Obamacare plans could be forcing people to pay extra for specialist care
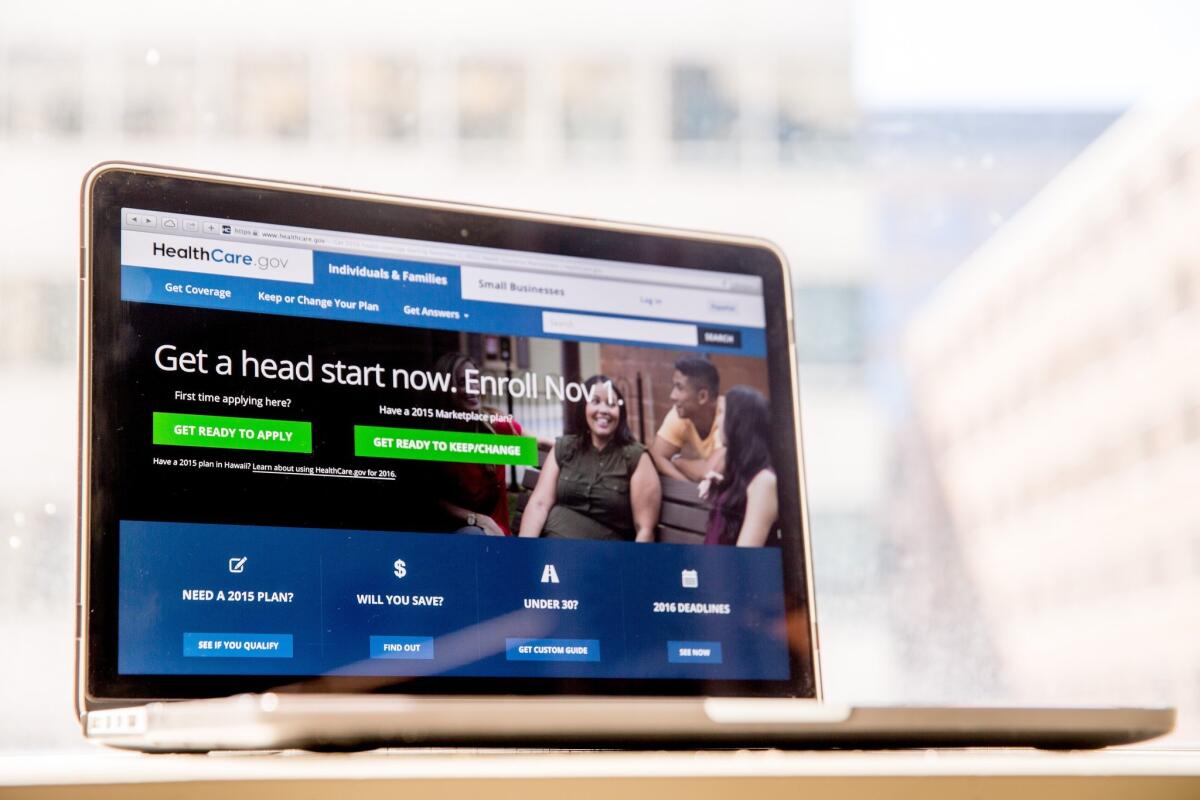
A new study shows that many of the plans offered through HealthCare.gov last year did not include specialists.
- Share via
Reporting from Washington — Many health plans sold through the Affordable Care Act in 2015 are so limited they don’t offer patients access to some medical specialists such as endocrinologists, rheumatologists and psychiatrists, a new study suggests.
That may be forcing some patients to pay thousands of dollars out of their own pockets for any care provided by these specialists.
“This translates into huge cost burdens for patients,” said Stephen Dorner, lead author of the study, published by the Journal of the American Medical Assn.
SIGN UP for the free Essential Politics newsletter >>
Health insurance plans sold on marketplaces created under the law are required to offer physician and hospital networks that are “sufficient in number and types of providers … to assure that all services will be accessible without unreasonable delay.”
But the rise of so-called narrow network plans that cover care at only a few hospitals and physicians’ offices is generating increasing criticism from patients and consumer advocates.
To test the extent of narrow networks, researchers at the Harvard T.H. Chan School of Public Health looked at provider directories in a sampling of 135 “silver” health plans being sold in the 34 states that relied on the federal HealthCare.gov marketplace in 2015.
They expected to find plans with only a handful of physicians in some specialties. Instead, they discovered that nearly 15% of the plans did not include a single in-network physician for at least one specialty.
See the most-read stories this hour >>
“We were definitely surprised,” Dorner said.
The plans with missing specialists either force consumers to pay the whole cost for any out-of-network care or require patients to pay more than 50% of the bill.
The study did not name the health plans or specify which states they are in, but researchers said they are scattered throughout the country in rural as well as primarily urban states.
Dorner said the findings suggest that state and federal regulators need to develop clearer network adequacy standards for health plans.
“Down the road, we likely will have to make sure [regulations] are sufficient and that we are guaranteeing patients access to affordable in access care,” he said.
The National Assn. of Insurance Commissioners is in the process of updating its suggested regulations to ensure health plans have sufficient networks.
Follow @noamlevey on Twitter
ALSO:
White House and Republican leaders reach budget deal
Girl in Vietnam War napalm photo gets laser treatments in U.S. to heal her scars
China, angered over warship patrol near artificial islands, warns U.S. not to ‘create trouble’
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.














