
- Share via
SAN DIEGO — On a foggy night in mid-March, several family members from the Mexican state of Michoacán followed smugglers’ instructions to climb the first of two border barriers to reach U.S. soil near San Diego.
One of the women felt her grip slipping on the first fence from the moisture in the air as she struggled over. When she approached the second wall, looming 30 feet above her, she realized it would be impossible for her to get over safely. As she panicked, the smugglers told her to wait to the side for Border Patrol to get her so that other migrants could cross.
It was only after she reached the Border Patrol station that she learned that her 14-year-old daughter, whom the smugglers sent with an earlier group, had fallen from the 30-foot wall.
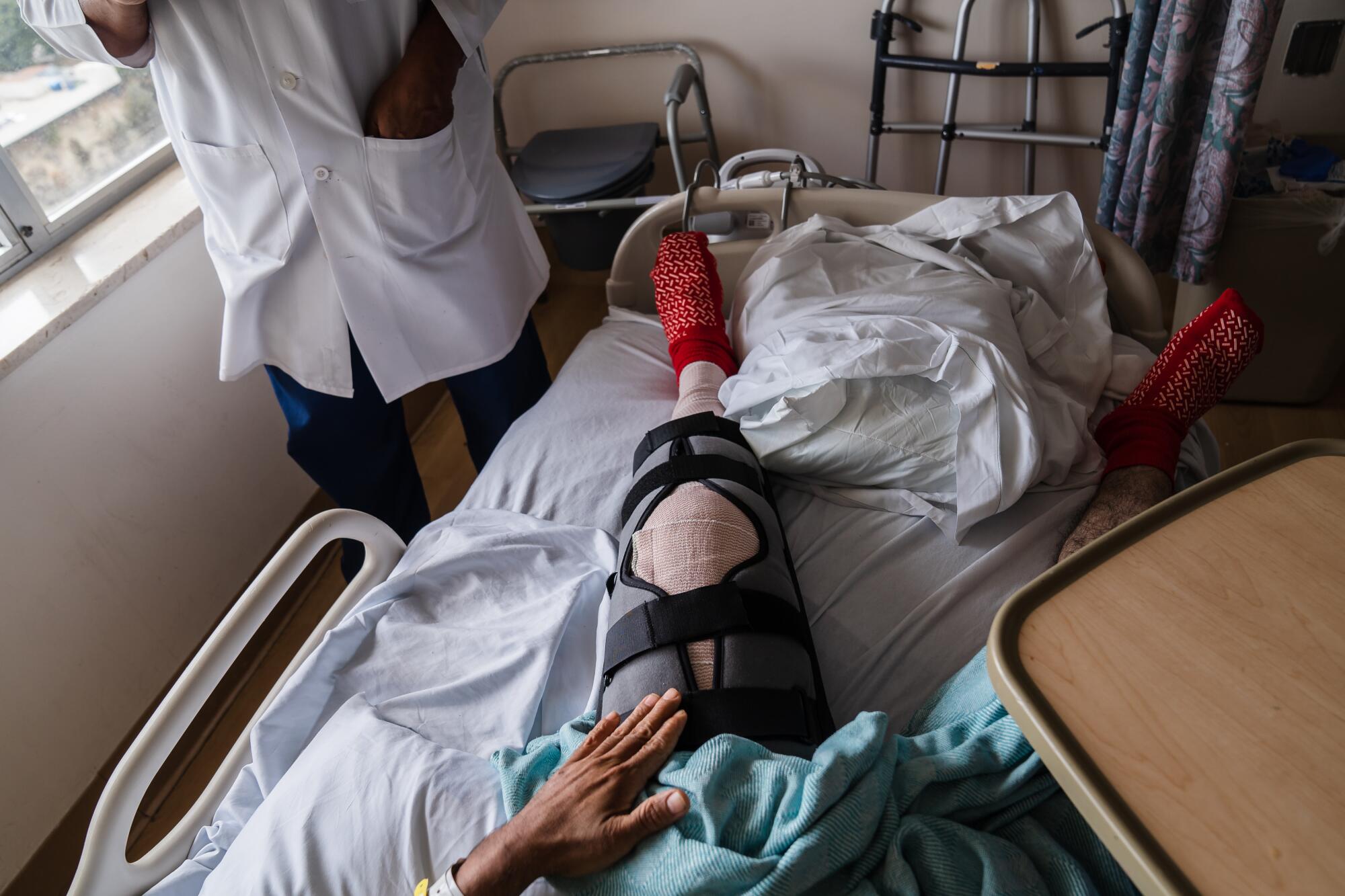
Her daughter had fractured her skull, her neck and back. She spent about a week in a San Diego hospital and is still mostly bed-ridden.
