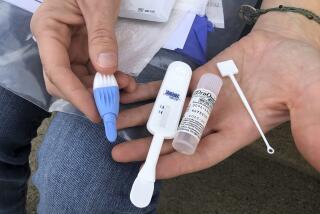
Anti-HIV drugs prove highly effective in preventing transmission of virus
- Share via
In what is being hailed as a breakthrough in HIV prevention, a new study has shown that giving antiretroviral drugs to HIV-positive people can reduce transmission of the virus to partners by 96%, U.S. researchers said Thursday.
Though some uncontrolled studies of populations had previously suggested that treatment of patients with antiretroviral drugs could slow transmission of the virus, the results announced by the National Institute of Allergy and Infectious Diseases represent the first large clinical trial to confirm those suggestions — and they showed that the drugs are unexpectedly effective.
In fact, the results of the study of nearly 1,800 couples in nine countries — mainly in southern Africa but including two couples in the United States — were so dramatic that the study’s sponsors decided to terminate it four years before its scheduled completion.
The study shows that not only does early treatment of HIV infections benefit the patient’s health, but also that “there is clearly a benefit of a profound decrease in the probability of … transmission to his or her own partner,” Dr. Anthony S. Fauci, the institute’s director, said in a news conference.
Antiretroviral treatment “can definitely decrease rates of transmission, and we can get this disease under control,” said Dr. Kathleen Squires, chairwoman of the HIV Medicine Assn. and director of the division of infectious diseases at Thomas Jefferson University Hospital in Philadelphia, who was not involved in the study. “This is scientific proof that this is true.
“This shows us that if we can identify the people who are infected and give them access to therapy, we can dramatically reduce the number of new infections in this country,” she said. Unfortunately, she added, there are waiting lists for the drugs in many states, chiefly because of underfunding of a government program that helps uninsured patients afford the drugs.
The clinical trial, begun in April 2005, was conducted at 13 sites in nine countries. Only two couples in the U.S. participated presumably because few patients wanted to run the risk of deferring treatment during one stage of the trial.
The trial enrolled 1,763 couples in which only one partner was infected: Those infected included 890 men and 873 women; 97% of the couples were heterosexual. All the infected patients had CD4 counts — a measure of the severity of the infection — between 350 and 550 at the beginning of the study. U.S. treatment guidelines now call for antiretroviral treatment to begin when a patient’s CD4 count falls below 500, but international guidelines typically require waiting until it drops below 350.
For half the couples — selected randomly — the infected member began receiving a cocktail of anti-HIV drugs immediately, and half had treatment deferred until the patient’s CD4 count fell below 350 or he or she developed an AIDS-defining complication, such as pneumocystis pneumonia. All the subjects received counseling on safe sex, free condoms and treatment for any sexually transmitted diseases that occurred during the study.
When the monitoring committee examined the interim results last month, they found 39 new HIV infections. Twenty-eight of the infections clearly came from the person’s partner, based on genetic analysis of the virus; seven were thought to have arisen from other sources; and four probably came from other sources but researchers were not sure.
Among the 28 who developed new infections that clearly seemed to come from their partners, 27 were in the group in which treatment with antiretroviral drugs was deferred.
“We were very, very surprised” by the magnitude of the reduction, said Dr. Myron Cohen of the University of North Carolina at Chapel Hill, who led the study.
The preliminary results also showed some benefit for the patients. The team observed 17 cases of disseminated tuberculosis — TB that has spread beyond the lungs — in the deferred-treatment group and only three in the immediate-treatment group. TB is a leading killer of HIV-positive people.
There were 23 deaths in the study, 10 in the immediate-treatment group and 13 in the other group. The difference was not statistically significant, and the researchers have not yet analyzed the causes.
“This is amazing news,” said Michel Sidibe, executive director of the Joint United Nations Program on HIV/AIDS. “Prevention can be a reality. The science is strong — so strong that we must use it.”
The finding should put increasing pressure on funding agencies to provide more access to drugs in developing countries, he said.
The $73-million study was funded by the National Institute of Allergy and Infectious Diseases. The 11 drugs used by participants were provided free of charge by the companies that make them. The cost of the drugs in the developing countries would normally be “a few hundred dollars per year,” Fauci said.
All patients in the study will receive the drugs for at least another year as Cohen and his colleagues monitor them to determine whether the findings bear out over time.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.