moist areas of the human body, such as the nose, armpit or groin. It can linger on the skin without causing infection, waiting to enter through a cut or an abrasion. Unlike many other germs, it can also survive hours, possibly days, on inanimate objects such as towels or catheters.
Once inside the body, the bacteria can bloom into rashes, pimples and boils. But sometimes the bacteria cause invasive infections, such as pneumonia or meningitis. In a few cases, staph infections can turn into a nightmarish necrotizing fasciitis, the so-called flesh-eating disease. In rare cases, an infection can be fatal.
Lancing a wound is sometimes enough to stop a broader infection. But if the bacteria has spread through a person’s body, antibiotics are the only effective cure.
There is a hierarchy of antibiotics, starting with older drugs, such as penicillin, and working up to the most aggressive ones, including vancomycin and linezolid, which can cause serious side effects. Using the most aggressive ones first only helps to foster more drug resistance. Thus, infected patients are often initially prescribed antibiotics that have little effect.
When Thomas Lovato’s 9-year-old daughter, Cynthia, developed tiny red bumps on her hips and abdomen in August, her pediatrician thought the young girl had flea bites.
The pediatrician prescribed the common antibiotic amoxicillin, but the boils didn’t go away, said Lovato, a 38-year-old air conditioner repairman from San Jose. He tried to help his daughter by popping them.
Soon he spotted a pimple on his own neck that looked like an ingrown hair follicle. Within days it grew to the size of a quarter. Then a painful rash 10 inches wide erupted on his groin, he said. Another popped up on his chin.
In about a week, he developed a fever and went to the local emergency room, where doctors cut open the wound on his groin and prescribed amoxicillin, he said.
By the beginning of September, their boils were growing faster than they had before and were three times bigger. Cynthia would scream when anyone touched them. Pus started coming out from beneath Lovato’s fingernails. His 3-month-old son, Hayden, developed small bumps on the back of his head, Lovato recalled.
The whole family went back to the emergency room and the doctor prescribed different antibiotics, including rifampin, a drug commonly used to treat tuberculosis and leprosy, but which can cause liver damage.
They went on a mission to try to contain the infection. They wore surgical gloves when they tended their sores. They squirted sanitizer gel on their hands every time they touched anything. They scrubbed walls, doorknobs and surfaces with bleach and washed their bedding in hot water every other day. They skipped work and school for months, sequestered in their bedroom with little contact with the outside world, he said.
For the last month, they think they’ve been clear. But they fear the infections will return.
“We’re trying to be optimistic,” said Lovato’s wife, Lorraine, the only one to escape infection.
*
Amid the din of afternoon wrestling practice at Bell High School, 14-year-old Manuel Villegas pushed a microfiber mop infused with a disinfectant across purple gym mats.
“I’m not going to get it,” Villegas said. “That’s why I take two showers a day, before practice and after practice. I bring my own soap to the boy’s locker room.”
Rashes started popping up on Coach Eric Klein’s wrestlers about two years ago, and Klein quickly invested in the $200 mop. He didn’t know exactly what was causing all of the rashes -- maybe ringworm, maybe staph -- but he was worried.
Last season, he started asking the kids to lather themselves in a special wrestling foam that is supposed to provide a barrier to transmission.
“I spend a lot of money on having the mats cleaned,” Klein said. “The last couple or three years, it’s been a big stress.”
Just as Villegas was scrubbing the mats, teammate Jose Uribe, 16, walked in with a red flush on his arm and a dark crusty scab in the middle of it.
“I think it’s a spider bite,” he told his teammates. Uribe said he saw a doctor, but he couldn’t remember what kind of infection the doctor said it was. He said he was taking penicillin.
Klein barked at Uribe to tape up his arm. “Did the doctor say it was OK?” he asked.
Uribe nodded.
A large part of the problem with the spread of drug-resistant staph is that it is difficult to diagnose. The only way to tell for sure is a test that can take up to three days for results.
Eileen Moore, the La Canada resident, started on the common antibiotic Keflex and ended with rifampin.
“When I think how I have something that’s resistant to all Western medicine, or almost all Western medicine, that’s scary to think about,” Moore said. “Had I been resistant to those other antibiotics, I could have died.”
Dr. Thomas Horowitz, who treated Moore at his office in downtown Los Angeles, said if rifampin didn’t work, he was prepared to check her into the hospital and set up an intravenous drip of vancomycin, considered one of the antibiotics of last resort.
“We’re seeing resistance to so many of the antibiotics, and so little new antibiotic research is going on,” Horowitz said.
Ten years ago, a strain that could partially resist vancomycin surfaced in Japan.
A totally resistant strain emerged a few years later in Michigan. Doctors have recorded six cases worldwide, all in the U.S.
*
(BEGIN TEXT OF INFOBOX)
Microscopic menace
*
Within a few years of the introduction of penicillin in 1941, antibiotic-resistant forms of Staphylococcus aureus began to appear. These bacteria, once found only in hospitals, have now emerged in the general population.
*
Staph infection chronolgy
--
Late 1880s: Scottish surgeon Alexander Ogston identifies a bacterium, Staphylococcus aureus.
1928: British scientist Alexander Fleming discovers the first antibiotic, penicillin.
1941: Penicillin becomes available in the United States and England. The first penicillin-resistant Staphylococcus aureus is reported a short time later.
Late 1940s: one-quarter of Staphylococcus aureus bacteria in hospitals are penicillin-resistant.
1958: Vancomycin, still considered an antibiotic of last resort, is introduced.
1959: The antibiotic methicillin is introduced.
1961: Doctors find the first cases of methicillin-resistant Staphylococcus aureus.
2002: Doctors find vancomycin-resistant Staphylococcus aureus in the United States.
Today: Over 95% of Staphylococcus aureus worldwide is penicillin-resistant and 60% is methicillin-resistant.
*
Sources: U.S. Food and Drug Administration, Princeton University, Chemical Heritage Foundation, National Academy of Sciences, ActionBioscience.org