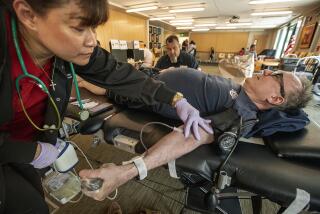
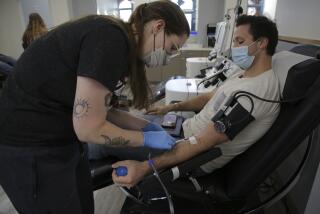
Every drop counts
- Share via
For some Americans, most notably Jehovah’s Witnesses, the issue of transfusions has always been clear-cut: Their religious beliefs prohibit the use of blood products under any circumstances -- even life-saving ones. Others would simply prefer to avoid transfusions for safety or personal reasons.
Now, a growing number of hospitals are catering to both types of patients.
In the last decade, hospitals across the country have opened “bloodless,” or “transfusion-free,” medicine programs. Currently, almost 125 hospitals have established programs; in 1994, only about 35 did, according to the Bloodless Medicine and Surgery Institute, a private educational organization for medical professionals interested in blood conservation.
The approach appeals to far more than Jehovah’s Witnesses. “Many patients know that transfusions carry risks that they simply don’t want to incur,” says Dr. Leo Orr, co-director of the transfusion-free program at Good Samaritan Hospital in Los Angeles, one of the few hospitals in the area to offer this type of medicine. Orr estimates that almost 20% of the patients participating in his program are not Jehovah’s Witnesses.
Bloodless programs employ a variety of techniques to minimize blood loss before, during and after treatments for many illnesses -- all in the hopes of avoiding the need for transfusions. Some are extraordinarily simple, such as collecting smaller-than-usual samples of blood for testing. Others involve the use of innovative medications, such as the hormone erythropoietin, which stimulates the bone marrow to produce red blood cells.
In the operating room, physicians use sophisticated surgical instruments such as a harmonic scalpel, which simultaneously cuts tissues and stops bleeding, and pay meticulous attention to surgical technique. They also use special surgical sealants and glues to control minor bleeding, and drugs such as tranexamic acid to help blood clot normally. Blood that is spilled during surgery often is collected, cleaned and returned to the patient using high-tech systems.
--
Dangers and fears
Advocates of bloodless medicine think that avoiding transfusions is worth all this effort, pointing to the dangers associated with transfusions. Minor allergic reactions are among the most common side effects. But, infrequently, incompatibilities between the donor and recipient trigger more serious reactions.
For example, when patients are mistakenly given the wrong type of blood, their immune systems attack the newly transfused red blood cells, with potentially devastating consequences. Within several hours of the transfusion, these patients sometimes become severely short of breath, and their lungs fill with fluid. This syndrome, called transfusion-related acute lung injury, or TRALI, is the leading cause of transfusion-related deaths (about 24 per year) in the U.S.
The threat of contracting an infectious illness, however, is what many patients worry about most. Donors infected with viruses such as hepatitis or HIV, or parasites such as those that cause malaria, can transmit these illnesses to the patients who receive their blood.
Transfusion experts say such dangers are sometimes overstated. “We’ve gone to extremes to ensure the safety of the blood supply,” says Dr. Alyssa Ziman, medical director of transfusion medicine at UCLA Medical Center. “It’s not cost-effective, but the community demands it.” To minimize the risk of infectious diseases, potential donors and the blood supply itself are aggressively screened and tested. According to the National Heart, Lung and Blood Institute, the risk of getting HIV or hepatitis C from a transfusion is about 1 in 2 million transfusions; the risk of exposure to hepatitis B is higher, approximately 1 in 205,000.
Proponents of bloodless medicine argue their case from another angle as well. They think that avoiding transfusions improves outcomes, and they insist that transfusion-free patients recover more quickly and experience fewer complications than those who receive blood.
Not everyone agrees with this point of view, however. Many experts in transfusion medicine acknowledge that some patients may do well with a low blood count and bloodless measures, but point out that others might not. A young person in good health, for example, might tolerate a significant drop in blood cell count and bounce back more quickly if transfusion is avoided. For an elderly patient with underlying heart disease, avoiding a transfusion could be catastrophic.
--
Complex calculation
Cost comparisons are difficult. “The studies have tended to look only at the cost of blood products,” Ziman says. “I’m unaware of any studies that look at all of the elements.” In the end, costs will depend on the procedure -- a major surgery may wind up costing more with the bloodless approach because of all the technology and expertise required; simply riding out mild to moderate anemia in a medical patient, however, would cost less than a transfusion.
The medical community has adopted a relatively conservative approach to transfusions. “Transfusion practices changed when HIV became a big issue,” Ziman says. Although they’ve relaxed a bit since a screening test for the virus was developed, most physicians are not as quick to transfuse patients as they once were.
“We’re not advocating that people don’t use blood at all, but we are trying to use less blood through more appropriate transfusion practices,” Ziman says. “We try to balance the risks of transfusion with the benefits it offers.”
Although a bloodless approach may be the only acceptable option for Jehovah’s Witnesses, there might be a more appropriate middle ground for most people. It’s one thing to take reasonable measures to try to steer clear of transfusions; it’s another thing entirely to risk your life in order to avoid receiving blood.
As for the bloodless medicine programs themselves, in many cases they may actually be more hype than substance. Many of their techniques have now become mainstream and are implemented by most hospitals. Instead of seeing bloodless medicine programs at a few hospitals, blood conservation should be a priority at all of them.
“Bloodless is a term we’re trying to move away from,” says Dr. John Waters, medical director for the preoperative blood management program at the University of Pittsburgh. “Blood management is a more all encompassing term.”
--
Dr. Valerie Ulene is a board-certified specialist in preventive medicine practicing in Los Angeles. She can be reached at themd@att.net. The M.D. appears the first Monday of the month.
--
(BEGIN TEXT OF INFOBOX)Blood’s oxygen carrier
Hemoglobin, a component of red blood cells, carries oxygen to tissues throughout the body. When hemoglobin levels drop very low -- from blood loss or iron deficiency, for example -- tissues don’t receive adequate amounts of oxygen. Deprived of oxygen, they might not be able to function properly and, in some cases, could be permanently damaged.
In the past, many physicians would automatically transfuse patients if their hemoglobin fell beneath a certain level. Experts in bloodless medicine point out that the body is able to accommodate fairly significant drops in hemoglobin. As levels fall, the body compensates in a variety of ways such as increasing the heart rate and pumping more blood to the tissues.
However, a hemoglobin level that may be perfectly safe for one person could be too low for someone else. For this reason, doctors now look at more than just hemoglobin levels when trying to determine if a transfusion is necessary. A patient who is experiencing symptoms of their low blood count -- such as a rapid heart rate -- is more likely to require a transfusion than someone who is not.
-- Valerie Ulene