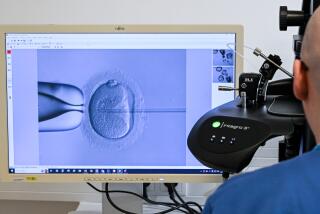
Shots, eggs, embryos and a big dose of hope
- Share via
Fairfax, Va. — CHAD AND DAVID CRAIG FIDGETED in the waiting room like expectant fathers, which is, after all, what they were.
Just down the hall, in a sterile surgical suite, a young woman they had met only once had her legs up in stirrups. Dr. Suheil J. Muasher, a fertility specialist, gripped a long silver needle between his right thumb and forefinger and twirled it gently as he guided it through her vaginal wall and into her right ovary.
“It’s full of follicles,” he said approvingly, glancing at an ultrasound monitor to track the needle’s path.
The follicles showed up on the screen as black blobs. Each contained an egg the size of a dust particle. As Muasher punctured the first sac, he stepped on a foot pump and suctioned it until it collapsed and disappeared. Fluid the color of fruit punch streamed through a catheter attached to the needle and into a test tube.
The fluid was spirited into an adjoining lab, decanted into a dish, and examined under high magnification by one of Muasher’s embryologists.
“Do you have anything?” the doctor called.
“I have a first egg,” his assistant announced. She transmitted an image resembling a star cluster onto a monitor in the operating room. The anesthesiologist, Dr. David C. Yarnall, couldn’t resist. “Looks like it’s sunny side up,” he said.
The date was Oct. 9, 2004, and Chad and David had been awaiting this moment for nearly two years. It was the first significant medical step in their unconventional quest to become fathers, an undertaking that would have been inconceivable a few years earlier.
As gay men trying to produce genetic offspring through a gestational surrogacy arrangement, Chad and David had invested their hopes and their savings in the primacy of technology over biology.
They knew from years of research into assisted reproduction that success was never guaranteed. And their process would have more moving parts than most. They were paying one woman to provide her eggs, and another to carry their artificially inseminated embryos to term. To make it all happen, they had assembled a team of doctors, nurses, embryologists, technicians and lawyers. Things could go wrong at any stage, and Chad and David would have little control over events beyond playing the odds.
At the moment, none of that mattered. After months of planning and anticipation, it felt to them like Christmas morning.
“We are absolutely on the edge of our seats,” said Chad. “The process is such a test of patience. Tons of waiting and then quick and short bouts of intense progress. I am guessing it will just hit me all at once that we are finally about to be pregnant.”
Their fate now depended on the intricate choreography Muasher had directed by prescribing various fertility drugs to stimulate the egg donor’s production, synchronize her reproductive cycle with that of the surrogate, and prepare the surrogate’s uterus to accept an embryo.
They knew their egg donor only as Jessica, but their dreams of building a family relied heavily on this near total stranger. She was single and 25, in her egg-producing prime, but she had never been pregnant or donated eggs before.
For the previous three weeks, at Muasher’s direction, Jessica had injected herself daily with hormones. Each morning, she numbed one of her hips with an icepack and jabbed it with Lupron, a synthetic formulation that prevented her from ovulating until the desired moment.
At night, she gave herself two shots that stimulated egg production -- Follistim (derived from the ovarian cells of Chinese hamsters) and Repronex (extracted from the urine of postmenopausal women). In addition to bruising from the injections, Jessica suffered side effects like sleeplessness, headaches and bloating that sometimes forced her to unbutton her jeans.
Muasher carefully monitored her hormone levels and follicle development through regular blood tests and sonograms, and tweaked the dosages accordingly. The adjustments were critical to warding off a rare but dangerous condition known as hyperstimulation, which could lead to renal failure or blood clots.
“It’s more of an art than a science,” Muasher explained, “because people respond differently to the medications.” Indeed, he had tried to treat Jessica conservatively, but based on her sonograms he projected she would yield at least 20 eggs, well above average.
Precisely 35 hours before Muasher planned to retrieve the eggs, Jessica gave herself a final “trigger shot” of yet another hormone that would prepare her follicles for ovulation. The timing of the procedures was calculated so that the peak of her egg maturation would dovetail with the priming of the surrogate’s uterus for maximum receptivity.
