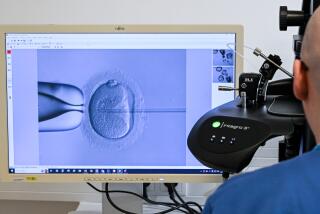
1 in vitro embryo may be best
- Share via
When couples with fertility problems turn to in vitro fertilization, they often assume that they can double their chances for a healthy baby by transferring two embryos to the womb instead of just one.
But data published in today’s edition of the New England Journal of Medicine show that what they’re really doing is increasing their odds of having twins -- which is riskier for the mother and babies alike.
In the early days of in vitro fertilization, doctors routinely transferred half a dozen embryos, or more, to boost the odds that at least one would grow into a healthy fetus. As the treatment improved, doctors were able to get better results using fewer embryos.
Debate lingers about the pros and cons of transferring two embryos instead of one. Pregnancies involving multiples come with a greater risk of gestational diabetes, bleeding and preeclampsia for the mother, and cerebral palsy, birth defects, developmental delays and death for the babies. Twins usually survive, but incur higher medical expenses in the first five years of life.
A team of Swedish researchers is trying to assess the optimum number of embryos to transfer. In their study of 661 IVF patients, 331 women got two embryos, and 142 of them (or 43%) had live births. The other 330 women got a single embryo, and if that didn’t work, they made a second attempt. Of these women, 128 (or 39%) had live births.
The difference between 43% and 39% wasn’t statistically significant. But one-third of the patients in the double-embryo group had twins or triplets, compared with only 1% in the single-embryo group. Those results were published in 2004. Researchers continued to follow the 661 patients. Their conclusion, in the latest issue of the journal: There’s little downside and plenty of upside to transferring one embryo at a time instead of two.
--