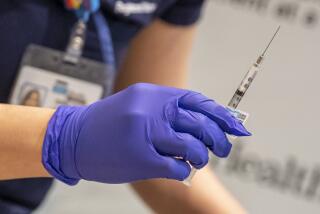
HIV drugs to be tested as protection
- Share via
Disheartened by the failures of vaccines and microbicides in blocking HIV transmission, some AIDS researchers are now touting a third possibility: using existing HIV drugs prophylactically.
By next year, as many as 15,000 people worldwide will be enrolled in trials to test the concept -- more than are enrolled in all vaccine and microbicide trials combined -- according to a report issued Sunday at the International AIDS Conference in Mexico City. There are seven trials underway or planned.
“We need to look for new ways that people can protect themselves,” said Dr. Lynn Paxton of the U.S. Centers for Disease Control and Prevention, who is coordinating the agency’s trials. “Clearly, this is one of the most promising things we have in the pipeline right now.”
Some results are expected to be available next year.
“We don’t know if this is going to work or not, but we must get it on the agenda,” said Mitchell Warren, executive director of the AIDS Vaccine Advocacy Coalition, which prepared the Mexico City report. “We must be prepared for the answers we do get.”
The concept, called Pre-Exposure Prophylaxis, or PrEP, is relatively simple: Take a drug used to treat HIV infections and give it daily to people at risk of contracting the virus in order to block infections.
A similar approach is now used routinely for people who are going into areas where malaria or tuberculosis are endemic and for AIDS patients who are at risk of pneumocystis pneumonia.
AIDS drugs are also used to block mother-to-child transmission during birth or breast-feeding and for post-exposure prophylaxis, such as when a laboratory worker is accidentally stuck with a contaminated needle or when a nurse or emergency technician is exposed to HIV-positive blood.
“In all those circumstances, it works,” Paxton said. “The logical extension is to think about it for prevention of sexual or injection-drug transmission.”
Researchers have been arguing for PrEP for years, she said.
“The only thing that held us back is we didn’t have any drugs amenable to that. We need very low side effects and a high barrier to development of resistance,” she said. “It wasn’t until Truvada came down the pipe that we had the pills to test it.”
Truvada, manufactured by Gilead Sciences Inc. of Foster City in Northern California, is a combination of tenofovir and emtricitabine, drugs in a class known as non-nucleoside reverse transcriptase inhibitors, which block an enzyme necessary for HIV replication. Truvada is being used in many of the studies. The rest of the trials are using only tenofovir, which is trade-named Viread by Gilead.
Animal studies have suggested that the approach will work. An early study of tenofovir, for example, showed that it prevented monkeys from getting SIV, the monkey form of the AIDS virus.
“But animals are not people, so we don’t know if it will work until we conduct clinical trials,” Warren said.
The seven such trials are sponsored by the CDC, the National Institutes of Health and the Bill & Melinda Gates Foundation.
Dr. Robert Grant of UC San Francisco is leading one trial that will enroll 3,000 HIV-negative gay men in Peru, Ecuador and the United States. Half will receive Truvada daily and half a placebo.
The men will be followed through the end of 2010, and Grant hopes to see at least a 60% reduction in infections among men receiving the drug. “If the efficacy is at that level or higher, intervention would be cost-effective in very high-risk populations,” he said.
One risk of the trials is that continued use of the drugs by people who become infected without realizing it could lead to drug resistance, limiting treatment options for those people.
Critics have also argued that the availability of the drug might lead recipients to engage in riskier behavior. That has not happened so far, Grant said.
In fact, the prevention counseling that the studies provide to all participants has lowered the incidence of risky behavior -- paradoxically making it harder to prove the value of the drugs because there are fewer infections even among those receiving placebos.
That is why the trials require large numbers of participants, Grant said.
Even though results will not be available until next year, the Mexico City report called on researchers to begin making plans for use of PrEP, just as plans were made for the wide-scale implementation of circumcision even before reports showed that it would help limit HIV transmission.
“We cannot wait for the study results to begin to prepare for the optimal use and delivery of PrEP,” said Pedro Goicochea of the Lima-based nongovernmental health organization Impacta, who heads one of the studies.
“Instead, we should look ahead to consider all the possible outcomes of the trials and make real plans for making PrEP available to those who can benefit from it, as quickly and as safely as possible if it is proven effective.”
Researchers have not given up on a vaccine.
“We all support vaccines,” Grant said. “They are ultimately easier to implement than a pill a day. The problem is that there is no guarantee there will ever be a vaccine against HIV. . . . We hope there will be a vaccine, but in the meantime, PrEP is a concept that should be evaluated thoroughly.”
--
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.