That moment did not always coincide with office hours. When Muasher began suctioning Jessica’s follicles, it was 7:45 on a Saturday morning. Chad, 33, and David, 36, steeled themselves in the waiting room with coffee and Krispy Kreme doughnuts as the doctor methodically punctured one sac after the next. With a single swift stroke, he guided the needle through three abutting follicles, like a toothpick through cocktail olives.
After he finished, Jessica was wheeled into recovery, where she emerged quickly from a deep sedation. “How many eggs?” she asked groggily.
“We did very well here,” Muasher reported. “We got about 26 eggs.”
“Woo-hoo!” she cheered.
“You go, girl,” said the anesthesiologist.
After Muasher informed Chad and David of Jessica’s bountiful harvest, they donned yellow surgical gowns and blue hairnets to greet their heroine. Though her full identity was to remain anonymous, she had agreed to let them visit her in the recovery room.
“Twenty-six! Twenty-six!” she grinned, giving a thumbs-up.
“Oh my gosh, you’re such a trouper,” David said. “Fertile Myrtle.”
They presented her with an arrangement of white roses and yellow freesia, and then a box from Neiman’s. It contained a sterling Konstantino bracelet, adorned with egg-shaped gold balls.
“How do we even begin to thank you for the generous gift you have given us?” began the handwritten note. “Each and every day from this moment on will be an unfolding miracle for us.”
Jessica was touched. “Oh, guys, that’s fabulous,” she said. “Thank you so much. So, do we want to take bets on how many babies there are going to be?”
“Everything over two,” David joked, “we give away as Christmas presents.”
Creating embryos
SHORTLY after the egg retrieval, Muasher’s embryologists returned to the lab, where they thawed, washed and counted the sperm that Chad and David had donated months earlier.
In late August, it had fallen to David to collect the frozen samples they had deposited at the Fairfax Cryobank and transport them the few blocks to Muasher’s office. He had never felt as self-conscious as he did leaving the sperm bank with a tall, cylindrical canister in each hand.
In the lab that Saturday, the embryologists used a pipette to draw up a drop of sperm from each man’s sample and release it onto a counting chamber -- essentially a microscope slide overlaid with a grid. By averaging the number of sperm in several squares, and the percentage that were moving forward, they could derive sperm counts and measures of motility.
The two samples were visibly different. Chad’s sperm scurried frenetically like mice through a maze. David’s, by contrast, seemed in no hurry.
Six hours after the egg retrieval, Jessica’s 26 eggs were divided into two batches. They had been rinsed in a special medium of proteins and nutrients and placed in an incubator at body temperature. The embryologists fertilized one batch with Chad’s Olympian swimmers and the other with David’s lollygaggers (he preferred to think of them as “overcalculating”).
That night, the prospective fathers talked about how the ingredients of life were brewing in a dish. “It’s not just genetic material now,” Chad said. “It’s together. The creation of this life has started.”
Early the next morning they got a call from one of Muasher’s nurses. Of the 26 eggs, 16 had fertilized, nine from David’s batch and seven from Chad’s. “It sounds like we’ve got enough for several tries,” David said.
So long as Muasher deemed the embryos of comparable quality, Chad and David wanted him to transfer one from each batch. This so-called “dual embryo transfer” would increase the odds that their surrogate, Whitney Cruey, would get pregnant, while also increasing the chances of twins. Chad and David had always been comfortable with that prospect; they wanted siblings, and twins would give them two for the price of one.
Some doctors would not perform dual embryo transfers, because in cases of genetic defects they would not be able to determine a child’s paternity without DNA testing. That was exactly what appealed to Chad and David. If possible, they wanted to cloak the paternity of their children, even from themselves, in order to reinforce their equal stature as parents.
With twins, each man presumably would be the biological father of one, though they wouldn’t necessarily know which. With a singleton, each would have had an equal chance at being the genetic contributor. If Muasher determined that one man’s embryos were better than the other’s, they had instructed him to transfer two from that batch, but not tell them whose it was.