“It was the worst night of my life,” the woman said in Spanish. “We had come to save our lives, not to risk them in such an awful way.” She asked not to be identified because the rest of her family remains in danger in Tijuana.
Ever since the Trump administration increased the height of the border barrier to 30 feet, trauma doctors in San Diego have noticed a significant uptick in patients who have severe injuries such as these after falling from it. The people they are treating come from all over the world — Mexico, Central America, South America, Africa and Asia.
The two trauma centers that receive most border-wall patients — UC San Diego Medical Center in Hillcrest and Scripps Mercy Hospital — saw a more than five-times increase in such patients in 2019 through 2021, the three years after the new wall went up, compared with the three years prior, according to data provided by both institutions and analyzed by the Union-Tribune.
Doctors with UC San Diego Health published a research letter in the Journal of the American Medical Assn.’s surgery subjournal on Friday detailing what they’ve experienced with admissions to their trauma center.
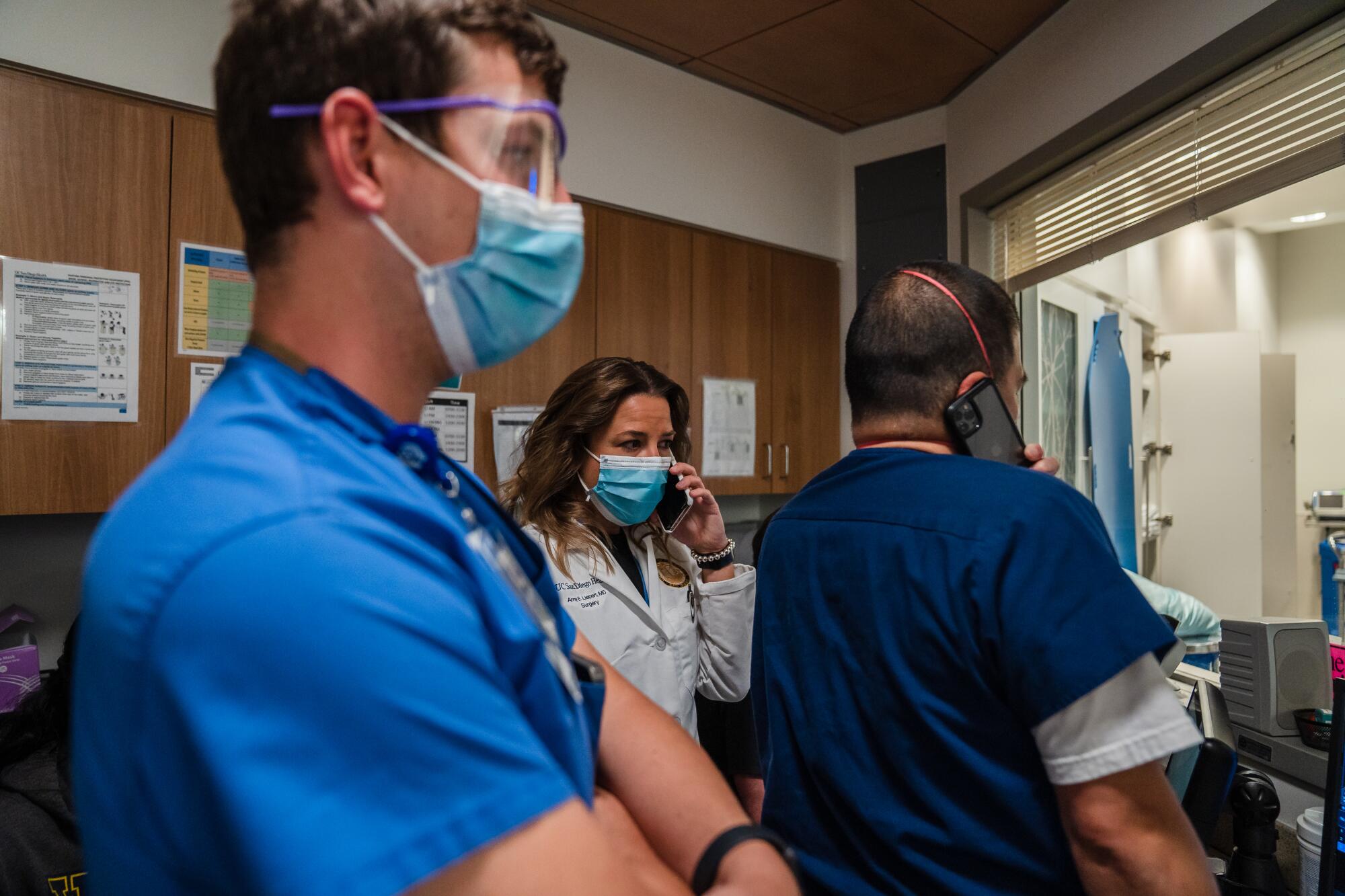
“It added stress to an already stressed healthcare system as we were trying to navigate effects of the pandemic and now the effects of a new or increased patient population,” said Dr. Amy Liepert, medical director of acute care surgery at UC San Diego Medical Center and the lead researcher for the letter.
The doctors found that the increase in admissions of border-wall patients was still significant when they controlled for changes in the number of border crossings.
In 2016, for example, UC San Diego Health admitted border-wall injury patients at a rate of about 49 people per 100,000 local Border Patrol apprehensions. By 2021, that rate grew to about 449 people per 100,000 apprehensions.
They also found that the severity of injuries, length of stay and cost of care had gone up significantly. And, for the first time, some of the people admitted with injuries from falling off the border barrier died.
Dr. Vishal Bansal, director of trauma surgery at Scripps Health, said that the change seen at his hospital has been astounding.
“It absolutely hasn’t tapered off,” Bansal said. “It’s getting worse.”
Deterrence and death
The idea of building a bigger border barrier — the border wall — started with former President Trump’s campaign and became a major point of contention throughout his administration.
