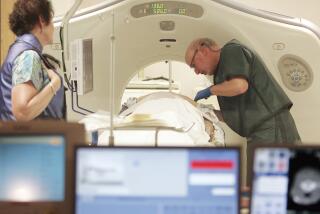
Cancer exams get political
- Share via
NEWARK, DEL. — With soothing walls of turquoise tile and a vase of orchids on the front desk, the Colon Health Center of Delaware has been selling an alternative to one of medicine’s most unloved procedures -- the colonoscopy.
Rather than insert several feet of tubing into patients’ lower intestines, clinicians slide patients into a computed tomography, or CT, imaging machine that can quickly scan the abdomen for signs of cancer.
Today, however, this procedure is the subject of a heated debate in Washington pitting powerful sectors of the healthcare industry against a government desperate to contain healthcare spending.
The fight over virtual colonoscopy has also become a prime example of how hard it can be to ensure that healthcare dollars are spent efficiently, a key goal of the Obama administration.
The procedure is cheaper and more comfortable than the traditional method. Proponents say the noninvasive approach will save lives by increasing the number of people who get screened. Around 50,000 people die every year from colorectal cancer, many because they avoided a traditional colonoscopy.
But there is still no consensus about the effectiveness of the new procedure. Some critics contend it could inflate the nation’s skyrocketing healthcare tab because a traditional colonoscopy is required if anything is found in the imaging.
Federal officials are now deciding if Medicare should cover virtual colonoscopy for millions of senior citizens, a determination that could have consequences for all consumers, as well as doctors, hospitals and medical equipment makers. The decision is expected next month.
“This may be a bellwether for how the hard choices around expanding access and controlling costs will play out,” said Dr. Sean Tunis, who was chief medical officer at the Centers for Medicare and Medicaid Services in the last Bush administration.
Colorectal cancer is highly treatable if detected early, but it remains the nation’s second deadliest cancer, in large part because half of adults over 50 do not get screened.
For years, the most reliable screening method has been optical colonoscopy, in which an endoscope is used to inspect the walls of the intestine and remove abnormal growths, or polyps. But many people shy away from getting screened because they don’t want to be sedated, as is sometimes necessary, or prodded by a tube inserted through the rectum.
Rosemarie Blair was such a person. “I don’t like operations or needles or anything too invasive,” the 60-year-old legal assistant from Delaware said.
But, prompted by the death of a friend’s daughter last Christmas, Blair made an appointment to get a virtual colonoscopy.
The procedure, which produces a three-dimensional image of the patient’s lower intestine, can still be unpleasant. As with a normal colonoscopy, patients must drink large quantities of unpalatable liquids to cleanse their bowels. Before the scan, air is injected into the lower intestine, a process that can be uncomfortable.
Blair’s scan identified two polyps that were removed that morning by a gastroenterologist using traditional colonoscopy. The scan also picked up something suspicious in Blair’s right kidney.
Follow-up tests identified a small cancer. Last month, Blair had the kidney removed.
Stories like Blair’s have fueled enthusiasm for wider use of virtual colonoscopies. Last year, the American Cancer Society added the procedure to its list of recommended screening options.
Also backing the new procedure is the medical imaging industry, which by one estimate reached $7.8 billion in sales in 2007, and healthcare providers eager to use their CT scanners.
Like many new medical technologies, however, virtual colonoscopy poses a challenge for Washington policymakers.
Medicare, which will spend more than $500 billion this year, is under increasing pressure to contain spending that many experts say threatens the whole federal budget.
Of particular concern has been the rising cost of scans. Medicare spent more than $14 billion on imaging in 2006, double what it spent six years earlier, according to a 2008 report by the Government Accountability Office.
Many experts believe cutting ineffective or wasteful procedures will be key to controlling healthcare spending.
The federal government has attempted to do that in part by carefully evaluating new technologies before Medicare agrees to pay for them.
In an extensive, year-long, review of virtual colonoscopy, Medicare officials scoured medical journals, convened doctors and health policy experts and reviewed more than 400 opinions submitted in two public comment periods.
Though many urged Medicare to cover virtual colonoscopies, others counseled caution.
“You have to be really, really careful when it comes to preventive services because you are starting with asymptomatic people who appear to be healthy,” said Dr. David Shih, senior director of medical affairs at the American College of Preventive Medicine.
Some studies have indicated that the procedure can detect most polyps as well as traditional colonoscopy. But others have suggested it is not be as good at detecting some smaller polyps.
Disputes over the cost-effectiveness of virtual colonoscopy further complicated the analysis.
The procedure, which typically costs less than $1,000, can be half as expensive as a traditional colonoscopy. But some 20% of patients will have a polyp requiring a follow-up optical colonoscopy to have the growth removed. That has led to criticism that virtual colonoscopy is duplicative.
On Feb. 11, the federal agency drew a simple conclusion: “The evidence is inadequate.” It recommended Medicare not cover virtual colonoscopy.
The move sparked an immediate backlash.
“There are those who believe we have to have absolute gold-plated evidence to OK a procedure,” said Dr. Len Lichtenfeld, deputy chief medical officer at the American Cancer Society. “But the fact is that we are not getting the job done when it comes to colorectal screening. . . . We have an obligation to give the benefit of the doubt to Medicare beneficiaries.”
Working with a Washington lobbying and public affairs firm, interest groups organized a briefing last month for lawmakers in the Capitol.
More than 50 members of Congress mounted a letter-writing campaign to the Medicare agency.
To some health policy experts, that kind of political pressure is one of the reasons the nation’s healthcare system has become so inefficient. Few expect it change, however. .
“The issue is: Who is going to make the decisions about what we do and what we don’t do in medicine,” Lichtenfeld said. “Let’s not kid ourselves: That is a political question.”
--