The couple recognized there might be an obvious resemblance, or that they might have to learn paternity for a birth certificate. But this way, at least during the pregnancy, if someone had the nerve to ask who the “real” father was, they could answer honestly that they had no idea, or that both of them were.
In addition to choosing which embryos to transfer, Muasher had another critical decision to make -- whether to transfer the embryos after three days, when they typically would have grown to eight cells, or after five, when each would have become a mass of 100 or more cells known as a blastocyst. Three-day transfers were more common, but some research suggested that blastocysts were more likely to implant in the uterine lining.
Muasher felt it was an open question. You could expect to lose embryos between the third and fifth days of incubation, meaning there would be fewer to freeze for a second attempt. And if more than one blastocyst were transferred, the odds of a multiple pregnancy would be high. Twins and triplets, while sometimes desired, carried greater risks of miscarriage and premature delivery.
Three days after the egg retrieval, Muasher studied the embryos and saw that a number had cleaved into eight cells. He summoned Chad, David and Whitney to his office that morning.
He told them he had graded 12 of the embryos as good candidates for transfer, based on their structure and cell division. He would try to pick the best one from each man’s batch and freeze the rest.
“We’re looking at a 50 to 60% chance of success,” he said. They had a young egg donor -- the most important variable -- and pregnancy was more likely with fresh embryos than with frozen ones. If Whitney got pregnant, the odds of having twins would approach 30%.
Statistically, this first transfer would be their best shot.
Pregnancy hopes
WHITNEY felt ready to play her part. A 25-year-old college student, waitress, and single mother from Frederick, Md., she had been wearing estrogen patches on her lower abdomen for nearly three weeks. As the estrogen seeped into her body, it coaxed her uterus into reacting as if she were ovulating. The hormonal surge made her so emotional she found herself sobbing through “Fahrenheit 9/11.”
On the day Muasher collected Jessica’s eggs, Whitney added a daily shot of progesterone to thicken her uterine lining. It was administered with a 2-inch-long needle. If she got pregnant, she would have to continue the shots and patches for up to two months, one of many burdens she would endure for her $20,000 fee. (If she did not get pregnant, she would receive just $2,000, plus $500 for each unsuccessful embryo transfer.)
In the nearly five months since Whitney had signed on with Chad and David, they had made a point of going to dinner and visiting each other’s homes. But the time they spent together only seemed to magnify their differences.
She couldn’t relate to their vacations in Tuscany and the concert tickets they bid for on EBay. She found herself afraid to touch anything in their immaculately decorated house. Their walk-in closet was the size of her apartment bedroom, and she wondered if they had any idea how much baby-proofing the place would require.
On the morning of the procedure, classical music lilted through Muasher’s operating room as he prepared Whitney to receive the embryos. Dressed in blue scrubs and masks, Chad and David took seats just to her left, and reached for each other’s hands.
The embryologists flashed magnified images of the two embryos onto a monitor in the O.R. They looked vaguely lunar, their eight cells like craters in a gray landscape. This is surreal, Chad thought, our first view of our children.
“They look almost perfect,” Muasher said. “This is the uterus there. We’re going to try to put the embryos right in the middle.”
Muasher took the catheter containing the embryos, which were suspended in fluid, and maneuvered the tip into place. He depressed the plunger on the syringe and held it for 15 seconds. After withdrawing the slender tube, he handed it to an embryologist to check under a microscope. She returned to say the embryos were gone.
Whitney smiled serenely throughout the procedure, which she said was no more uncomfortable than a Pap smear. Muasher instructed her to limit her activity for 24 hours, and to return in 13 days for a pregnancy test. He handed Chad and David the culture dish that had held the embryos.
“If it works, this will be like your first baby crib,” he said. “Good luck.”
Chad and David were amazed by what they had witnessed. As they settled in for their two-week wait, they were utterly convinced Whitney was pregnant.
Getting the news
WHITNEY arrived at the Craigs’ house in northwest Washington about 11 a.m., her 2-year-old daughter in tow. It was a dreary morning, with a white fog enveloping the Washington Monument. She had just given blood at Muasher’s clinic and the nurse had told her to call at 2 p.m. for the pregnancy test results.
Chad arrived home from work with 20 minutes to spare. “I’m so stressed out that I’m beyond stressed out,” he announced.
