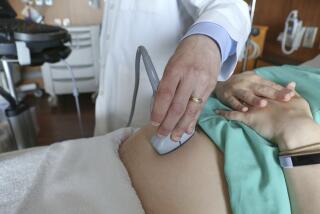
All in good time
- Share via
Her first baby wasn’t due for four days, but Misa Hayashi was advised by her obstetrician during a routine exam to check into the hospital that day.
“The doctor said the baby was too big for me to push out and we should go ahead and induce labor,” says the Alhambra woman, 24. “I didn’t really question it. Induction sounds so common. We went home and packed a bag and checked in at the hospital.”
Once there, however, Hayashi’s plans for an uncomplicated birth faltered. After receiving the drug Pitocin to trigger contractions, she labored for 20 hours. The pain was so intense she needed medication to ease it -- something she had hoped to avoid -- and eventually the baby became distressed, requiring constant monitoring of his heart rate.
Finally, almost a day after Hayashi entered the hospital, her son was born. Although he was healthy at 7 pounds, 10 ounces, Hayashi was left questioning the wisdom of labor induction.
Some hospitals and healthcare organizations across the nation share her concerns. Several have barred elective labor induction under certain circumstances, such as before 39 weeks of gestation (one week before the due date) or when there isn’t clear evidence that the mother’s cervix is primed for childbirth.
“There is renewed interest in these seemingly benign medical interventions,” says Dr. William Grobman, an assistant professor of maternal-fetal medicine at Northwestern University. “But the topic is somewhat hazy. We don’t have all the information we’d like to have about risks and benefits.”
The move appears to be a push back against the trend in recent decades to medically manage childbirth. Fewer than 10% of women underwent induction in 1990, but more than 21% did so in 2004, according to federal government statistics. No one knows how many of those inductions were prompted by legitimate medical concerns. But various studies have put the number of inductions for convenience at 15% to 55% of the total number.
At the same time, rates of caesarean sections increased to more than 29% in 2004, up from 23% in 1990, with many women requesting elective C-sections -- surgical births without any medical justification. That trend too has generated debate about whether patients are undertaking unnecessary risks.
Labor induction is frequently, and legitimately, recommended when health problems complicate a pregnancy or when pregnancies are more than two weeks past the due date, obstetricians and gynecologists say. But sometimes the procedure is done solely for convenience. In a busy society, doctors and patients have grown increasingly comfortable with this practice.
“People want to schedule their birth like they schedule their nail appointments,” says Janie Wilson, director of nursing operations for women and newborns at Intermountain Healthcare, a Salt Lake City-based chain of hospitals that has tried to reduce the rate of labor inductions.
Until recently, few have questioned whether elective labor induction is appropriate. “There is not a unique description of elective labor induction that every single provider can agree on,” Grobman says. Indeed, the practice appears to vary widely among patients, doctors and hospitals. According to the national figures, for example, labor induction for both medical and nonmedical reasons occurs in 25% of white women but in only 18% of black women and 14% of Hispanic women. And a study published in 2003 in the journal Birth found that the percentage of inductions that were elective varied from 12% to 55% among hospitals and from 3% to 76% among individual doctors.
But some experts say the practice creates unnecessary risks and costs. It can lead to more interventions, such as caesarean sections, and increased use of forceps and vacuum devices to assist in delivery, research has shown. A 2005 study in the journal Obstetrics & Gynecology found that C-sections occurred 12% of the time among women having spontaneous labor compared with 23.4% for women having medically necessary labor induction and 23.8% for women having elective labor induction.
Other studies have found that, compared with spontaneous labor, elective induction leads to longer hospital stays and higher costs. Induced labor also may be more painful because some of the drugs administered to trigger labor can cause more intense contractions.
The risks of C-section or other complications appear highest when induction is performed before 39 weeks and in women who have not had a previous vaginal birth.
--
Charting a new course
Now, some hospital administrators are saying, “Enough.” Intermountain Healthcare, which operates 21 hospitals in Utah and Idaho, implemented strict guidelines on elective labor induction eight years ago. Today, the company’s results are held up as a model for reining in birth practices that cannot be medically or financially justified.
The chain, which delivers 53% of all babies in Utah, told its doctors they must seek permission from a supervisor before inducing labor prior to 39 weeks. Doctors must also make sure the cervix is favorable for delivery.
When the cervix is optimal (it must be opened and thinned out enough to allow the baby’s head to pass through the vagina), labor averages about nine hours in a first-time pregnancy, according to Intermountain. If the cervix is not ready, however, an average labor is about 22 hours. The guidelines have reduced rates of elective labor inductions performed before 39 weeks gestation from 28% in 1999 to 3.4% in 2006. The percentage of first-time moms with an elective induction has fallen from 15% in 2003 to 4.7%.
Hospital administrators no longer see sudden spikes in deliveries before major holidays, three-day weekends and Jazz basketball playoff games.
The program has resulted in plunging C-section rates, fewer newborns in intensive care and fewer medical interventions in delivery. Length of labor has decreased by an average of two hours per patient. That’s important, Wilson says, because length of labor is linked to a higher risk of dehydration and infection.
“We feel pretty confident that it does make a difference,” she says.
There is little scientific evidence that labor induction causes any long-lasting harm to mother or baby. But even short-term medical problems are significant given the nation’s healthcare economics crisis, Wilson says. According to Intermountain’s data, healthy deliveries in the 39th week (and women whose cervixes were fully prepared) incur the lowest costs.