Despite pushback, the Trump administration started several projects along the border that replaced barriers that were roughly 10 feet to 20 feet tall with the 30-foot bollards, or steel posts with narrow gaps that allow Border Patrol agents to see to the other side, that are now in place. That included two projects along about 14 miles of border in San Diego from where the barrier ends in the Pacific Ocean to the mountains that some say serve as a natural barrier.
The first project replaced the “primary fence” or the barrier closest to Mexico, which was initially made of rusted helicopter-landing mats left over from the Vietnam War and was erected in the 1990s. That replacement barrier varied in height, reaching 30 feet in some places but not everywhere.
The second project replaced the “secondary fence” farther into the interior of the United States and extended it, creating two rows of the formidable bollards that those desperate enough to reach the United States would have to find their way over, around or through.

Dr. Jay Doucet, chief of trauma at UC San Diego Health, said he was surprised by the uptick in patients because the wall had been touted as unclimbable.
Though the Trump administration was known for its efforts to block asylum seekers and other migrants from reaching the U.S., its actions followed a longtime trend in the United States of using deterrence measures at the border to keep people out. And this is far from the first time that those deterrence measures have led to increased injuries and fatalities.
When the previous barriers were installed, border crossings shifted to the mountains, deserts and ocean — places where the people trying to reach the United States are more likely to die en route.
Yet people kept coming.
The same has happened with the taller border barriers and the host of other border policies that the Trump administration put in place, some of which have been maintained by the Biden administration.
For the family from Michoacán, the decision to cross without permission felt like one they had to make.
The group of adult siblings, their parents, spouses and children fled the cartel violence that has caused many to leave the coastal state after their family was targeted and the woman’s husband was killed. They tried to ask for asylum at the San Ysidro Port of Entry, but they were turned away by U.S. officials.