The two-week wait had been tough on him. Unable to focus at work, he kept searching the Web for pictures of embryonic development so he could imagine what their child might look like on any given day.
Chad slid into a kitchen chair next to David, who placed the phone on speaker and called Muasher’s office. The room was silent as the call routed from one assistant to the next and then to the doctor.
“Hello?” His thickly accented monotone was instantly recognizable.
“Hey, Dr. Muasher,” they replied in unison.
“Hi, how are you?”
“Fine, how are you?” David replied.
“Good, who do we have there?”
Chad listed those in the room.
“How’s everybody doing?”
“We’re doing fine,” they all answered. It was starting to seem like too much small talk.
“Good,” he said, and paused. “I’m really sorry, you know, I don’t have good news.”
Chad’s head dropped.
“The test was negative, unfortunately. I’m really very, very sorry. I mean, all of us are sorry. This is one of those situations where everything went fine, we expected it to work, and it just didn’t work.”
“So what do we do next?” David asked.
Muasher explained they could try a second transfer with frozen embryos in as little as three weeks. Whitney would have to stop her medications, wait for her period and then start a new regimen.
“Is that all right with you, Whitney?” David asked.
Her voice cracked. “Yeah,” she whispered. “That’s fine.”
The doctor gave her instructions, told Chad and David to set up an appointment, then apologized twice more.
Whitney started to tear up.
“Hey, listen,” David said, “it’s certainly not your fault.”
“I’m going to cry,” she said.
“No, don’t cry,” said Chad, his own face puffy.
“It’s a roll of the dice and we’ll just keep going,” David said.
Whitney began sniffling. “I’m sorry,” she sobbed.
“Don’t be sorry, Whitney,” David said. “It has nothing to do ... it’s just ... you know ... it’s sad for all of us but we’ll try to do it again.”
They thanked her for all she had done, walked her to her car and hugged her goodbye. Both men dug their hands in their front pockets as she backed out of the driveway.
Chad and David started making calls -- their mothers, their friends, Chad’s sister, who was seven months pregnant with her second child.
“It’s just one of those things,” David told his mother. “You know, everything happens for a reason.”
It was a family motto, and Chad and David had made it the guiding tenet of their Christian faith. God always had a purpose, though it might not reveal itself immediately. Perhaps the point here was to bring them closer to Whitney, David mused.
During the two-week wait, Chad had sent an e-mail to friends and family members informing them of the surrogacy project. As he followed up with a note that afternoon, he could not believe how arrogant they had been to assume it would take the first time.
“Please know that we have great faith that this will work and we will one day have a baby,” he wrote. “It’s just a matter of when.... God is teaching us about patience.”
Playing the odds
SUHEIL Muasher felt terrible for the guys, as he liked to call them. It was the first time he had treated two men as patients, and he’d badly wanted it to work.
“You wish you could call everybody with good news,” he said the next day, “especially with cases that you work the hardest on. And in this case, we had to coordinate things with multiple people.”
Born in Amman, Jordan, the doctor came from a prominent family; his brother, a one-time ambassador to the United States, was then deputy prime minister.
Muasher, who immigrated to the U.S. after training as an obstetrician at Johns Hopkins, represented a link between the earliest achievements of assisted reproduction and its newest and most controversial applications. He had studied and worked for more than two decades under Howard and Georgeanna Jones, the legendary husband-wife team who created the first IVF baby in the U.S. (and 15th in the world) in 1981.
The Joneses and their superiors at Eastern Virginia Medical School in Norfolk had never been completely comfortable with the use of IVF for patients without conventional fertility problems. But after Muasher went into business for himself in early 2004, he recognized that gay men might form a promising niche market.
He had no moral qualms, but he did have practical ones. He had wanted reassurances from the Craigs’ lawyer that provisions had been made to care for their children if they went separate ways.
It frustrated him -- and them -- that he couldn’t find an explanation for Whitney’s failure to get pregnant. All the component parts -- Jessica’s eggs, both men’s sperm, Whitney’s uterus -- had seemed ideal. It was always possible he had simply selected embryos with undetectable chromosomal abnormalities.