“It could be contributing to the double-digit premium increases you pay each year,” she says of elective labor induction’s effect on insurance rates. “Cost is the icing on the cake. But it’s not the main reason we should be doing this. We should do it because it’s safer.”
--
Trend starts to take hold
Other hospitals and provider organizations are also curbing elective labor induction.
Ascension Health Inc., the largest nonprofit healthcare system in the country with facilities in 20 states, last year requested its doctors follow criteria before proceeding with an elective labor induction. The criteria specified that the fetus must be at least 39 weeks in gestational age, in a specific size range and have established lung maturity, and that the mother isn’t already having contractions.
“We don’t discourage elective induction, but there have to be a number of things in place,” says Dr. Robert Welch, chairman and program director of obstetrics and gynecology at Providence Hospital in Southfield, Mich. The goal is not only to reduce C-sections, he says, but to “have zero preventable birth trauma.”
“Some doctors do many elective labor inductions at 38 weeks. But if you do them long enough, eventually you’re going to have a baby with respiratory distress and complications. And that can be very serious.”
Other healthcare organizations and hospitals have applauded the actions taken by Intermountain and Ascension. The Institute for Healthcare Improvement, a nonprofit group based in Cambridge, Mass., that advocates for improved quality in healthcare, and Premier Inc., in Charlotte, N.C., an alliance aimed at improving quality in 1,700 nonprofit hospitals, have also called for lower rates of elective labor induction as a way to reduce harm to infants during childbirth.
Not everyone thinks elective labor induction is harmful. A study published July 31 in the Annals of Family Medicine suggested that “preventive labor induction” may produce the best safety outcomes, including lower C-section rates.
Doctors practicing in a rural Connecticut hospital found that the approach, which includes the use of a mild-acting prostaglandin gel to ripen the cervix before inducing labor, significantly lowered C-section rates compared with women receiving traditional care. Specific criteria were used to determine the “optimal time” for the patient to undergo the preventive induction.
The idea is to perform an induction before the baby gets too big and the placenta can no longer fully support a healthy pregnancy.
If women are carefully selected -- based on an accurate due date, fetal maturity and other risk factors -- induction may produce the best results, says the study’s author, Dr. James M. Nicholson, assistant professor at the University of Pennsylvania Department of Family Medicine and Community Health.
“Over the last two or three years, there is evidence that if you induce when the cervix is favorable, then induction doesn’t cause adverse outcomes like C-sections,” he says.
The method needs more proof, Nicholson says. He is conducting a randomized, controlled trial at the University of Pennsylvania.
“If this is true, it really could change thoughts on how to manage labor in a big way,” he says. “It would lead to all sorts of different research questions: How to induce, when to induce, is race a factor? The questions are numerous.”
--
Calls for more study
Many researchers believe elective labor induction -- like elective C-sections -- should be submitted to more rigorous research on safety outcomes.
Until then, however, interventions that are performed without an obvious medical need should be viewed skeptically, says Dr. Michael C. Klein, emeritus professor of family practice and pediatrics at the University of British Columbia, who wrote an editorial in the same journal calling the study’s conclusions into question.
“Childbirth is complex,” says Klein, who has studied birth outcomes. “What they are doing is complex, but they are not acknowledging it.”
Klein says the lower C-section rates may be due to the especially attentive and intense care the laboring women in the study received -- not because they were induced at an optimal time.
“This is another study saying to women, ‘You can’t survive without us making things better; nature is completely off-track,’ ” says Klein. “And there is a huge reservoir of practitioners out there who want to hear this message.”
Women of childbearing age today also seem to be receptive to the message that a medically managed birth is the best route, says Intermountain’s Wilson.
“We’ve been hammering on this guideline for a long time. It’s hard to get doctors to buy into it,” she says. “Their patients are really putting a lot of pressure on them.”
Despite the lack of research and sometimes conflicting data, women undergoing elective induction should discuss the potential risks and benefits with their doctors, says Wilson.
“I’m not sure consumers think about the risks. They think, ‘Gosh, I want elective induction at 38 weeks because I’m tired of being pregnant,’ ” she says. “Hopefully, educating them up front and setting expectations will make it easier.”
Doctors who want the convenience to schedule daytime deliveries may be the biggest force for elective labor induction, says Lisa Sherwood, a certified nurse midwife and women’s healthcare nurse-practitioner based in San Clemente. Women who “haven’t slept well in weeks, have swollen ankles and sore backs” are vulnerable to the suggestion of elective induction. “People look at the doctor as the expert and will do whatever he or she suggests.”
But, she says, “once you do an intervention, it begets more interventions, and many women feel they are led down a road they didn’t understand. Women tell me, ‘I didn’t know it was going to end up like this.’ Women need to be given all the information on what they are signing up for, not just told, ‘You’re going to have your baby today.’ ”
Hayashi turned to Sherwood this year to deliver her second baby after she was informed -- in the first trimester -- that she would be induced again.
“I think these doctors kind of play bully. They give you the better of two horrible options and say your body can’t do it.”
Her second son was born two weeks after her due date following a spontaneous, four-hour labor.
--
--
(BEGIN TEXT OF INFOBOX)
Labor induction
In less than 15 years, the rate of labor induction among U.S. women has increased 123%. Experts believe many labor inductions are not medically necessary.
1990: 9.5%
1995: 16.0%
2000: 19.9%
2003: 20.6%
2004: 21.2%
Source: National Vital Statistics Reports, Vol. 55, No. 1, Sept. 29, 2006