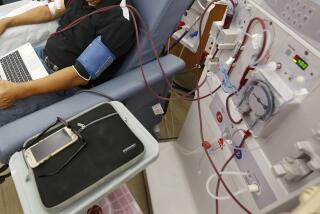
Trust and transplants
- Share via
EVER SINCE DOCTORS PERFORMED the first successful kidney transplant in Boston in 1954 -- from one identical twin to another -- the biggest worry in the field has been finding enough organs for the tens of thousands of people who linger on waiting lists each year. As recent reports indicate, that worry was not misplaced -- and the best way to address it is through better oversight.
Last week, Times reporters Charles Ornstein and Tracy Weber revealed that Kaiser Permanente in San Francisco put patients at risk when it hastily started a kidney transplant program in 2004 and forced members waiting for transplants elsewhere to join it. Because of staffing problems and paperwork delays, patients needlessly waited months for kidneys that never arrived.
To make matters worse, more than two dozen people lost out on nearly perfectly matched kidneys because hospital officials rejected organs during the transition but never informed patients. Kaiser Permanente now says that its patients can go outside its network for transplants, and its top official in Northern California has officially apologized.
This follows news last fall that St. Vincent Medical Center in Los Angeles misappropriated a donated liver to a Saudi citizen who ranked far below one of its own patients on the regional waiting list. The local patient later died. Weeks later, it was revealed that yet another center, UC Irvine, was turning down livers for transplant at two to three times the rate of other hospitals because it didn’t have enough full-time surgeons -- issues it failed to disclose to patients and regulatory officials.
All three hospitals have promised or started internal inquiries, and both state and federal regulators are investigating. But regardless of what they find, it’s clear that more checks and balances are needed. Today, a mix of public and private agencies oversee transplant programs, and they have different rules. The United Network for Organ Sharing, a federally funded group that is the closest thing to a regulatory agency for the field, admits its oversight responsibilities are unclear.
It is, of course, important to allow doctors and hospitals to innovate and experiment with medical procedures such as transplants, and too much oversight can be stifling. But the current arrangement needs more oversight, and the U.S. Department of Health and Human Services could provide it.
Thousands of people are alive today because of the work of transplant centers around the country. But the continued success of these programs rests on keeping the public’s faith that these surgeries are safe and that patients are getting the best possible care.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.