At an appointment in late October, Muasher explained that the odds of success would decline with the next attempt. The remaining embryos had on first inspection been deemed inferior to the two he had already transferred. And only 70% to 80% of embryos typically survived the stresses of freezing and thawing.
Playing the odds, they decided to thaw five of their frozen embryos, hoping three would survive to be transferred.
As they wondered how many attempts it might take to get pregnant, they began to feel the press of time. Not only was the process getting more expensive by the day, but on Nov. 2, 2004, when George W. Bush was reelected, 11 states passed constitutional amendments to prohibit same-sex marriage. Chad and David understood the next front in the culture wars might well be gay parenting, and they feared the political tide would surge before they could complete a pregnancy.
On Nov. 17, Muasher called with unsettling news from his lab. His staff had thawed the five frozen embryos and only one was remotely viable. Deeply discouraged, they authorized him to thaw the remaining five.
Things only got worse when Chad, David and Whitney arrived at the clinic early the next morning. Of all the thawed embryos, only one was suitable to transfer. Muasher could not explain the extraordinary loss rate. He and his chief embryologist had checked conditions in the lab and all seemed fine.
“It happens maybe 2 to 3% of the time,” he said.
Chad and David were starting to feel they weren’t very good at this. “Now we really do need a miracle,” Chad said. “We need to beat the odds big time.”
Nobody was surprised when Muasher called two weeks later to say Whitney was not pregnant.
Harder to give up
NOW their frustration was palpable, bordering on anger. Chad had foolishly thought his obsession with research would give him a measure of control. Instead, he had a head full of information and no answers.
They faced the same questions so many infertile couples confront after repeated rounds of IVF. How long should they keep trying? How much bad news could they take? Was there a physiological problem or a lab problem, or were they just unlucky? Were they throwing good money after bad?
They had spent nearly $70,000, much of it from a home equity loan. The costs would escalate rapidly with a second egg retrieval, and they were running out of cushion. Yet the more they invested, financially and emotionally, the harder it was to back away.
“This process just sucks,” Chad said. “Oh my God, I don’t know how people do this for years. You better have twice as much money as you think you need and three times the patience.”
“And four times the time,” David added. “I thought we’d have kids in kindergarten by now.”
Whitney remained committed to Chad and David, but the process was wearing her down as well. The drugs made her sleepless and moody. She couldn’t help but feel responsible for the failures. Her boyfriend had started calling her a “guinea pig.” And if she didn’t get pregnant, she would not receive the lion’s share of her fee.
“I feel I’m trying so hard to make this happen,” she said.
Though their confidence was shaken, Chad and David decided to stick with Muasher through another round. It didn’t hurt that he offered a 20% discount.
Their lawyer, Diane Hinson, got in touch with Jessica, who instantly agreed to a second egg retrieval. This time she yielded 32 eggs, even more than before. Chad and David rewarded her with earrings to match her bracelet.
“If we have to do it a third time, you get a tiara,” David said.
“Is it wrong to hope?” she teased.
Twenty-seven of the eggs fertilized, 14 by one of the men and 13 by the other. Their friend Lisa Alexander observed that they seemed to be “over-egged and under-uterized.”
At Muasher’s recommendation, they froze 12 of the day-old embryos and let the rest grow to the blastocyst stage. Seven made it.
On Feb. 1, 2005, Muasher picked the two best blastocysts -- they were from the same batch -- and placed them in the center of Whitney’s uterus. The others were frozen.
Again they all gathered in the Craigs’ kitchen to receive the news. And again it was negative.
When Muasher finished his apologies, David looked at his partner. “We just can’t get it right, can we?” he said.
“Is it possible he’s doing something wrong?” Chad asked dejectedly. “Everything looked so perfect.”
To try to isolate the problem, Muasher suggested new tests on Whitney, including a biopsy of her uterine lining. The tests would be invasive and costly. And if they detected trouble, such as a blockage, it might require surgery. Whitney, who had already been subjected to 64 injections and 164 estrogen patches, hadn’t signed on for that.
New possibility
Ten days after the third negative pregnancy test, Chad got a call from his 33-year-old sister, Tonya Rosenberger, who lived in Arlington, Texas. Sissy, as the family called her, had just delivered a second child after a wonderfully easy pregnancy, and had been tracking her brother’s efforts closely.
