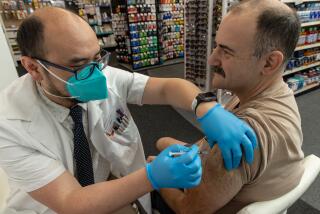
Column: Should we pay women to donate their eggs for research? No, and here’s why.
- Share via
“Not everything in life is for sale, nor should it be.”
That’s what California Gov. Jerry Brown said in 2013 when he vetoed a bill allowing women to be paid to donate their eggs for scientific research.
“In medical procedures of this kind,” he added, “the long-term risks are not adequately known. Putting thousands of dollars on the table only compounds the problem.”
But bad ideas don’t always die in Sacramento; they just hibernate. The proposal to repeal a 2006 ban on any payment beyond reimbursement for time and travel expenses is back this year, with barely a single word changed from the 2013 measure. Passed by the Assembly in April by a 65-3 vote, it will be taken up by the Senate after lawmakers return from vacation next month.
Not everything in life is for sale, nor should it be.
— Gov. Jerry Brown
Its sponsor, the Alabama-based American Society for Reproductive Medicine, evidently hopes that Brown will sign the same measure he already vetoed once. Let’s hope the ASRM is wrong, because this is a bill that could harm women, and its main motivation seems to be profit.
“The ASRM is aggressively trying to expand the market without due concern for what donors want, which is more research and more oversight of the potential health consequences of egg donations,” says Raquel Cool, co-founder of the advocacy group We Are Egg Donors.
Cool is right: There is scant research on the long-term health risks of egg retrieval, and nothing in the bill that would encourage more. To paper over that fact, the measure’s advocates have engaged in a neat bit of obfuscation. Assemblywoman Autumn Burke (D-Marina del Rey), who is carrying the bill for the ASRM, labels it a “pay equity” bill.
“It’s perfectly legal for a woman to get paid when advertising through Craigslist to provide eggs for infertile couples, but she can’t get paid for a donation in medical research,” she said when she introduced the measure in February. That’s “insulting to women,” Burke said, because it “assumes women shouldn’t be allowed to make their own decisions.”
But it’s not about equity or discrimination. What worries the bill’s critics is that the measure may allow women to be misled into taking uninformed health risks by the prospect of easy cash.
Major scientific institutions, including the National Academy of Sciences and the California Institute for Regenerative Medicine, the state’s stem cell program, oppose compensation for donors of eggs used in research, beyond reimbursement for actual expenses and care for immediate complications. Let’s see why.
Unlike sperm collection from males, harvesting eggs from women involves hormonal therapy and invasive surgery. Donors spend weeks getting injected with drugs to stimulate the production and release of dozens of eggs at a time. A physician ultimately collects the eggs from the ovaries by a needle while the woman is under general anesthesia.
The procedure carries short-term complications as well as long-term risks that haven’t been thoroughly studied. Because fertility treatments have been in use only since the 1980s, relatively few women who have donated eggs have reached menopause, when cancer or other long-term consequences might show up. One known complication is ovarian hyper-stimulation syndrome, which at its worst can cause organ damage, kidney failure, or even death, according to the Berkeley-based Center for Genetics and Society, a critic of the Burke bill.
Legislatures tend to act as though such risks are balanced by the benefits of fertility treatments. “The policy argument about helping someone have a child is compelling,” says former state Sen. Deborah Ortiz, who sponsored the ban on paying for research egg donations that’s targeted by the new measure.
Federal and state governments are indulgent about allowing compensation for women who donate eggs for others’ fertility treatments. The field is self-regulated by professional groups, but the rules are vague and easily ignored. ASRM guidelines say payments of $5,000 to donors “require justification” and those over $10,000 are “not appropriate,” and that pay shouldn’t reflect “the donor’s ethnic or other personal characteristics.”
In reality, recruiters have been known to offer $50,000 or more to women with elite academic backgrounds, artistic or athletic skills, or conventionally desirable physical features.
Egg donations for scientific research are different, however. The physical or social characteristics of the donors aren’t as important, so recruiters can cast a wider net, potentially attracting women with greater need for compensation and less inclination to ponder long-term health risks.
Reputable research institutions comply with certain standards to protect human research subjects—the subjects must give their “informed consent” to being experimented upon and can be paid a nominal sum. Sometimes they’re participating in research for their own benefit—testing a drug for their medical condition, for instance.
Yet as David Magnus and Mildred K. Cho of Stanford observed in a 2005 article in Science, egg donors don’t fit into the usual categories of research subjects. They’re not patients, nor are they research subjects. “In a typical research trial, a drug or procedure requires close monitoring of the participant,” says Lisa Ikemoto, a bioethicist at UC Davis law school. “Here, women undergo a procedure and the focus immediately shifts to their eggs. There’s no guarantee of follow-up for them.”
Proponents of paying for research eggs say enough is known to regard egg retrieval as safe. “We have 6 million babies and 30 years of experience,” says Sean Tipton, a spokesman for ASRM. He acknowledges that “there haven’t been specific studies about long-term effects,” but says some studies have followed subjects for 20 years without documenting a link between egg retrieval and cancer.
Yet 20 years may not be enough to judge the long-term effects of tampering with women’s reproductive systems and hormones early in their lives. There are also reports that agencies and doctors who recruit egg donors minimize the immediate complications. “Women are typically told that the rate is less than 1%,” says Diane Tober of UC San Francisco, who is conducting a study of egg donors. The ratio of donors in her sample whose complications required medical care ranging from days or weeks of bed rest to inpatient hospital admission is closer to 30%, she says.
Some experts also question whether even paying for eggs for fertility treatment is ethical. “The equity argument assumes that pay for the fertility market is somehow natural,” says Ikemoto. But the fertility treatment market has been estimated at $5 billion a year. ASRM’s member roster includes fertility clinics along with fertility drug makers.
Increasing the potential compensation for research donors and thus stepping up recruitment, Ikemoto says, “represents an opportunity to expand the business.”
It’s conceivable that paying more for egg donations for research is justifiable, but premature. Before the rules are liberalized, there needs to be more data.
“We’ve been calling for long-term studies for 15 years now,” says Marcy Darnovsky, executive director of the Center for Genetics and Society. “Meanwhile, millions of women have undergone this procedure. We need to know what the risks are.”
Keep up to date with Michael Hiltzik. Follow @hiltzikm on Twitter, see his Facebook page, or email michael.hiltzik@latimes.com.
Return to Michael Hiltzik’s blog.