That’s due to a pandemic policy known as Title 42 that says border officials can keep out asylum seekers and other migrants without legal status and expel those who are caught crossing into the United States without permission.
After the people hunting the family showed up at a relative’s home and beat him until he said where they were, the family returned to the port of entry to ask for help. But they were again turned away.
That same night, they climbed the wall.
Compound fractures, brain injuries
Scripps Mercy Hospital and UC San Diego Medical Center share responsibility for trauma cases originating on the border, switching off months and pitching in if one of them gets crowded.
Rady Children’s Hospital receives trauma patients under the age of 15, which probably is where the girl from Michoacán ended up, though her mother was so beside herself with worry that she doesn’t remember.
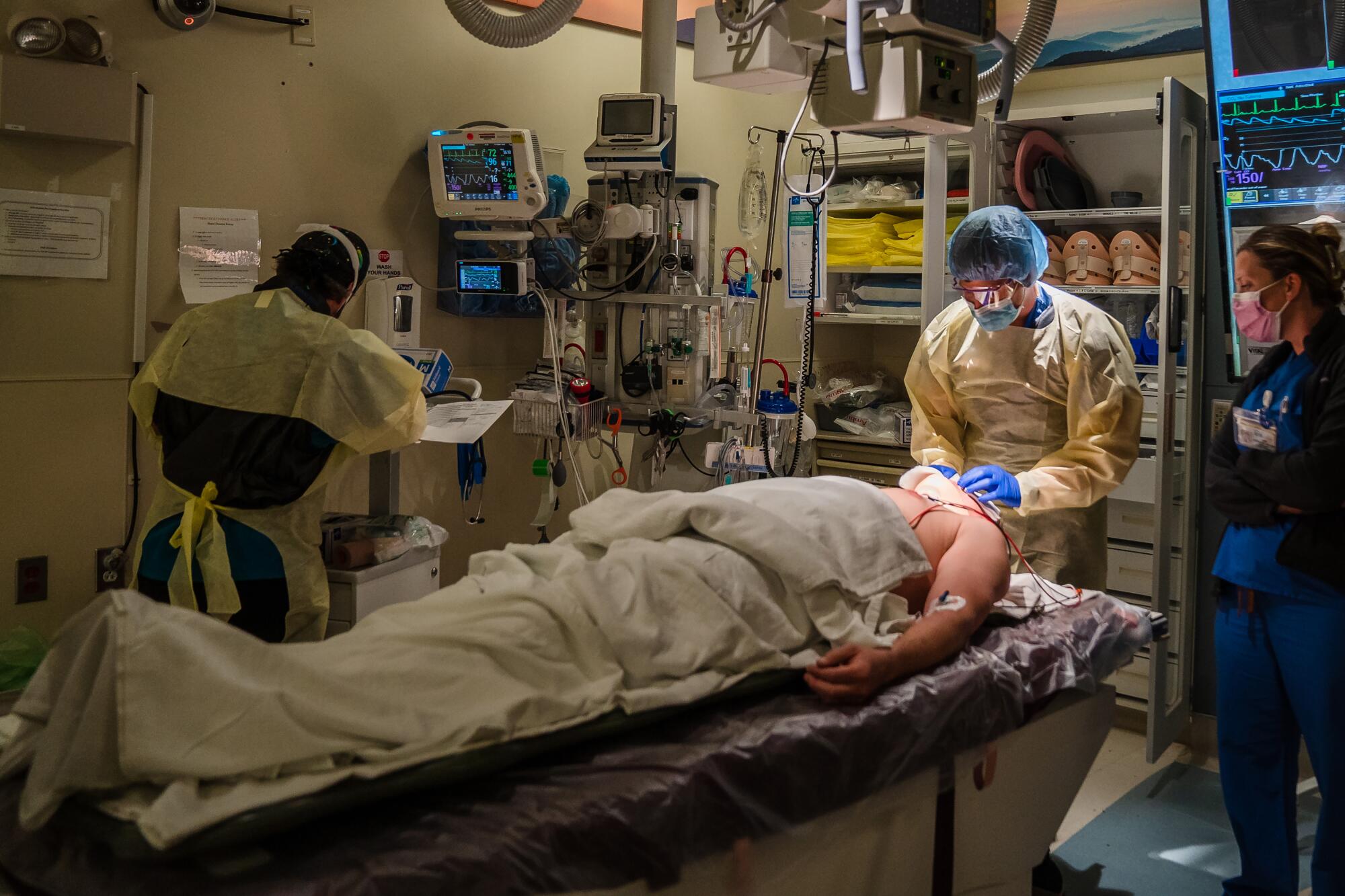
When people fell from the old barriers, doctors would see broken ankles, the occasional spinal fracture, but nothing like what is happening now, Doucet said. Both of the Hillcrest trauma centers are now tending to border patients with shattered limbs, fractures that stick out from the skin, broken skulls as well as brain and spinal injuries.