She sensed that Chad and David were running out of money and resolve, and she thought she might have a solution.
“What would you think about me being the surrogate?” she asked Chad. “You wouldn’t have to pay me.”
“Are you kidding me?” Chad asked. “My God, I’m thrilled, but I don’t know what to think.”
What he really thought was that it was too much to ask. Did she fully understand what she was volunteering to do?
He knew Sissy was terrified of needles. And because Texas statutes were neither surrogacy-friendly nor gay-friendly, she and her two kids might have to spend the last eight weeks of the pregnancy with them in D.C. to be sure she delivered in Maryland.
How would her husband, Jay, feel about her carrying her brother’s child? Only a year earlier, they had balked at her being the egg donor.
Sissy told Chad they had discussed the idea, and that Jay, an engineering professor, was fully on board. Surrogacy, he had remarked, was “like loaning someone your car, only a little more.”
Sissy assumed she would develop a special bond with the baby, and might even suffer postpartum depression. But she thought it would be worth it to know that Chad and David finally had a child to love.
“Any kid would be lucky to grow up with them as parents,” she said. “I wish they would adopt me sometimes.”
She told Chad, “This is something we really want to do for you.”
The only complication, she said, was that she wanted to breastfeed her baby, Anabelle, for six months. She would not be able to start the surrogacy process until midsummer.
Chad’s head spun with the possibilities. He and Sissy, separated by 12 months and two weeks, had been close since early childhood, their bond forged by the shared trauma of their parents’ divorce. The journey would be much more meaningful with her along for the ride.
“I think it will make everything better,” Chad said, “but it has the potential to make the bad stuff, like negative pregnancy tests, even more painful.”
Their mother, Debbie Young, who still lived in south Georgia, told them she thought it would be wonderful. She was moved that her children remained so connected. Whatever horror she had felt when Chad came out 15 years earlier seemed long forgotten.
She worried, though, that failure could come between Sissy and Chad. Her daughter was headstrong. Her son was sensitive. Sometimes they clashed. This would be the fourth attempt at a pregnancy, and she thought Sissy might feel the pressure.
“Chad,” she said one day, “you do realize there’s a possibility the same thing could happen. I’m not trying to be a downer here, but I don’t want any problems between y’all if it doesn’t work out.”
“I realize that, Mother,” he said. “I know all of that.”
Sissy and Jay knew suburban Dallas might not be the easiest place to carry a child for two gay men. Jay wasn’t going to advertise it around the campus where he was trying to gain tenure. They were prepared to lose some friends, and to deflect any questions with humor.
“Didn’t you know,” Sissy would drawl, “that it’s a tradition in south Georgia to have your brother’s baby?”
Feeling optimistic
THAT summer, Chad and David made a rather sudden decision to move from Washington back to Atlanta, where they had met eight years earlier. The cost of living would be lower, and it would bring them closer to family. Chad’s stepfather had been ailing, and his mother needed a hand.
They made a tidy profit on their house and used it to pay off their surrogacy debts. In Atlanta, they bought a two-story manor and began a top-to-bottom renovation, with plans to move in December.
The legal process to help Chad and David take clear title to their children had already been complicated by the selection of a surrogate from Texas. Now they would need lawyers and doctors in three states, each with its own adoption laws and birth certificate practices.
They were moving to a state where, only a year earlier, 76% of voters had supported a constitutional amendment banning gay marriage. There were rumblings in the Georgia Capitol that social conservatives might introduce legislation in the next session to ban gay adoption. The clock was ticking.
Sissy weaned Anabelle in August and began her drug regimen. She flew to Washington in late October and prepared for the Nov. 5 embryo transfer. Diane Hinson drafted contracts saying that Sissy would carry up to triplets.
Muasher was pleased to have a new variable in the equation. This round, he decided to thaw eight of the frozen day-old embryos. Six survived the thaw, and the doctor allowed them to grow for two more days.
To improve their chances, he decided to transfer three. At Chad’s request, he utilized a chemical process called assisted hatching, designed to help the embryo implant in the uterine lining.
