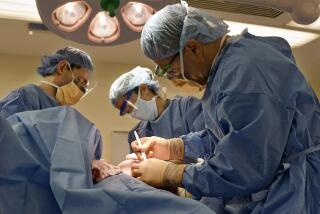
Studies find spinal procedure no more effective than placebo
- Share via
A widely used surgical procedure in which cement is used to fortify cracks in the spine is no better than a sham operation, two groups of researchers independently reported Wednesday in the New England Journal of Medicine.
The findings shocked clinicians because the procedure, first introduced in the early 1990s, is now widely accepted and assumed to be very effective at relieving pain and improving mobility. About 80,000 such procedures, called vertebroplasties, are performed in the United States each year, primarily in the elderly. The total has doubled in the last six years.
The spinal cracks typically are a result of thinning of the bones caused by osteoporosis. The operation typically costs as much as $3,000, although Medicare pays only about two-thirds that amount.
The procedure is so widely accepted that researchers had a hard time enrolling patients in the clinical trial because patients feared being placed in the placebo group.
The findings come at a time when President Obama has been calling for increased use of comparative effectiveness research, in which medical procedures are tested against one another to determine which is best or most cost-effective. The findings should provide powerful support for increased testing, Dr. James N. Weinstein of Dartmouth Medical School in Hanover, N.H., wrote in an editorial accompanying the reports.
In one of the new studies, supported primarily by the National Institutes of Health, Dr. David F. Kallmes of the Mayo Clinic -- one of the originators of the procedure -- and his colleagues enrolled 131 patients; 68 received a vertebroplasty, and 61 received a sham procedure in which the back was numbed, surgeons pressed on it as if they were injecting cement, and the patients were exposed to the distinctive odor of the cement.
Both groups of patients reported a significant reduction in pain and improvements in quality of life and functional status during the follow-up period.
Epidemiologist Rachelle Buchbinder of Monash University in Australia and her colleagues performed a similar study on 71 patients, with identical results. That study was funded by the Australian government and an American company that manufactures the cement. Buchbinder received a grant from the company for conducting the study.
Kallmes suspects that the improvement in pain may have come from prolonged effects from the drugs that were used to numb the back in both groups. He is beginning a second trial to test the benefits of such numbing.
It is also possible that many or all of the benefits derive from a placebo effect -- simply from patients’ perceptions that something is being done for them.
Despite the disappointing findings, surgeons are unlikely to stop performing the procedure any time soon because it does relieve pain, even if it is through a placebo effect, said Dr. Ty Thaiyananthan, a spinal surgeon at Chapman Medical Center in Orange.
“But it changes the way we will do an informed consent,” he said, because patients must now be told about the similar benefits of sham surgery.
--