“We know from prior studies and looking at our own records that about half of people will die if they fall 40 feet,” Doucet said. “When you get to 30 feet, you’re starting to get to the range at which some people are going to die from that height.”
The team of doctors at UC San Diego Health asked the county medical examiner’s office for records of people who had died at the border wall because of falling. From 2016 through 2018, there were none. From 2019 through 2021, there were 14.
For those who don’t die, the long-term consequences of injuries can still be quite significant. Some will live the rest of their lives with pain or some kind of disability, Doucet said. Those with severe brain injuries may never regain the level of mental function they had before the fall.
Doctors haven’t been able to study the outcomes of their border wall patients because they’re generally not involved in any follow-up care that the patients receive, for several reasons.
Most lack insurance, and they can’t afford the out-of-pocket costs for ongoing treatment.
Also, most do not stay locally after they are discharged from the hospital. Though Border Patrol used to guard patients and keep them in custody, doctors have observed that agents have recently generally released those with severe injuries after a few days of guarding them.
In the case of the mother and daughter from Michoacán, the mother recalls that agents stayed with them for most of the week before disappearing. The pair were allowed to join family already living in the United States and will have to go through immigration court hearings to determine what ultimately happens to them. The rest of the family members who crossed with them were expelled to Tijuana while the girl was in the hospital.
The mother said she hasn’t yet been able to get follow-up care for her daughter.
Full operating rooms
In addition to complicating the lives of the people who fall from the wall, the extent of their injuries and the care they require also complicate resources at the hospitals that treat them.
“Orthopedic colleagues are beginning to burn out, and trauma surgeons are beginning to burn out,” Bansal said. “Our operating rooms are beginning to cancel some elective cases just because the burden is so high.”

The seriousness of the injuries has meant extended hospital stays at both institutions, which means more use of hospital beds, nursing staff and other hospital resources.
Bansal said patients at Scripps have been so injured that they stay in the hospital, on average, about six days, more than five times the 27-hour average for most trauma patients.
The doctors at UC San Diego Health found that the median length of stay for border-wall patients increased from about four days before the wall grew taller to about six in the years since. Some even stay for several months.
Their patients’ time in the intensive care unit also increased from about half a day on average to just over two days.
“This isn’t a fracture you get when you fall off your bike, and you get a cast on it,” Liepert said. “These are bones broken in multiple pieces that need to be pinned back together sometimes with external fixation devices.”
Once patients have healed enough, they have additional surgeries to remove those external devices, she explained.
The lack of insurance adds to the hospital stay, she added. These patients can’t be transferred to rehabilitation or long-term care centers, so they remain in the hospital for more of their treatment.
If the patients are in custody, the federal government will pay the hospital for the services provided, Doucet said. But once Border Patrol agents release the patients, it is up to the hospital to cover the cost of care if the patients can’t pay.
Liepert said the team of doctors at UC San Diego Health hoped that by publicizing what is happening, politicians and policy makers will consider in the future not only the consequences that border policies can have on the lives of people trying to cross, but also the effects that those policies can have on the healthcare systems that may end up receiving them.
She said that because she’s been so busy with work, she hasn’t been able to learn the stories of many of her patients. But one thing she has learned from them stays with her.
“What they’re willing to risk and give up — that I think has, outside of the medical pieces, struck me,” she said.
Staff writer Paul Sisson contributed to this report.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.