Chad hugged Sissy on her way into the operating room, and he and David held hands at her side as Muasher transferred the embryos. “I hope this is the moment,” Sissy prayed.
She was amazed at how brief and antiseptic the procedure was. “If I’m going to get pregnant,” she told herself, “the least they could have done is put a little mood music on.”
Muasher, as always, exuded optimism. “I think we have a good chance,” he told them as he finished.
After Sissy returned to Texas, Chad called every day to see if she noticed any symptoms. “How’s your uterus feeling?” he would ask, making her laugh. At first there was some cramping, but then it disappeared. As the pregnancy test neared, she could feel the tension mounting. “They’re just so positive about it,” she said of Chad and David. “It makes me nervous.”
On Nov. 17, Sissy gave a blood sample in the morning, and later collected the results in a sealed white envelope. It stared at her from the kitchen counter as she waited for Chad and David to arrive on a late-afternoon flight from Washington.
After exchanging hugs and some chitchat, Sissy grabbed the envelope and tapped it on the counter.
“D’you want to do it?” Chad asked.
“I’m very nervous about it,” she said.
Chad took the letter, ripped it open, and instantly made sense of the numbers. “Negative,” he said. “It’s negative.”
A last chance
Chad and David didn’t know what to do. They had frozen embryos remaining, but was it worth putting Sissy through another round of hormone treatments? They wondered whether they should raise their odds by starting over with a fresh embryo transfer, perhaps with a new egg donor.
When they heard that Whitney’s boyfriend had gotten her pregnant, it reinforced the hypothesis that Jessica’s eggs, though high in number, might be low in quality. But finding a new donor would add months and tens of thousands of dollars to the process. And it would leave their remaining embryos in frozen suspense, a prospect that made them uneasy.
“I don’t want to leave them out of the game,” David said.
Muasher, meanwhile, had thrown up his hands. “I tried my best here,” he told David in a phone call the next day, “but I don’t know what else to do. I’m ready to give up.”
Chad and David looked into doctors in Dallas, but could not find one that would work with gay men. A clinic in Atlanta said it would take them, but would not transfer embryos from both simultaneously. Furthermore, transporting frozen embryos could be risky.
Muasher agreed to give it one more shot. This time, Chad and David wanted to transfer three blastocysts, pushing the boundaries of accepted medical practice. To prevent high-risk multiple gestations, fertility industry guidelines recommended the transfer of no more than two embryos in most instances, and fewer in the case of blastocysts. Muasher stunned them when he said that, given their track record, he would even consider transferring four. “I’m good with three,” Sissy interjected. “Four makes me nervous.”
On Jan. 9, 2006, Muasher’s staff thawed the four remaining day-old embryos and began the delicate process of growing them into blastocysts. Later that week, they also thawed the five blastocysts that had been frozen previously. When Chad, David and Sissy sat down in Muasher’s office, he told them he planned to transfer three embryos -- all from the bunch that had been growing all week. Two of the embryos had been fertilized by one man, and one by the other. There would be none left.
Because expectations were low, the mood was light. Chad had stuck a lucky penny in his loafer, and David joked that Sissy should put it in her uterus.
As they left to prepare for the transfer, David told Muasher that perhaps this would be the last time they would see each other. “I honestly hope so,” the doctor deadpanned, and they all laughed.
The statistics told them that this final attempt would be the least likely to work. They had four failures behind them. They were using second-string embryos that had been frozen and thawed and then cultured for five days in a dish. The odds had broken against them for 15 months. This time, they were lower than ever.
Next: Will Chad and David become fathers?
*
*
About this series
For more than two years, National Correspondent Kevin Sack followed Chad and David Craig as they attempted to become parents through a gestational surrogacy arrangement. The Craigs provided confidentiality waivers to their physicians and lawyers, giving Sack broad access to the inner workings of the process. Sack interviewed more than 90 people for these stories. He also reviewed hundreds of documents, including e-mails, contracts, government reports and court decisions.
Sunday: The journey begins
Today: Trying to make a baby
Tuesday: Will Chad and David become fathers?
*
On latimes.com
See additional photos as Chad, David and the team try to make a baby, along with the first story in this series. Go to latimes.com/surrogacy.