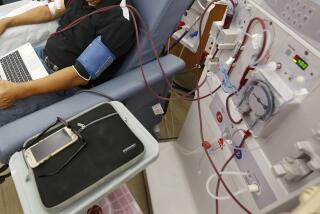
Kidney dialysis on the go
- Share via
People with chronic kidney failure face a bleak future. Conventional dialysis cleanses the blood of only about 17% of the toxic chemicals that a healthy kidney removes. And donor organs are scarce. The 300,000 Americans who depend on dialysis to stay alive are crippled by an array of complications caused by the buildup of dangerous poisons in their blood, and only one-third survive more than five years.
Experimental devices in development could help turn this situation around. One advance, a battery-powered, wearable dialysis machine, would allow users to have their blood cleansed round the clock instead of being hooked up to machines 12 hours a week, potentially improving quality of life and reducing mortality. Even further ahead, blood-filtering systems created via nanotechnology -- engineering on a scale one-billionth the size of a meter -- may prove more effective than current dialysis and may even lead to miniaturized, implantable artificial organs that mimic the continuous function of healthy kidneys.
“There’s been an explosion in innovation in dialysis in the past few years,” says Dr. Allen Nissenson, director of the Dialysis Program at UCLA’s Geffen School of Medicine. “In the not too far future, this new technology could transform the field. . . . If it works, it could improve people’s lives by providing a form of dialysis that is much more like what natural kidneys do.”
--
Round-the-clock treatment
Currently, people suffering from chronic kidney failure must undergo half-day hemodialysis sessions tethered to bulky machines three times a week to have toxic chemicals cleared from their blood. The intensive treatment can be physically and psychologically draining and cause cramps and nausea.
Because their kidneys no longer flush out fluids, patients must restrict their fluid intake. They must avoid foods containing potassium and phosphorous, because their bodies can’t metabolize them properly. Patients also take a fistful of medications every day to help their tissues absorb the scant amount of these minerals their bodies can manage and to stave off the collateral damage of kidney failure such as heart disease, anemia, high blood pressure, osteoporosis, severe joint pain and loss of mental acuity.
“These patients are miserable and not infrequently they tell me, ‘I can’t take it anymore, stop and let me die in peace,’ ” says Dr. Victor Gura, a nephrologist at Cedars-Sinai Medical Center who has invented a wearable artificial kidney, and chief scientific officer at Xcorporeal Inc., the L.A.-based company developing his device.
Growing scientific evidence suggests that increasing the frequency and duration of dialysis treatments could greatly reduce this suffering. But dialysis is expensive, and there are not enough machines or nurses to give everyone daily treatments. “The exponentially increasing number of patients requiring dialysis -- a population that is growing 10% annually -- coupled with the crisis in heathcare funding in the U.S. is putting immense pressure on us to deliver dialysis in a completely different way,” says Dr. William Fissell, a nephrologist at the Cleveland Clinic in Ohio.
A wearable artificial kidney would be an important step toward providing round-the-clock treatment, says Dr. Claudio Ronco, a nephrologist at St. Bortolo Hospital in Vicenza, Italy, who tested Gura’s device in early human trials. “Dialyzing patients continuously with a miniaturized wearable device represents a complete paradigm shift from the way we treat patients today,” Ronco says.
--
How it works
The portable artificial kidney consists of a tiny, double-channeled pulsating pump -- one circulates blood, the other water -- a fluid-collection bag, a filtration system to cleanse impurities and disposable cartridges to purify the water so that it can be recirculated.
The device weighs about 10 pounds, uses about 14 ounces of water and is powered by a 9-volt battery. These components are attached to a belt worn around the waist.
(In contrast, conventional dialysis equipment is the size of a washing machine and requires 40 gallons of water and 110 volts of electricity, which means it must be plugged into an electrical outlet.)
“This is an excellent first step,” says the Cleveland Clinic’s Fissell.
Small pilot studies have been encouraging, the researchers say. Initial tests in May 2006 on six patients in Italy revealed that the device was safe and removed water effectively without complications.
The results of a more recent trial were reported Nov. 3 at the annual meeting of the American Society of Nephrology. Eight patients in London wore the belt for as long as eight hours. The wearable artificial kidney effectively cleansed waste products and excess fluids from the patients’ blood, although at a slower rate than conventional dialysis. “But if we could use this 24/7 or even 18 hours a day, it would be as good or better than daily dialysis, and liberate patients from being tied for huge chunks of time to machines,” Gura says.
The crude prototype used in these tests was constructed with existing equipment off the shelf. But now that they’ve proven the concept works, engineers at Xcorporeal are fabricating a customized version with turbo-charged pumps and more efficient filters that would clear toxins and fluids more rapidly, Gura says. They hope to put all the components together in a streamlined package that weighs about 5 pounds, so that it can be worn comfortably all day.
“We’re still a long way from having an FDA-approved product,” Gura says. “But we’ve demonstrated this is doable.”
--
(BEGIN TEXT OF INFOBOX)
The next generation
Nanotechnology -- precision tooling at the micro-molecular level -- is being used to create the next generation of artificial kidneys, ones that would be small enough to be implanted and engineered to more closely simulate the function of human kidneys than current equipment.
Scientists at Cleveland Clinic’s Lerner Research Institute in Ohio have completed some key initial steps in this process. Employing technology used to make computer chips, they’ve fabricated synthetic membranes with pores engineered to filter the blood with exquisite selectivity: trapping the bad stuff -- toxic metabolic waste products such as urea, plus excess fluids and salts -- without robbing the body of critical proteins and blood cells.
The micro-machining enables researchers to etch precise patterns of pores onto ultra-thin silicon wafers, creating sponge-like filters with more than 10,000 pores per square centimeter.
“The trick is to refine the holes and build a membrane with an easy flow so you don’t need a huge pump,” says Shuvo Roy, a biomedical engineer at the Cleveland Clinic who is involved in this research.
The research is still in the preliminary stages -- researchers are refining the membranes -- but the ultimate goal is to exploit the capabilities of nanotechnology and shrink the filtration and pump system down to the size of a soda can. This would open the pathway toward the development of a truly implantable artificial kidney, one inserted right in the body, much akin to pacemakers. “What we’re aiming for is a quantum leap forward -- a device that would operate 24/7 without human intervention,” says Dr. William Fissell of the Cleveland Clinic, who is also working on this technology.
UCLA researchers also are using nanotechnology to fashion a device that functions more like a normal kidney does. It would have a dual membrane system: one would filter impurities from the blood and the other would reabsorb blood components that are needed, then excrete the rest as urine, as flesh-and-blood kidneys do. “By mimicking nature, we have the best chance of getting the best outcome,” says nephrologist Dr. Allen Nissenson, director of the Dialysis Program at UCLA. “It’s still very early, but so far so good.”
-- Linda Marsa