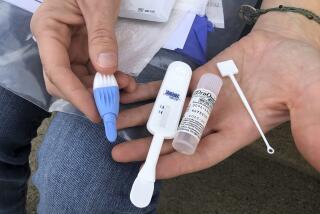
Older but wiser? Safe sex after 50
- Share via
KANSAS CITY, MO. — Jane Fowler thinks it’s about time college students had “the talk” with their grandparents.
She doesn’t mean grandmothers and grandfathers explaining the facts of life. She wants kids to explain safe sex to their elders.
It’s part of a broader message the 72-year-old has advocated for more than a decade. Ever since she contracted HIV when she was in her 50s, Fowler has made it her mission to help aging baby boomers and members of her generation avoid her mistakes.
“Once people get past their own embarrassment and understand grandparents today are still sexually active, they realize I’m right,” said Fowler, who is scheduled to speak at a safe-sex event on the Kansas State University campus today. “Their grandparents face the same risks of sexually transmitted diseases as they do.”
The over-50 crowd is a relatively small segment of the nation’s at-risk group for sexually transmitted diseases. Approximately four times as many HIV diagnoses occurred in people ages 25 to 44 as in those 50 and older, according to a 2005 report by the Centers for Disease Control and Prevention.
Still, medical experts agree that older Americans often are among the most overlooked -- and therefore one of the more vulnerable -- populations.
They point out that the majority of funding for preventive education over the last two decades has been aimed at the traditional high-risk populations such as teens, gays and urban residents. (Others, however, note that many baby boomers were young enough when the public first became aware of the AIDS crisis that they should have gotten plenty of exposure to safe-sex campaigns.)
In addition, many older patients feel uneasy discussing sexual behaviors with their physicians, according to AARP research. Doctors too can be uncomfortable talking about STD risks with people old enough to be their parents or grandparents, according to a recent study backed by the National Institutes of Health.
Considering that people now are living longer than previous generations have, and enjoying extended sex lives because of hormone therapy and erectile dysfunction drugs, there’s a growing concern that the baby boom generation -- and their elders -- don’t understand that getting older doesn’t make one immune.
That concern is fueling a national push among public health officials and educators for more prevention efforts aimed at aging baby boomers and those who are firmly in their golden years.
In Arizona, volunteers regularly have passed out free condoms at community centers, and state health workers in Florida host safe-sex programs in retirement communities. In Broward County, Fla., the Senior HIV Intervention Project recruits retired boomers and older residents throughout the region to become “safe-sexperts” who can convince their neighbors to get tested for STDs.
At the University of Michigan Health System, enough patients were concerned about the impact of aging on intimacy that a clinic was opened in Ann Arbor last year devoted to dealing with the sexual concerns of the 60-and-older crowd. And in Ohio, professor Nancy Orel and staff at Bowling Green State University have preached about the risks of casual sex and offered free HIV tests at a workshop targeting “boomers and beyond.”
Orel sells the idea of using condoms and getting tested for HIV as part of serving as a role model for their younger loved ones.
But to the undergraduate students taking her gerontology classes at Bowling Green, the roles are reversed. One of the assignments Orel gives is for students to go home, find out what their grandparents know about HIV and discuss safe sex practices.
“Initially, some of the students are hesitant. But a lot of them are surprised at how open the conversations can be,” said Orel, director of the university’s gerontology department.
A study published last summer in the New England Journal of Medicine reported that a majority of 3,005 American adults surveyed, aged 57 to 85, continued to have sex two to three times each month.
But only 38% of the men and 22% of the women had discussed sex with a doctor since they turned 50, according to the report funded by the National Institutes of Health.
Edward O. Laumann -- a professor at the University of Chicago who studies human sexuality and is one of the study’s authors -- said older Americans should know better than to have unprotected sex. When the HIV/AIDS epidemic started, he pointed out, many of them were young enough to have been bombarded by public education efforts.
“I’m not saying there aren’t randy goats in a nursing home somewhere, who might have [STDs] and spread [them],” Laumann said. “But educating them isn’t going to affect anything . . . and it’s a waste of money, particularly when there’s other vulnerable groups that need the resources anyway.”
Part of the problem with figuring out exactly what risks older Americans face comes from a lack of testing data, said Spencer Lieb, senior epidemiologist at the Bureau of HIV/AIDS at the Florida Department of Health.
He noted that although the number of HIV and AIDS patients in the over-50 crowd nationwide had grown in recent years, some of the increase was attributed to people who are living longer with the virus or disease, thanks to improvements in therapy treatments.
But without widespread testing, “we don’t really know what the true prevalence [of STD infection] is in this group,” Lieb said. “There’s reason to think, at least anecdotally, this is a combustible situation that is being overlooked.”
That’s why some social service and public health officials have turned to HIV-positive patients like Fowler to speak out and try to get their peers’ attention.
Just outside a small classroom, at the back of a St. Louis community center, Fowler recently met up with a graying group to commiserate about sexually transmitted diseases, and recounted her cautionary tale. How a divorce in her 50s led her back into the dating pool, and how she enjoyed a New Year’s Eve fling with a former co-worker. Fowler said she never considered using condoms, given that she had already gone through menopause.
“I had lived what I considered a conventional, traditional life. I had been a virgin on my wedding night in 1959,” said Fowler, a founder of the National Assn. on HIV Over Fifty, who now coordinates the speakers bureau at a local AIDS organization. She has spoken before hundreds of groups over the years, including medical researchers and HIV/AIDS advocates to senior centers.
“I remained monogamous for 23 years of marriage. . . . After the divorce, I didn’t consider myself promiscuous. I didn’t frequent the singles bars. I went out with men my age who, like me, had been married and were divorced.”
Her own physician, she said, dismissed her questions about getting tested for HIV as unnecessary for someone her age. Her early symptoms were dismissed as routine ailments of aging.
“I visited [my doctor] five times, complaining of intermittent low-grade fevers, headaches, nasal congestion, a sore throat, a rash, bronchitis, aches in my arms and legs,” Fowler said. “She didn’t think HIV. Neither did I.”
Sitting in rows of plastic folding chairs, the small crowd of two dozen nodded in understanding. The group of casually dressed men and women were black and white, straight and gay. All were older than 50. All had HIV.
No one wanted to give his or her name. A 68-year-old widower who contracted HIV three years ago confessed that he had been too embarrassed to talk to his doctor about his symptoms. Across the room, a 62-year-old retired teacher said she never thought of using a condom -- she too had been through menopause and was not concerned about getting pregnant.
“None of my friends think about these things, let alone talks about them. Condoms? Testing?” the woman later confided to Fowler. “At my age, the worst I thought could happen was a broken heart.”
--