Select health, not eye color
- Share via
Something stinks about reproductive medicine in Southern California, and it doesn’t involve eight dirty diapers.
Recently, the Los Angeles-based Fertility Institutes announced that it would soon be offering patients at its clinics the chance to choose traits such as “eye color, hair color and complexion.” The clinics already offer gender selection to patients undergoing in vitro fertilization.
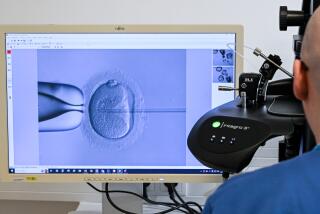
The Fertility Institutes employs a technique known as “preimplantation genetic diagnosis,” which allows doctors to screen embryos soon after they are created in a petri dish and implant only the ones that meet certain criteria. The technique was invented to help high-risk families avoid or manage potentially deadly genetic traits, and to help women who’ve had multiple miscarriages conceive babies they can carry to term.
Now the Fertility Institutes is corrupting this lifesaving clinical procedure by using it to help families create designer babies, and I worry that their excesses will turn public sentiment against all preimplantation genetic diagnosis. That would be wrong.
My son, Henry, was born with a rare and fatal genetic disease, Fanconi anemia. Fanconi patients are born with faulty immune systems and a host of health problems. They are at high risk for leukemia and other deadly diseases and usually die before the age of 30. The only hope is a bone marrow transplant that replaces the immune systems they are born with. The transplants are most likely to succeed if the donor is a sibling who is a perfect genetic match.
My wife, Laurie, and I had always planned to have more children, and in the late 1990s we decided to try to employ preimplantation genetic diagnosis in an attempt to conceive a baby free of the deadly disease who would be a perfectly matched cord-blood donor for Henry. Cord blood is usually disposed of after birth, and harvesting it causes no problems or discomfort for a baby.
We were among the first families attempting the technique, but after three years of trying unsuccessfully, we ran out of time. Henry’s health was deteriorating, and he needed an immediate transplant, which he got from an unrelated donor. Ultimately, his body rejected it. In December 2002, he died at the age of 7.
In the decade since we first tried to conceive using embryo screening, the technology has improved and has saved many lives. I get letters and e-mails with regularity from other Fanconi anemia families who were able to conceive babies who saved their siblings’ lives.
But not all Fanconi families are lucky enough to live in the United States, where preimplantation genetic diagnosis is legal. The regulation and availability of the technique in the European Union is a patchwork, and some countries ban the practice outright.
I understand that there are ethical issues surrounding the procedure. Not all families are comfortable with creating embryos in the laboratory knowing that some of them will be discarded. And no one would advocate creating a child who is only wanted to save another’s life. But the choice of whether to employ screening is a deeply personal one and should be considered with great care by families in consultation with their doctors and genetic counselors.
What I now fear, though, is that clinics offering trait selection to satisfy the whims of parents will turn people against a procedure that can save lives.
Henry was among the most optimistic, wise and courageous people I have ever met. We felt a great responsibility to do everything in our power to save his life. In the end, that wasn’t possible. But our efforts contributed to scientific knowledge, and for that we are grateful. Abusing that hard-won knowledge to capriciously choose hair color, eye color and other cosmetic traits in a baby is wrong and repugnant.